Global coronavirus pandemic battle is led by an army of medical doctors, nurses, paramedics, and researchers. Italy — where nearly one-tenth of the infections are among medical workers — should make two things impossible for us to overlook. First, that depletion due to disease of an already inadequate workforce will spell disaster for India. And second, that inadequate personal protection for our healthcare workers can itself wreak infectious havoc in our hospitals.
As the crisis looms large, it is time for India to look for ways to incentivise its health workforce like Indonesia, Malaysia and China.
Broken healthcare system
In India, healthcare workers have been working overtime and risking their lives every single day, while striving to save the lives of others. And add to the bargain the largely unconducive milieu in which they are fighting this fresh battle. The reasons that have contributed to the hardships of doctors are many, including deficient stocking of personal protective equipment (PPE) while allowing their export and evacuation of doctor’s quarters in certain hospital campuses to build quarantine facilities.
At places, healthcare workers have been compelled to carry their own PPE, forced into duty despite personal exigencies and even ousted from rented accommodations owing to fear of contagion. Add to this our woeful staff-population ratios, with a shortage of nearly 6 lakh government doctors and 2 million nurses. There have been positive developments too, including the nationwide lionising of healthcare workers as Covid-19 warriors, and the announcement of a Rs 50 lakh insurance cover, but more would be needed. And this gap will be felt more and more acutely as stage 3 of the pandemic looms on the horizon. Based on this understanding, we make these suggestions.
Need for monetary incentives
Research shows that both monetary and non-monetary incentives significantly impact the motivation of workers across the professional board – such that even a mere act of collective clapping can work wonders. Further, targeted and ad hoc incentives aren’t new in the healthcare landscape. The Indonesian government announced incentives of up to Rp 15 million for medical doctors and nurses, in addition to a compensation of Rp 300 million in case of death due to coronavirus. In Malaysia, the government announced a special monthly critical allowance of 400 Malaysian ringgit from February 2020 till the end of outbreak for medical staff fighting Covid-19. In China, children of frontline health staff in Hubei province will be awarded with extra points in school and higher education admissions.
While a Rs 50 lakh insurance cover is a good step forward, we propose special incentives like other countries for frontline medical staff tackling Covid-19 in India. Also, given that incentives pegged to number of hours worked and similar other criteria would be largely infeasible in the context of an emergency, a flat incentive system based on healthcare worker category can be conceived. With efforts to rope in medical staff from all quarters already underway, a special incentive can greatly hasten and enhance human resource mobilisation and retention. Further, the fact that we are still in the early stages of the epidemic will only facilitate incentive-driven workforce reinforcement, helping us bolster our capacity to confront future stage three excesses.
Also Read: India’s fight against Covid-19 needs wartime industrial production, not more red tape
Enhance health workforce
The best healing touch for a Covid-19 warrior in this situation would be to add to the deficient workforce. The NITI Aayog has already invited applications for volunteer medics. However, simple addition without appropriate planning will lead to wasteful use of vital resources. The lockdown that is currently underway allows some time for this planning and reinforcement exercise.
With that being said, different categories of ad hoc staff will suit different roles, which will be equally important. While medical specialists from allied departments can buttress critical care capacity after focussed, short-term training – medical students and interns could help offload routine outpatient and elective medical work, and even contribute to handling non-critical Covid-19 cases. In the US, medical students have been involved in ‘phone triaging’, a technique of screening out mild cases over the phone, so that only severe ones reach the hospital casualty.
As has been suggested already, roping in the vast pool of traditional medicine and foreign medical graduates will be imperative. In the state of New York, US, licensing requirements have been modified to allow foreign medical students to provide patient care in hospitals. We believe that the current pandemic can provide a useful window of opportunity to curb the opposition to bridge courses for allied medical graduates.
In addition, frontline healthcare workers should be assigned age categories and preferably younger cadres should be recruited as the first line. The second line cadres should be held as reserves for excesses or recruited during relatively non-peak hours. Further, particularly in anticipation of a prolonged Covid-19 presence in the country, avoiding acute and chronic staff fatigue becomes crucial.
Also Read: All essential service providers should be periodically tested: Scientists in open letter
While hospitals may possess an urge to employ staff for long shifts, it can significantly elevate the chances of getting infected due to fatigue-driven breach of personal protection. Too short and frequent shifts would also be counterproductive. A better balance would be to mandate not more than eight hours of continuous work, 12 hours in case of exigencies. While a decree in this direction is desirable – neither do our present numbers support such a luxury, nor does our track record in this respect seems promising.
Task shifting is another important measure that would need to be emphasised. Shifting bureaucratic workload of existing and potential clinical staff can help free up a considerable skill pool. This can range from simple reduction of paperwork for clinical staff to a change of staff portfolio, as for those doctors holding administrative posts. Apart from these, makeshift arrangements for lodging frontline staff within the hospital premises will need to be both augmented and insulated.
While appreciating the enormity of what needs to be done, we must also acknowledge the reciprocal duty that we as a society owe to our healthcare workers, who today face a disproportionate share of the Covid-19 risk. At the end, it is they who largely hold the key to a successful Covid-19 rescue.
Dr. Soham D. Bhaduri is a Mumbai-based physician and editor, ‘The Indian Practitioner’. Dr. Apurva Jain is an MPH candidate at TISS, Mumbai. Views are personal.



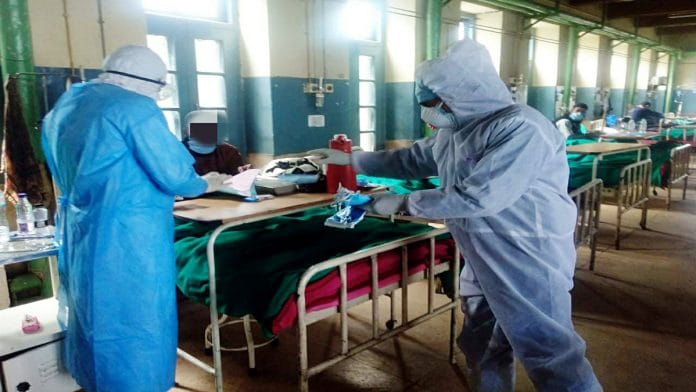


Very correct. The immediate need is good quality PPE, sufficient equipment and enough trained staff. Tali, Thali and lighting diyas are the jokes played on health workers. What they need are hygienic working conditions, security, decent living quarters and uniform stipend across India. In fact more care is needed of health workers. Then only they can take care of patients. Govts. can use this pandemic to start repairing restoring the hospitals.
Looking for solutions in the midst of epidemic is like a student starting preparation for exam one night before the exam. Huge deficits in healthcare sector due to neglect by successive govt are becoming visible during the pandemic situation. Govt has given 3 days time to states to find the number of PPE, drugs and other emergency equipments which itself shows the lack of understanding in the people sitting at the highest offices. Can u wait for 3 days in a pandemic situation? Provide first PPE, ventilators, extra staff and then think about financial incentives.