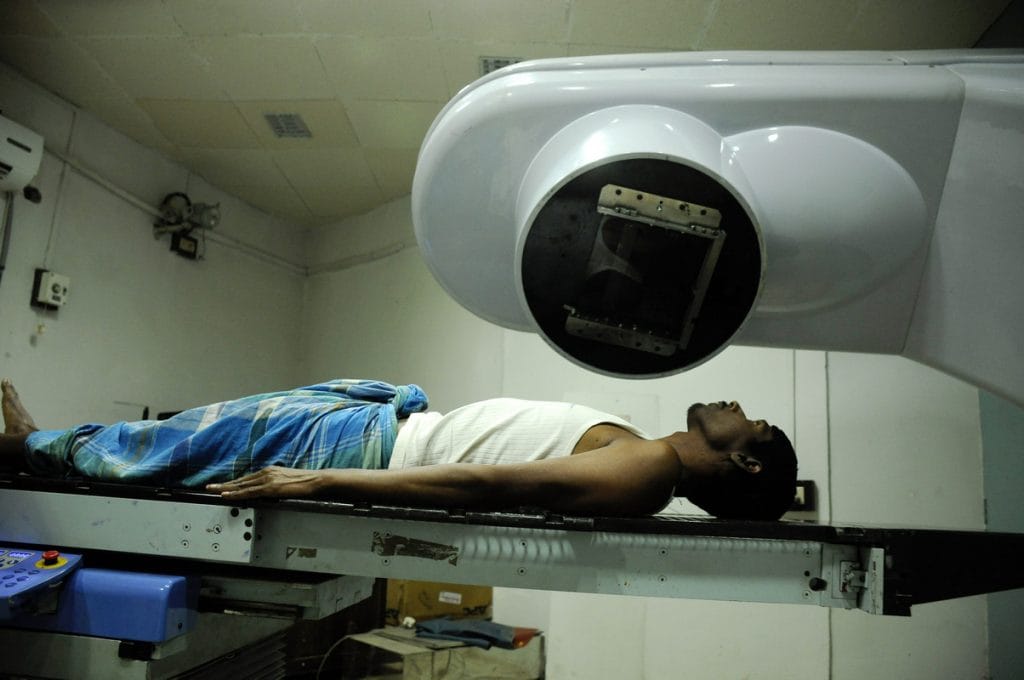
Studies suggest that air pollution, both indoor and outdoor, is linked to rising lung cancer cases among non-smokers, particularly the young & women.
New Delhi: Lung cancer cases are on the rise across India, and shockingly, it is the type least linked with smoking whose numbers are increasing faster.
This suggests a link with air pollution, both indoor and outdoor, experts say.
“The number of non-smokers with lung cancer is going up by 30 to 40 per cent. There could be other factors like obesity or drinking, but what is glaring is air pollution,” says Dr Shyam Aggarwal, chairperson of the Department of Medical Oncology at Sir Ganga Ram Hospital, Delhi.
Data and studies from the major cancer treatment centres across the country as well as case specific evidence from specialists suggest a clear link, although there is no nationwide data yet to confirm this increased incidence.
In Delhi, for instance, the number of lung cancer cases reported at the All India Institute of Medical Sciences (AIIMS) has more than doubled from 940 in 2013-14 to 2,082 in 2015-16, coinciding with a time of increased air pollution in the city.
Dr Randeep Guleria, one of India’s top pulmonologists and director of AIIMS, says there is plenty of data indicating a link between lung cancer and indoor pollution, especially coal and biomass burning, and that similar links could be drawn with the possible impact of outdoor air pollution, although more robust data would help establish the link more clearly.
Changing face of lung cancer
Specialists say increasing numbers of non-smokers, often young, are being diagnosed with lung cancer.
The nature of lung cancer cases being reported is changing too. For instance, more cases of adenocarcinoma, linked with a mutation in genes caused by a range of environmental and other factors, are being reported.
Historically, the types of lung cancer found among smokers differ from those among non-smokers. ‘Small cell lung cancers’ almost always occur in smokers, while ‘non-small cell lung cancers’ occur among smokers and non-smokers alike, and adenocarcinoma is among the latter type.
More adenocarcinoma cases are being reported elsewhere in the world too, but not at the same speed as in India. This has alerted researchers, who are studying this new trend in cancer hospitals across India.
One critical question they are asking is: is the polluted air Indians breathe in many parts of the country leading to increased lung cancer cases, especially among the young and non-smokers?
Is pollution to blame?
The association between air pollution and lung cancer has been well established for decades.
The International Agency for Research on Cancer (IARC), the specialised cancer agency of the World Health Organization, classified outdoor air pollution as carcinogenic to humans in 2013, citing an increased risk of lung cancer from greater exposure to particulate matter and air pollution.

Since fewer people smoke nowadays thanks to the worldwide anti-smoking sentiment, the increase in the number of lung cancer cases has to have another reason, says Dr M.S. Kanwar, senior consultant for respiratory medicine and pulmonology at Indraprastha Apollo Hospital in Delhi. He adds that air pollution is also implicated in oral and throat cancers.
Confirming a rise in reported cases of lung cancer among non-smokers, Aggarwal explains: “Adenocarcinoma is related to certain mutation in genes linked to air quality and pollutants. The incidences of adenocarcinoma are clearly on the rise. Younger patients between 30-40 years, more females and non-smokers are coming to us with advanced cancers.”
Among non-smokers with lung cancer, external environmental factors cannot be ruled out, says Dr Sameer Kaul, surgical oncologist at Indraprastha Apollo Hospital in Delhi. “It is hydrocarbons and carcinogens which have played havoc in human lungs,” he says, adding that genetics and external triggers “cooperate” to cause disease.
Dr S.K. Chhabra, head of the Department of Pulmonary and Critical Care Medicine at Delhi’s Primus Super Speciality Hospital, has been tracking the changing nature of lung cancer since 1998. “We found those living in more polluted areas had a 5 per cent decrease in lung capacity. They were non-smokers, and there was no other factor that could be established other than pollution,” he said.
Outdoor and indoor air pollution contribute equally to lung cancers as both have the same carcinogen content, says Dr Rajinder Prasad, founder and vice-president of the South Asia Association of Allergy, Asthma and Applied Immunology and the Indian Society for Study of Lung Cancer.
Not just a Delhi phenomenon
Although most experts ThePrint spoke to are based in Delhi, India’s most polluted metropolis, the story extends far beyond.
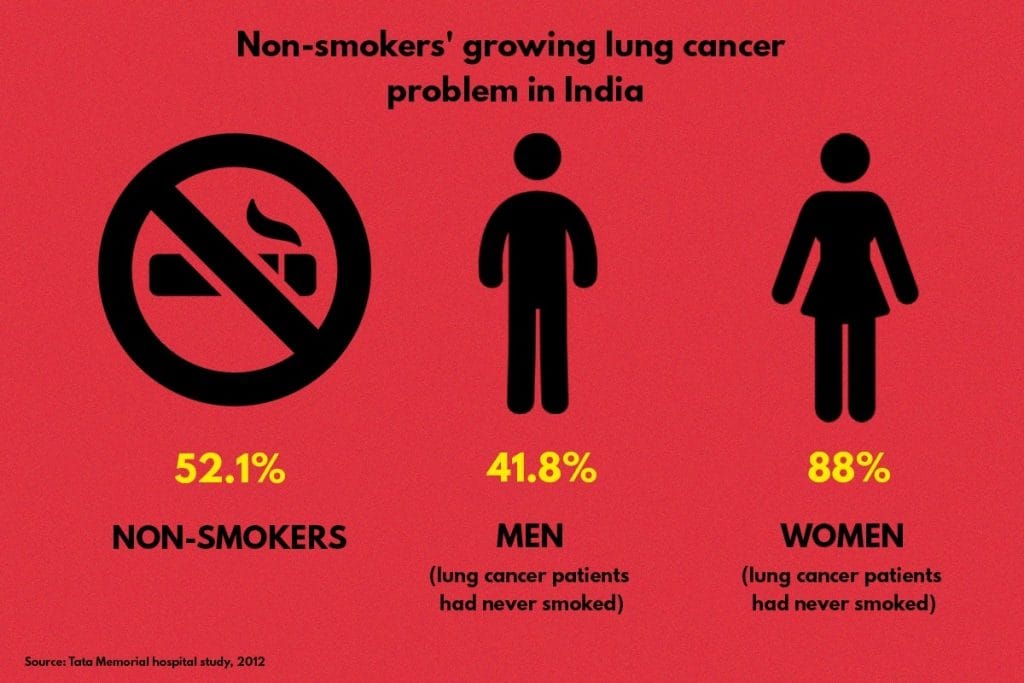
A 2012 study by Mumbai’s Tata Memorial Hospital found that 52.1 per cent of lung cancer patients had no history of smoking. The study contrasted this with a Singapore study that put the number of non-smoking lung cancer patients at 32.5 per cent, and another in the US that found the number to be about 10 per cent.
The Tata Memorial study found that 88 per cent of female lung cancer patients were non-smokers, compared with 41.8 per cent of males. It concluded that in the case of non-smokers, environmental and genetic factors were implicated.
In January 2017, researchers at AIIMS, Bhubaneswar, published a demographic profile of lung cancer in eastern India, which found that 48 per cent of patients had not been exposed to active or passive smoking; 89 per cent of women patients had never smoked, while the figure for men was 28 per cent.
A ‘clinico-pathological profile of lung cancer among smokers versus non-smokers’ published in January 2017 by the United CIIGMA Hospital in Aurangabad noted that between 10 to 25 per cent of lung cancer patients had never smoked, and that their number was rising.
And this is not an exclusively urban phenomenon.
Tata Memorial’s 2012 study found that among patients from rural India, indoor air pollutants such as cooking oil fumes and coal-stove smoke could be contributing factors. These are, in fact, suspected to be key factors behind more non-smoking women being diagnosed.
The study also found that 42.55 per cent of lung cancer cases in rural India were among non-smokers, and that the maximum number of patients were diagnosed at stage 4, the last.
Limited understanding
From available research, very little is understood about lung cancer among non-smokers in India. “We need more robust data to identify how strong is the risk and link,” Guleria of AIIMS says.
A 2016 study by Tata Memorial on ‘Lung cancer in the Indian subcontinent’ had observed that the “alarming rise” in non-smoking lung cancer was yet to be completely understood. It had blamed the “limited understanding of the impact of factors such as the presence of indoor air pollution, the use of domestic or biomass fuel exposure, the presence or lack of micronutrients in our diet, occupational exposure, and the possible contribution of infectious pathogens.”
The Aurangabad study had highlighted another challenge – most patients had reported at the advanced stages 3 or 4, when treatment is difficult and death nearly certain.
In addition to wider and more in-depth research, experts are unanimous that India needs greater awareness to encourage patients to visit a doctor when early symptoms show up — persistent cough, coughing with blood in sputum, chest pain that gets worse with deep breathing or coughing, hoarseness, weight/appetite loss and shortness of breath, among others.
Early detection is all the more crucial as lung cancer at stage 1A has a five-year survival rate of 49 per cent as against 5 per cent at stage 3B, according to the American Cancer Society.







Nice blog, as you have mentioned that lung cancer can occur in nonsmokers due to pollution, smoke, and fumes while cooking. Sometimes it is not easy to diagnose lung cancer because the symptoms are normal like cough, fatigue, etc. But if you find any of the symptoms on a regular basis then it is very necessary to check if you are diagnosed or not. Positive Bioscience is a cancer testing company in Mumbai where You can get cancer testing and free consultation from experts. They offer the best treatment plans for your cancer. I will definitely suggest to visit Positive Bioscience if you want to diagnose cancer at an early stage and want to get the best treatment plans.