Bengaluru: The herb giloy has long been touted as a carrier of multiple medicinal benefits, with ayurveda practitioners waxing eloquent about its purported anti-inflammatory, anti-fever, and even anti-cancer properties.
But never before perhaps has the herb pervaded Indian households like it has during the Covid pandemic, with people stocking it up in different forms — tablets, syrups, powder, or just its roots and stems — influenced by its much-publicised “immune-boosting properties”.
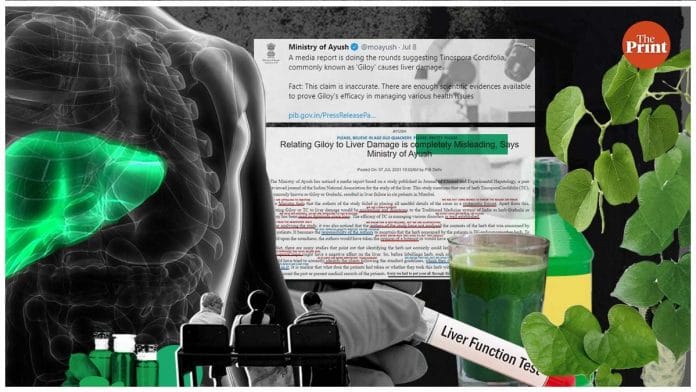
Earlier this week, however, the herb became a flashpoint between a group of Mumbai-based doctors and the Union Ayush ministry over a small study that sought to link it with liver damage.
Carried out by doctors affiliated with Jaslok Hospital, Mumbai, and Apollo Hospital, Navi Mumbai, the study was published in the peer-reviewed Journal of Clinical and Experimental Hepatology, published by the Indian National Association for Study of the Liver, which seeks to promote hepatology (focusing on liver diseases and conditions).
It involved six patients who, according to the researchers, had suffered extensive liver damage and were found to have consumed Tinospora cordifolia (TC) — the scientific name for giloy — in the preceding days.
Following the publication of the study and media reports around it, the Ministry of Ayush, a government department dedicated to the promotion of the alternative medical systems of ayurveda, yoga & naturopathy, unani, siddha, and homoeopathy (Ayush), issued a statement that challenged the findings. It said the authors did not “analyse the contents of the herb”, adding that it is the “responsibility of the authors to ascertain that the herb consumed by the patients is TC and not any other”. It claimed such studies could be “misleading and disastrous to the traditional medicine system of India”.
The researchers themselves acknowledged certain limitations to their study, including that they did “not analyse the contents of the plant parts which the patients had consumed” before being admitted.
Even so, doctors criticised the ministry’s statement as being a “knee-jerk” response, noting that the supposed benefits of giloy are not backed by scientific literature.
Erratum:
Giloy and Liver Injury#FactCheck pic.twitter.com/NUgDVUOCPg
— TheLiverDoc (@theliverdr) July 7, 2021
“Ayush Ministry’s press release on the recently published peer-reviewed case series on six patients developing severe autoimmune mediated liver injury was only a knee-jerk response,” said Dr Abby Philips, a hepatologist at the Liver Institute, Rajagiri Hospital at Kochi.
“The ministry’s claims of giloy being ‘safe’ are not backed by any evidence from published literature, and without supportive pharmacovigilance data,” he added.
It is a burden that dogs ayurveda as a whole, as it is seen as being short of the kind of scientific rigour usually involved in the development of drugs.
Further, doctors scoff at the very idea of certain food products boosting one’s immunity, dismissing it as commercial dog-whistling.
While purported immune-boosters have flooded the markets for ready purchase without prescription, even ayurvedic practitioners themselves warn against consuming excess quantities of such herbs, and advise sticking to quantities recommended.
Also read: How a bacteria is helping revive an endangered ayurvedic herb in CSIR labs
What is giloy?
Giloy goes by many names, including guduchi. A climber with heart-shaped leaves, it is a commonly used herb in ayurveda.
Its purported ability to boost immunity has also made it a part of Ayush Ministry’s Covid management protocols.
The study in question was a hospital-based observational exercise conducted at the Jaslok Hospital and Research Centre in Mumbai on six patients who reportedly suffered herbal-induced liver injury between September 2020 and December 2020. They were followed up with until March 2021.
All participants were adults with acute hepatitis or liver inflammation. They were shortlisted after ensuring that they didn’t consume significant amounts of alcohol, and that hepatitis was not induced by other reasons, the researchers said.
The study outlined the individual cases, and their final outcome.
Case 1 involved a 40-year-old man without comorbidities. The patient had consumed 10-12 pieces of giloy boiled with cinnamon and cloves in half a glass of water, once every two days, for three months. His liver showed evidence of necrosis or death of tissue. He was taken off the herb and took five months for normalisation of liver function.
Case 2 was a woman aged 54 with Type 2 diabetes. She had a seven-month history of boiling and consuming the extract of 1 giloy twig a day. Her liver, the researchers said, had presented more extensive damage. Her symptoms resolved under medical care, the researchers added.
Case 3 involved a 38-year-old male Covid patient with beta-thalassemia minor (mild anaemia). He had consumed giloy extract from 3-4 twigs boiled daily for six months. His symptoms resolved as well.
Case 4 was the only patient that died. The patient was a 62-year-old woman with Type 2 diabetes, who had complained of reduced appetite, fatigue, and yellow discolouration of urine. She also had a swollen abdomen and puffy eyes and skin. She had been consuming a commercially available giloy product every other day for a month. She had already started to show cirrhosis or late-stage liver damage — where liver tissue is replaced by scar tissue — by the time she came to the hospital. She was treated with steroids and diuretics, and put on a low-salt diet. The patient improved initially but eventually succumbed to hepatorenal syndrome (HRS) 120 days after it was first diagnosed.
Cases 5 and 6 were both 56-year-old women with hypothyroidism. One had developed yellow discolouration in her eyes and urine. She had been consuming giloy for three weeks, three times a week. She had also started to show signs of auto-immune cirrhosis, and was put on maintenance-dose steroids at the end of the study. The other patient had jaundice and had been consuming a commercial giloy tablet a day for three months. She showed signs of autoimmune hepatitis, and after two months, there had been no relapse.
Among other things, the doctors noted that the patients improved on TC withdrawal.
“The drug may have benefitted some through its immune stimulant action given the fact that it seems to have triggered an autoimmune process (where the immune system attacks healthy cells by mistake). However, there is a need to urge caution and a warning about the potential to cause liver toxicity,” the researchers wrote.
Doctors say the emergence of giloy-related adverse events are among the outcomes of “unreasonable promotion of clinically untested herbal” remedies. “This has become a worthless but damaging exercise in public healthcare,” added Philips.
Also read: Take action against Ayurveda, Unani drugmakers over misleading ads — Modi govt tells states
Ayurvedic science
Ayurveda — which translates to “science of life” — is based on medicinal herbs. Its practitioners describe ayurveda as a “holistic” system of alternative medicine that also includes practices that calm the body, such as massages, yoga, meditation, pranayama, and a healthy diet.
While several herbs contain important micronutrients that could help the body, there have been concerns about lack of research, as also the quality of research and misleading claims, backing their promotion for health and fitness, especially when serious diseases like hypertension and heart conditions come into play. Some have gone so far as to describe ayurveda as a “pseudoscience”.
Ayurvedic drugs and preparations are banned in several countries, including Canada and Europe, due to the reported discovery of high levels of lead, mercury, arsenic, and other heavy metals toxic to humans.
Since the liver is the organ where drugs metabolise and are excreted, it — and sometimes the kidneys — is the target for injury from drugs, and this condition is called drug-induced liver injury (DILI).
The first case of hepatotoxicity or liver poisoning from ayurvedic drugs was reported only in 2009 but it has since been consistently linked to liver injury in multiple people globally.
“In my personal experience, I’ve seen that those with comorbidities, women, and people with autoimmune liver conditions tend to develop an injury similar to autoimmune liver disease [on consuming giloy],” explained Dr Chetan Kalal, a hepatologist at the Mumbai-based H.N. Reliance Hospital. “Either the body’s immunity acts against the liver or it triggers a latent autoimmune condition.”
Added Philips, “I see 2 to 3 new cases of ayurvedic herbal drug induced liver injury per week, i.e., upto 14 cases a month.”
“Interestingly, among the ayurvedic drugs I have retrieved from patients who developed herbal liver injury, the most common component is giloy,” said Philips, who has published peer-reviewed data on nearly 100 patients over the last three years.
A team led by Philips was the first to identify autoimmune liver injury associated with ayurvedic herbal medicines and giloy in 2018. Four of the six patients in the new study also had associated autoimmune conditions and liver injury. A 1997 study also found associated autoimmune markers from the use of giloy and related herbs.
Kalal explained that when there are no obvious causes for liver injury, it is often diagnosed as DILI and hepatologists insist on patients’ record of alternative medicine use.
“Most patients would have consumed some over-the-counter alternative medicine,” he said. “It is common and well documented in the medico community. If at all, people should ideally be taking these only under supervision and medical guidance, and their liver profile with baseline liver parameters need to be monitored.”
”People should also document and monitor any side effects,” he added.
Philips said the “evidence for giloy and its benefits in current medical literature is confined to preclinical and small animal studies that cannot be extrapolated for human use”. “At present, there is no safe dose of giloy that can be recommended as prevention or for a disease.”
This report has been updated to correct a typo
(Edited by Sunanda Ranjan)
Also read: Why India needs to regulate Ayurveda to win the world market for natural remedies