As of mid-June, the Covid-19 pandemic has affected over eight million people and killed more than 430,000 people. If this was not bad already, the pandemic is wreaking havoc on every aspect of global health, from TB, AIDS and malaria to maternal and newborn health.
Even before Covid-19, TB was the leading infectious killer, with 1.5 million people dying every year. Then the Covid-19 pandemic hit, resulting in worldwide lockdowns and extensive disruption to routine TB diagnostic and treatment services.
Last month, the Stop TB Partnership published a modelling analysis predicting the long-term impact of the Covid-19 response on worldwide tuberculosis control. In the authors’ baseline scenario of a two-month lockdown followed by a gradual recovery to normal TB services over a two-month period, they estimated a 4 per cent increase in TB deaths between 2020 and 2025, equivalent to 342,000 excess deaths. In their worst-case scenario of a three-month lockdown followed by a 10-month recovery period, it was 16 per cent and 1.4 million excess deaths. This would represent a setback of at least five to eight years in the fight against TB.
Modelling for the WHO suggests that a six-month interruption to the supply of antiretroviral therapy in sub-Saharan Africa could lead to more than half a million excess deaths from HIV in 2020 alone, more than doubling death toll of 2018 and making this year the worst in the region since 2008. “The terrible prospect of half a million more people in Africa dying of AIDS-related illnesses is like stepping back into history,” said Dr Tedros Adhanom Ghebreyesus, Director-General of the WHO.
For malaria, 27 countries in sub-Saharan Africa, accounting for 85 per cent of malaria deaths in the region, were scheduled to undertake their three-yearly mass insecticide-treated net (ITN) distribution campaigns this year, a mainstay of malaria control. In the worst-case scenario of wholesale disruption to ITN distribution and a 75 per cent reduction in access to effective antimalarial treatment, modelling by the WHO predicts a total of 768,000 malaria deaths in sub-Saharan Africa this year, 70 per cent of them children under five, a figure higher than the global malaria death toll reported in the year 2000.
Also read: Focus on Covid-19 to increase malaria, tuberculosis and HIV related deaths in 5 years: Study
Bleak global health outlook
Outside the “Big Three” infectious killers, the global health outlook is equally bleak. Modelling published in the journal Lancet Global Health predicts an additional 417,000 to 2.3 million deaths from all causes in children under five in the next 12 months, pushing back progress on child mortality by between five and 15 years.
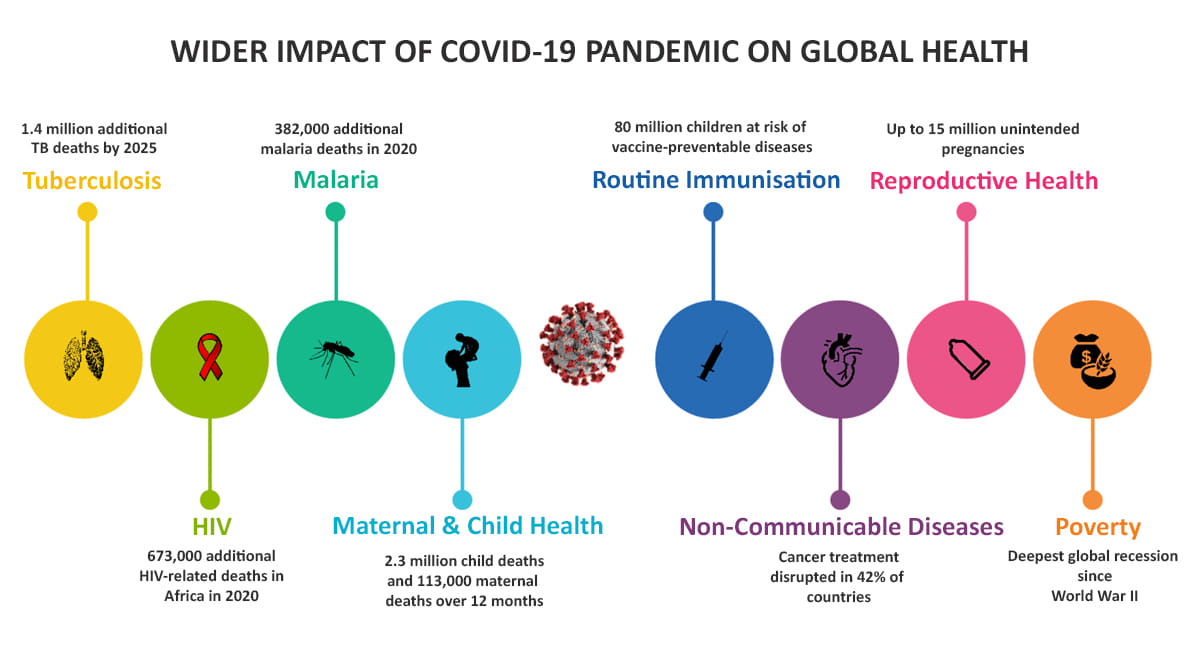
According to the WHO, at least 80 million children under one are currently at risk of vaccine-preventable diseases such as measles, mumps, rubella, polio, yellow fever, typhoid, cholera and tetanus, as routine childhood immunisation services have been disrupted in at least 68 countries. There may also be a large increase in the number of children born in the world next year. Modelling for the United Nations Population Fund (UNFPA) estimates that between 13 and 51 million women in 114 low- and middle-income countries will be unable to access modern contraceptives, depending on the length of lockdown and the level of health service disruption, leading to an additional 325,000 to 15 million unintended pregnancies.
The impact of Covid-19 is also being felt in the area of non-communicable diseases (NCDs). According to a recent WHO survey of 155 countries, more than half of the nations reported that services for NCDs have been partially or completely disrupted. This means people with conditions such as cancer, diabetes and cardiovascular diseases have not received adequate care during this crisis.
The impact of Covid-19 will be largest in the poorest countries. The UNFPA expects stock-outs of contraceptives within the next six months in more than a dozen low-income countries due to supply-chain disruptions, with an increase in unintended pregnancies potentially exacerbating the risk of malnutrition in families already struggling for food. The Lancet Global Health study mentioned above predicts an additional 24,000 to 113,000 maternal deaths in the next 12 months due to disruption of care before, during and after childbirth. A wave of unintended pregnancies next year could make things even worse.
Also read: TB patients badly hit by lockdown — 80% drop in diagnosis, huge struggle for medicines
Worsening poverty
Most worrisome among all this bad news is the worsening of global poverty, a major driver of poor health. The latest World Bank report predicts a 5.2 per cent contraction in the world economy in 2020, the deepest global recession since World War Two. Another estimate suggests there could be increases in poverty of a substantial magnitude — up to 400 million new poor living under the $1.90 poverty line, over 500 million new poor living under the poverty lines of $3.20 and $5.50.
Mathematical modelling can only give an estimate of what may be coming — nobody can precisely predict the future—but what we learn from the models should give us pause. Covid-19 is a novel and severe threat to human health, and an unprecedented draw on our global attention, but we must not forget that the old threats remain.
If we shift all our resources and attention to the pandemic, the world may find itself on the brink of a different humanitarian catastrophe. Even if we avoid the worst of those modelled scenarios, years or even decades of progress in global health will undoubtedly be undone. None of the health-related Sustainable Development Goals (SDGs) might be met.
Also read: India could see millions pushed into extreme poverty due to pandemic: World Bank analysis
What countries need to do
All countries must dig deep and find new funds to deal with the Covid-19 crisis, and not take money away from TB or AIDS, or maternal and child health. This cannot be a zero-sum game. We need to urgently tackle the coronavirus pandemic, and simultaneous deal with other existing health priorities.
All countries must resume and ramp up routine health services, including essential services such as immunisation, contraception, maternal and child care, treatment of common conditions such as AIDS, TB and malaria.
In the long run, all countries must invest in universal health coverage (UHC). Without UHC and stronger health systems, there is no pandemic preparedness. Without UHC, the next pandemic will be even worse.
Jacob Bigio is a physician and a postdoctoral research associate in global health and epidemiology at the Research Institute of the McGill University Health Centre, Montreal, Canada.
Madhukar Pai is a physician & epidemiologist, a Canada Research Chair in Epidemiology & Global Health at McGill University, Montreal, Canada, and Director of the McGill International TB Centre.
Also read: US President Trump’s WHO exit endangers fight against polio, tuberculosis along with Covid





