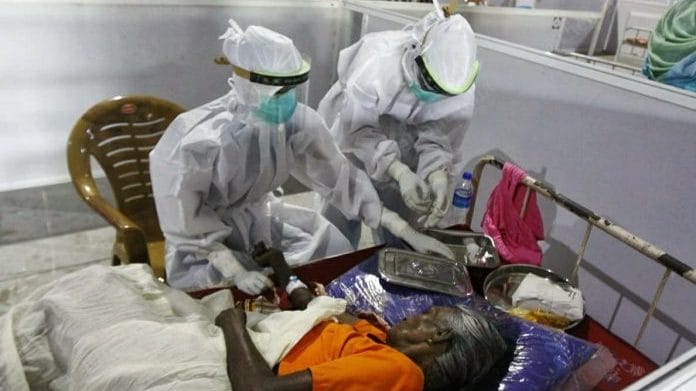
A catastrophic clinical outcome often triggers emotional turmoil, sometimes erupting into violence against doctors and hospital property. Though rare, such incidents spark doctor protests and the suspension of outpatient services. Doctors are no longer seen as ‘demigods’; the era of accepting poor medical outcomes as a fait accompli is over. The trusting patient has become a suspicious litigant. The credibility of the healthcare system is visibly eroding. Still, violence in any form is unacceptable in a civilised society.
Kerala is no exception to the circumstances delineated above, though violence is less frequent. But why does it occur in a state lauded by the NITI Aayog as a healthcare leader? Despite spending 1.1 per cent of its gross state domestic product on healthcare and having a strong public and private network, Kerala faces unique challenges: a greying population with a heavy disease burden, unregulated private hospitals that push people into poverty and unreported medical errors.
This paradox of high rankings amid rising health concerns calls for deeper scrutiny. The shift from Millennium Development Goals to Sustainable Development Goals in 2016 demanded reimagined healthcare systems. Has Kerala adapted? What policy changes are needed to meet new challenges? Should all public health resources be unified under one system to optimise outcomes?
This chapter explores the emerging issues and suggests reforms at both policy and service delivery levels.
Is Kerala the Real Topper?
Kerala has long been a pioneer in healthcare. Contributions from erstwhile rulers and missionaries boosted female literacy, a key factor in reducing maternal and infant mortality and improving immunisation rates. Successive governments built on this foundation, making Kerala a leader in reproductive and child health.
However, Kerala’s frequent health awards are often based on broad indices, not core measures like access, quality and cost. Critics such as Sundararaman and Indranil Mukhopadhyay argue that NITI Aayog’s health index is flawed and reflects past successes while ignoring present challenges and their economic fallout.
In contrast, global frameworks take a broader view. Bloomberg’s health index, for example, includes life expectancy, environmental risks and lifestyle factors. The Global Health Security Index assesses emergency preparedness across six dimensions, from prevention to system strength. Adopting such comprehensive tools could better guide Kerala’s future healthcare strategies.
Can Kerala adopt these broader frameworks to assess its performance in the health sector? Owing to the lack of data availability and integrity, it may not be possible to switch over to these frameworks. Over time, as health data for the population becomes available, Kerala could transition to one of these methodologies. However, as of now, fundamental issues that determine the functioning of the healthcare delivery system could be examined closely to find out where Kerala stands today. The following five core domains are worthy determinants:
- Appropriateness and quality of care
- Affordable healthcare services
- Equity issues
- Environmental protection
- Promotional and preventive aspects of healthcare
I explore the first three domains below.
Also read: Nehru’s enthusiasm, Jinnah’s silence, and Gandhi’s baffling indifference to Mohenjo-daro
Appropriateness and Quality of Care
Quality of care in healthcare refers to how well health services improve outcomes and align with professional standards. It includes safety, effectiveness, patient-centredness, timeliness, equity and efficiency – essentially, it means delivering the right care at the right time in the right way.
Globally, quality varies between hospitals and physicians, depending on factors like clinical support, staff skill, technology and patient cooperation. Medical errors, a serious quality issue, are often underreported and poorly investigated.
India lacks a national index of clinical and medical errors. Dr Girdhar J. Gyani, director general of the Association of Healthcare Providers (India), points out that healthcare staff are not trained to assess such errors. Professor Jha of Harvard Medical School estimates that 5.2 million medical errors occur annually in India.
A 2013 study by Nilay D. Solanki and Chaital Shah analysing 300 cases in a hospital in western India found that 117 cases (39 per cent) involved errors:
- 62 cases due to prescription errors
- 28 cases due to transcription errors
- 16 cases due to administrative errors
- 11 cases due to dispensation errors
Kerala has no studies documenting medical errors. Often, such errors are buried in records, with no disciplinary action by regulatory bodies like the Medical Council of India. This failure led to medical services being brought under the Consumer Protection Act in the 1990s. Currently, there are no standard benchmarks to assess doctors or hospitals. Outcomes are often attributed to patient-specific factors, not systemic failures. Without objective metrics, even excellent clinical recoveries may be undervalued if care lacks perceived quality.
Medical errors often occur at the point of care, especially when doctors face complex, multisystem issues without access to updated clinical evidence. Kerala publishes few scientific papers and medical colleges seldom contribute, forcing clinicians to rely on Western data, sometimes misclassifying normal findings as unhealthy. This results in unnecessary medication – a major source of errors. Patient education, a critical component of quality care, remains largely neglected, with no strong policy direction in place.
 This excerpt by Dr K Ellangovan from ‘The Kerala Club’, edited by KM Chandrasekhar and TP Sreenivasan, has been published with permission from Bloomsbury India.
This excerpt by Dr K Ellangovan from ‘The Kerala Club’, edited by KM Chandrasekhar and TP Sreenivasan, has been published with permission from Bloomsbury India.