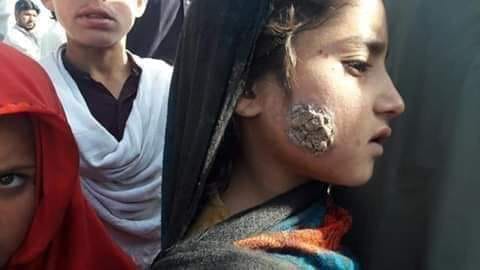
Bengaluru: In the last six months, nearly 30,000 cases of a parasitic disease — leishmaniasis — have been detected in Pakistan.
In India, leishmaniasis has been historically prevalent in Bihar, Jharkhand, West Bengal, and Uttar Pradesh.
The disease is caused by protozoan parasites of 20 Leishmania species. These parasites are transmitted to human bodies by the bite of infected female sandflies. Over 90 sandfly species are known to transmit Leishmania parasites.
The disease most commonly affects the skin, covering it with sores that take months to heal, sometimes leaving life-long scars. It is more common in tropical areas, affecting countries across the equatorial belt. It is classified as a neglected tropical disease, which is more commonly found in low-income countries.
The disease even affects dogs and rodents.
Three forms of leishmaniasis
The most common is the cutaneous form in which large sores appear on the area where the sandfly bites. These look like skin ulcers and can take several months or a year to heal. Sometimes, the scars can look like deep cuts and even resemble leprosy. The ulcers are prone to bacterial infection. This is, however, the mildest form of the disease.
The second form is the mucocutaneous form, which affects not just the skin but also the mucus glands. In this form, parts of the human body that produce mucus, such as nose and mouth, get damaged. Painful ulcers occur on mouth and nose that stay on for months.
The third and deadliest form of the disease is the visceral form or commonly known as ‘black fever’ or kala-azar. This can often be fatal if not treated properly. In a time period ranging anywhere from a few months to a few years since the bite, an infected person can start exhibiting symptoms such as fever, weight loss, reduction in blood iron levels, and damage to internal organs like liver, bone marrow, and spleen.
Also read: India announced end of leprosy 13 years ago, but 1.3 lakh cases were detected in 2016
Risk factors
Major risk factors associated with leishmaniasis are socio-economic conditions — malnutrition (lacking protein, iron, zinc) and poverty.
Apart from these, the World Health Organisation (WHO) also lists population mobility — where non-immune people move to infected areas or forests — and climate change — where fluctuations in temperature and rainfall can change the leishmania developmental cycle — as the major reasons.
According to the International Association of Medical Assistance to Travellers (IAMAT), researchers, army personnel, adventure travellers, bird watchers, missionaries, and construction workers, who work in night shifts, are at a higher risk of being exposed to sandflies.
Disease affects 1 million people worldwide each year
The disease occurs in varying frequencies in various parts of the world. In East Africa, ‘black fever’ or the visceral form of leishmaniasis is common and frequent. The situation is similar in countries like Iraq and Sudan.
In South America, the cutaneous form occurs more frequently, with Brazil making up for 90% of the cases. In South East Asian countries, both cutaneous and visceral forms are prevalent.
Almost a million people worldwide are affected each year by the disease, with anywhere between 25,000 and 65,000 dying of its various forms, according to WHO.
Also read: On World Health Day, a look at what ails India and status of Ayushman Bharat
Prevention and treatment
The disease, in all of its forms, can be diagnosed only when sores begin to appear. This can happen any time between some weeks and months after the bite.
Leishmaniasis can be first prevented by using an easily available deterrent for sandflies — an insect repellent.
The active ingredient DEET, present in most insect repellents, is said to work well. WHO-certified insect repellent icaridin, also known as picaridin, is also advisable. Mosquito nets, especially when sprayed with insecticide, can also be effective.
According to WHO, disease monitoring programmes must focus on effective disease surveillance and tracking to take prompt action.