India cannot control the spread of the Covid-19 epidemic unless the governmental authorities stay in mission mode and get better at the ‘test, trace and isolate’ strategy, as I wrote in my column a couple of weeks ago. The first and most important part of the epidemic control strategy is testing, for only when you test lots of people and get the results quickly will you be able to trace their contacts and isolate them all.
Covid-19 cases across India are rising because the country is just not testing enough people, and test reports are taking too long to come out. And the main reason why India is falling far short of its capacity to test is that governments have failed to engage private laboratories and healthcare facilities in a reasonable manner. How else can you explain the fact that while there are abundant numbers of test kits available in the country, India ranks among the lowest in terms of tests per capita? Philippines, Malaysia, Rwanda and Cuba test more people per day relative to population than India does.
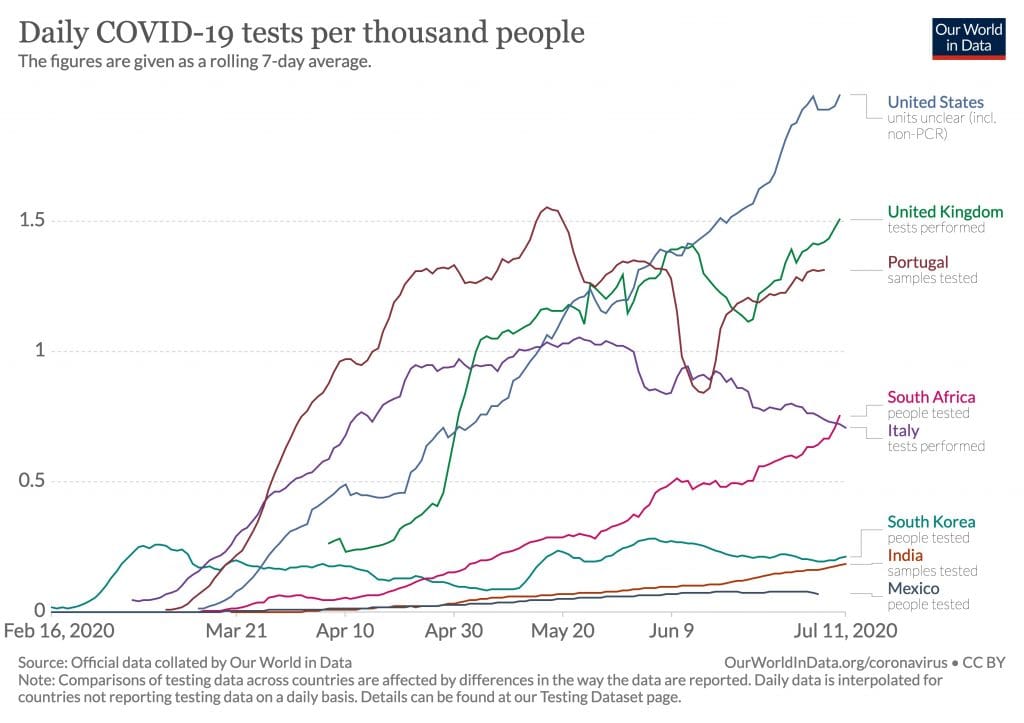
To be sure, India’s test rates have certainly increased over the past couple of months and are currently around 2,80,000 per day. Since the Union health ministry has not announced a national benchmark to guide health authorities at the state level, the situation is like a team batting second having to chase an unknown score at an unknown asking rate.
Also read: Covid testing numbers on rise, but states are feeling the pinch of high RT-PCR costs
Capacity is not the problem
My colleagues at the Takshashila Institution have proposed that every administration test a minimum of 2,500 people per week, for every million of the population; until the test positive rate is less than 1 per cent. By this count, India ought to be testing a minimum of 4,60,000 people per day and should ramp up this number until the test positivity rate falls from the current 10 per cent to less than 1 per cent. This possibly means we should be testing a million or more people every day — nearly four times as many as we are currently doing. As the analysis done by Karthik Shashidhar (see chart) shows, very few states and union territories are meeting even our minimum benchmark.
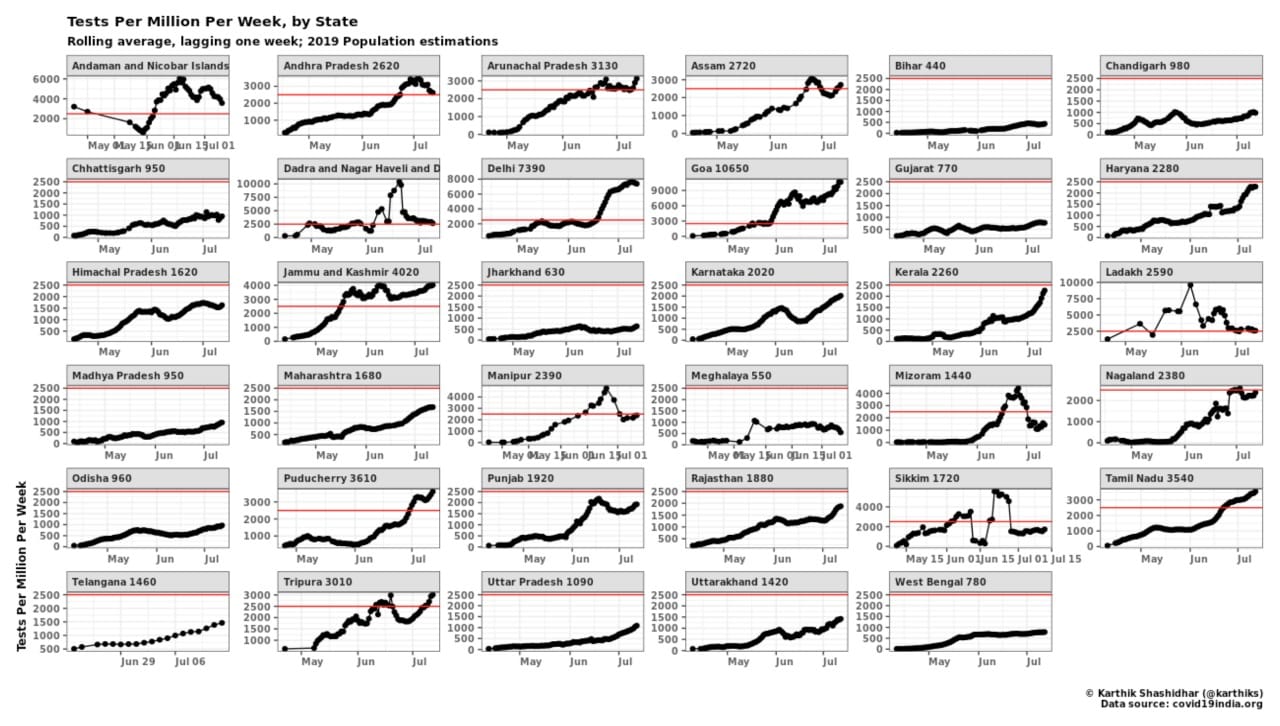
Why has India been slow in ramping up the testing rate? In the early days of the pandemic, it could be argued that we did not have enough labs and test kits. This is no longer the case. The Economic Times reports that “Indian companies have the capacity to make 146 million RT-PCR test kits a month, or 4.87 million kits a day”. Just one company, Pune-based MyLab Discovery Solutions, can produce 2,00,000 RT-PCR test kits per day. Yet, here’s a shocking fact — many domestic test-kit manufacturers are either cutting down production or appealing to the central government to allow them to export these test kits, because the domestic demand is low.
Also read: No need for govt doctor prescription for Covid test, contact-tracing must: Modi govt to states
The real cost of testing
The reason we are in this unconscionable situation is that many state governments have capped prices so low that very few private laboratories are interested in the business. The price that state governments pay private laboratories for an RT-PCR test varies from Rs 2,000 (in Uttar Pradesh) to Rs 3,000 (in Tamil Nadu), but are generally in the range of Rs 2,300. All are lower than the Rs 4,500 price cap earlier set by the Indian Council of Medical Research (ICMR). With the cost of materials itself falling in the range of Rs 1,800-Rs 2,000 per test, government policies have made testing feasible only for laboratories with massive economies of scale, or for unscrupulous ones that cut corners.
When determining costs, civil servants often ignore operational expenditures private firms have to incur. Sample collection personnel, data entry staff, material handling and hazardous waste disposal pose significant overheads beyond the costs of test kits. These have clearly been ignored by the government. With wafer-thin margins, few private laboratories have the capability to invest in more testing capacity or hire more people to speed up the testing.
In other words, India’s inability to test adequately despite having the capacity to do so is primarily because of price caps. This is hardly an unexpected outcome — in fact, it was entirely foreseeable and indeed foreseen.
What really is unfortunate is the decision by several state governments to try to be paisa wise and rupee foolish in trying to save a couple of hundred bucks in testing costs. Instead of browbeating and coercing private healthcare companies into taking up economically unfeasible tasks, civil servants ought to create positive incentives for more firms to enter the market, scale up operations and let competition keep the prices down. They must realise that it is in the public interest for private healthcare operators to be in good financial health.
Also read: RT-PCR, antigen, antibody, TrueNAT — all you need to know about the different Covid tests
De-regulate testing
With the ICMR liberalising the testing protocol to allow all doctors to order Covid-19 tests, we will see some improvement in test rates in the coming weeks. Similarly, the advent of cheaper rapid antigen tests can help authorities quickly scale up testing, as we have seen in Delhi over the past few days. State governments must avoid the temptation to impose fresh price caps on these tests.
Indeed, given the reality of the Indian healthcare system, domestic manufacturing capability and adequate market competition, the best policy is for the health ministry to completely deregulate Covid-19 testing, with the only condition being the mandatory reporting of results into the ICMR database. If anyone can walk into a laboratory, get a Covid-19 test done and get the result within a few hours, the problem of inadequate testing will rapidly melt away. This will free up the government’s resources for tracing, isolating and treating.
Disclosure: A member of the author’s immediate family is employed in a private genetic testing company.
The author is the director of the Takshashila Institution, an independent centre for research and education in public policy. Views are personal.






Contact tracing totally forgot and denying social transmission is incorrect. Tests figures are also misleading because every active /quarantine persons need minimum 6 tests to discharge after negative certificate. Of late normal death figures abnormal. Government should compare the so called normal death figures with last year’s figures to dispel people’s anxiety/doubts about increase in so called natural deaths.
good case by Pharma and health care hospital lobby forcing Govt to give them license to LOOT public and pile up cash mountain.. and well abetted by LOOTYENS, Lamborghini , Limousine vague Liberals socialists
@ Nitin,
You missed out on the point that market economics does not work for healthcare.!
I understand that to get pvt players into the game, the profit motive has to be there. But Pvt healthcare in India is predatory. If caps are removed, all of them will form a cartel and start charging exorbitant rates. At that point, the testing will out of reach for majority of the population especially those who cannot afford to work from home.
Caps have to be in place ..!!..The best a govt can do is to adjust the testing price to include minimum profit for pvt players.
Also, if govt can take over pvt hospitals for Covid19 patients why can’t they take over pvt hospitals and directly pay them including operational costs and such??
This is stupidity itself , one month before rt pcr tests were imported and now test kits are produced in india and the avareage market price is 1200 rupees if the cost of kit os 1200 how can test cost be 4500 ?
Is the cost of administring a test is 3300 ? Also there is a racket going on with biocon itolizumab when the drug is a not a new one in market and there is not R & D cost involved
Oh yes lets deregulate the prices let hospitals and labs go on money sucking rampage. Then this same idiot author will write government has turned blind eye and medical industry is extorting money from public. Write article if you have proper solution. Second when you compare countries check their population too.
The cost of RNA extraction from Swabs have dropped to Rs150/samples (rates quoted to laboratories). The most commonly used imported test kits costs 700/test. Most companies involved in testing already had the infrastructure , some have augmented it. The some kit selling distributors have already reached 7-10 times their annual turnover in 3 months. Their employees are getting increments while others are losing life and their jobs.
What does the author want, does he want a situation like corporate private hospitals who charged 8-9000 per PPE kit when it was available for 650-950 per kit.
In this country every one is an expert except the persons working in the field concerned
I am completely shocked by the very fact that these kits are not being provided to atleast the developing or third-world countries for free. Well, do you want the coronavirus disease to be checked and traced and stopped from spreading? or do you want to make a f****** business out of this too?!
If they really wanted to stop it from spreading, things would never have reached the level they have reached now. And even then, everyone is hell-bent on making a business out of it. An ignominious shoutout to USA and China.
Considering the huge size of Indian population, the 1st info graphic is misleading on its own and reflects a bias. The author should also add total number of tests when he is comparing with other countries.
India always this idea of price caps (Re 1 rice ?) then rationing everything. The poverty in the country we have seen how this policy its works.
Look at this board. People still defending price caps and govt intervention
no cap is as worst as stringent cap…. best option is formulate a reasonable price by counting kit cost, overhead costs and cost adjusted profit…for this the diagnostic centers should be categorized to provide appropriate incentives
Not price of test but the regulation of who can be tested has stymied the numbers