I recently received a call from a senior anaesthesiologist, a family friend who works at a large private hospital in Mumbai. He said he was becoming abnormally aware of his heartbeat over the last two months. Then the anxiety kicked in — he could not intubate a severely ill Covid-19 patient in the critical care unit. In his 35-year career, this had never happened. He froze, and another doctor had to take over. A sense of guilt continued to loom over him, and that’s when he called me, a psychiatrist.
Following an initial assessment over Skype, I determined that he was having a form of clinical anxiety. I put him in touch with a therapist who handled the non-pharmacological part of the illness. I started him on a short-term, low-dose anxiolytic. With medication and therapy sessions, he was soon able to gain control of his debilitating anxiety. This is just one incident – I have lost count of the number of people who have been reaching out to our organisation for help lately. When I checked about this with other colleagues, they also had similar stories to tell.
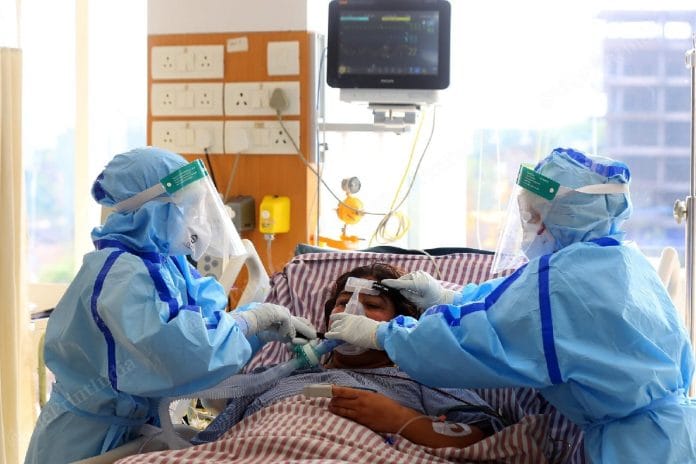
In India’s second Covid wave, the toll on our healthcare professionals seems to be far worse. Especially when it comes to their mental health. This phenomenon was not seen to this extent in the first wave. In the second wave, along with Covid-19 patients, healthcare professionals are also feeling helpless. I recently read that a resident doctor at a private hospital in Delhi died by suicide allegedly due to the frustrating situation he had to face on a daily basis. He had to deal with seven to eight critical patients every day in the Covid ward. He is survived by his two-month pregnant wife.
Among most doctors, nurses and hospital staff, chronic exhaustion, pandemic fatigue, feelings of isolation, loneliness, lack of opportunity to grieve, and inadequate closures are setting in. More and more are reaching out for help.
Also read: Second Covid wave is causing guilt, anxiety, distress, NIMHANS helpline sees 40% spike in calls
Doctors can’t be on auto-pilot
With barely a few months to recover after the first wave, the existing workforce has been stretched thin, and healthcare workers are having to shoulder additional responsibilities. Unless the frontline workers are adequately rested, we cannot expect them to discharge their duties to the best of their abilities. Healthcare workers are humans too, and cannot function on auto-pilot mode.
The overarching theme that is increasingly being seen among healthcare workers is fear. We have had several nursing professionals reach out to our team and say that they fear going back to the Covid ward.
Rekha (name changed), working at a Covid hospital in Karnataka’s Hubli, sought an online appointment.
“Doctor, I am in a catch-22 situation. My family and I can’t make ends meet if I don’t work. At the same time, I worry about stepping out into the Covid ward. I have this sense of restlessness throughout the day, and can’t wait to get back home. I am exhausted by the time I reach home. I then have to make dinner for my family. It is depressing,” she told us.
One question gnaws at every healthcare worker: “Am I inviting this untameable virus into my home?” Despite this being a very realistic fear, doctors and nursing personnel are left with little choice. They don’t have the luxury of not working on weekends, or of working from home. If they stop going to work, there will be no bread on the table. The irony of the situation is cruel. While they are working for survival, their very survival can come to a halt should they get infected.
Work is not easy either. A slight error in judgement can be fatal; we are talking about life and death situations. There is an acute shortage of beds, oxygen, and ventilators. This has forced doctors to make some hard choices — and that takes a mental toll of its own. A 70-year-old man who is on the brink of collapse needs the ventilator as much as a 30-year-old woman who is battling severe Covid-19. And there is only one ventilator available. Which guideline do we turn to in such a situation?
Dr Ram (name changed), an interventional cardiologist in Maharashtra’s Nashik, converted his state-of-the-art facility into a Covid hospital. He tells me that physicians at his hospital are under immense duress while making such hard choices. One of his physicians recently quit saying that he could no longer bear the mental fatigue accompanying such difficult choices.
How are we to process the scale of this trauma? Are we supposed to carry on from one patient to another as though nothing has happened? My brother-in-law, a neurosurgeon, and my sister, an obstetrician, tell me some harsh details of the kind of pressure that frontline workers are facing. I see both of them being completely drained by the time they come back home. Their only respite is the family dinner that we all have together, and even then, the conversations veer towards the degree of emotional exhaustion that healthcare workers have to bear.
Also read: Not all doctors think putting medical, nursing students on Covid duty is practical. Here’s why
Not just yoga
India doesn’t pay particular attention to mental health. But the second wave has exposed that denial too.
A study conducted by the Ohio State University College of Nursing has found that critical care nurses in poor physical and mental health committed more medical errors than nurses in better health. Approximately 40 per cent screened positive for depression symptoms, and more than 50 per cent screened positive for anxiety. The National Mental Health Survey 2015-16 conducted across 12 Indian states reveals that 1 in 20 Indians is clinically depressed.
A part of the solution lies in incentivising healthcare workers. Compensation and work-related benefits should be attractive enough to invite more workforce. The existing pay scale is discouraging, to say the least. In the unfortunate event of a healthcare worker succumbing to the virus, the family of the said worker should be adequately compensated.
Prescriptive practices such as doing yoga, exercising, engaging in mindfulness meditation are largely applicable to non-healthcare workers. In the middle of such a pandemic, it is impractical to expect healthcare workers to find the time to engage in such practices.
Incentivisation will hopefully attract more workforce so that the existing professionals find it a bit more easy to manage the work pressure and a rest cycle can be initiated.
Healthcare settings in India should take mental and emotional health seriously. In most medical colleges and hospitals, the department of psychiatry is relegated to a remote inaccessible corner, or may even be housed in a separate building, which is cut off from the main healthcare system. Integration of mental health into the general healthcare system should begin with easy access to mental healthcare. Psychiatry, as a subject, should be included in the undergraduate curriculum, and the final year curriculum should evaluate students with a separate theory and practical exam. This will serve to reduce the stigma surrounding mental health, and also make more doctors aware of the ground realities of mental healthcare in our country.
Hopefully, once we emerge out of this pandemic, we as a country, will make more of an effort to facilitate conversations around mental health. Of doctors and hospital staff too.
The author is Senior Consultant Psychiatrist, Manas Institute of Mental Health, Hubli. He tweets @alokvkulkarni. Views are personal.
(Edited by Neera Majumdar)