New Delhi: With over 19.9 crore Indians living with high blood pressure and high salt intake causing 1,75,000 deaths every year, the country’s leading heart doctors, kidney specialists, and public health experts have recommended replacing regular table salt with a potassium-enriched alternative. This switch, they say, can cut the risk of stroke by 14 percent and deaths from heart disease by 12 percent. This, they say, will be comparable to any first-line pharmacological interventions (treatment using drugs).
The recommendations follow the January 2025 launch of the World Health Organization (WHO) guidelines on the use of lower-sodium salt substitutes.
A panel of 29 Indian medical experts has now signed a consensus statement, recommending that low-sodium salt substitutes (LSSS) need to be integrated into national sodium-reduction strategies, hypertension and other NCD (Non-Communicable Diseases) guidelines, and regulatory frameworks.
This includes recognition of potassium-enriched iodised low-sodium salt as an approved “edible salt” category by the food regulator, the Food Safety and Standards Authority of India (FSSAI), and clear evidence-based labelling.
LSSS are reformulated versions of regular salt in which 15 to 30 percent of sodium chloride is replaced with potassium chloride. The result is a product that looks, tastes, and cooks much like conventional salt, but delivers less sodium and more potassium—a mineral known to help lower blood pressure.
At a national consensus conference on LSSS as a public health intervention Friday, hosted by George Institute for Global Health—an independent, non-profit medical research organization—in collaboration with global health nonprofit Resolve to Save Lives, researchers presented relevant findings from a white paper.
The white paper presents scientific evidence and expert recommendations for replacing regular table salt with low-sodium, potassium-enriched salt substitutes as a cost-effective strategy to reduce hypertension, stroke, and cardiovascular deaths in India.
Dr Ambuj Roy, Professor of Cardiology at the All India Institute of Medical Sciences (AIIMS), New Delhi, and a member of the expert panel, said, “Despite LSSS receiving the highest possible recommendation in this year’s guidelines from the American College of Cardiology and the American Heart Association, the switch remains almost entirely absent from clinical practice in India.”
Also Read: Swap table salt with low sodium substitutes, says WHO. Why Indian doctors say this can save lives
Uniquely Indian opportunity
According to the white paper, the average Indian consumes between 8 and 11 grams of salt a day—roughly twice the WHO’s recommended limit of 5 grams.
But what sets India apart from other countries dealing with the same problem is where that salt comes from. In wealthier nations, most sodium enters the diet through processed and packaged food. In India, roughly 80 percent of sodium intake comes from discretionary salt—the salt that people add themselves while cooking at home or eating at the table.
As the white paper notes, this means that “LSSS must primarily target household consumption. Population-level substitution in homes, community kitchens, and mid-day meal programmes offers the highest potential impact”.
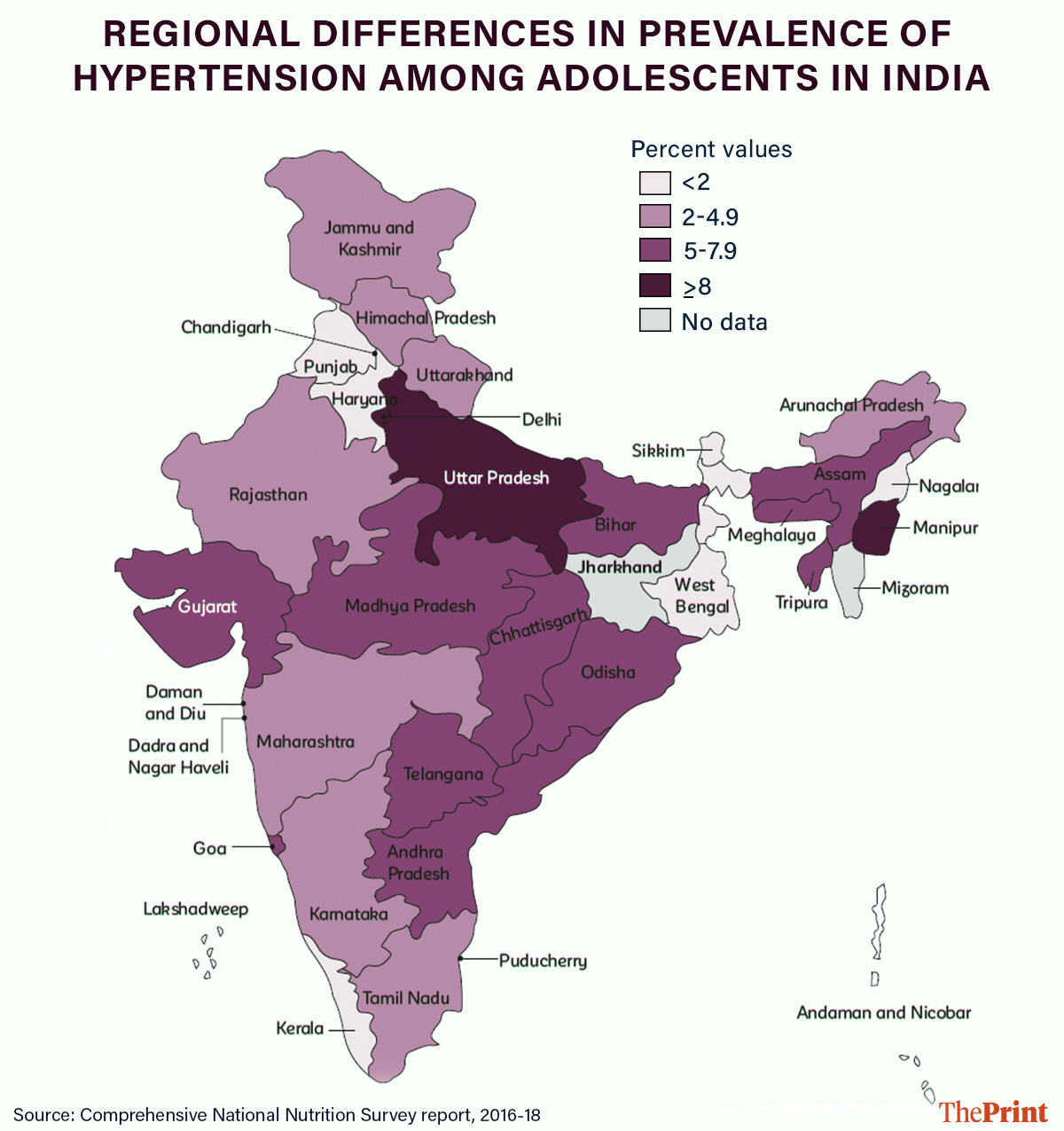
India’s low potassium intake makes the case even stronger.
Studies reviewed in the white paper found that Indians consume on average around 1,826 milligrams of potassium per day, which is well below the WHO’s recommended 3,500 milligrams.
The paper noted that an LSSS containing 30 percent potassium chloride, used at the recommended intake of 5 grams of salt per day, would add roughly 779 milligrams of potassium daily. This is within safe limits and can improve the amount of potassium Indians get.
Research by the George Institute suggests that 75 percent of the blood pressure-lowering benefit seen in large clinical trials came from the increase in potassium and not just from eating less sodium.
What the existing trials show
The largest study on this subject, the Salt Substitute and Stroke Study (SSaSS), conducted across 600 villages in rural China between 2014 and 2020 with nearly 21,000 participants, found that switching to potassium-enriched salt reduced the risk of stroke by 14 percent, major heart-related events by 13 percent, and deaths from all causes by 12 percent over nearly five years.
Importantly, there was no significant increase in serious side effects related to high potassium levels.
An Indian clinical trial, the Salt Substitute in India Study (SSiIS), conducted in villages in Telangana between November 2019 and January 2020 by researchers from George Institute for Global Health in India, and other researchers from Australia, and the United States, found that replacing regular salt with a blend of 70 percent sodium chloride and 30 percent potassium chloride reduced blood pressure in adults with hypertension.
Stratified use for people with kidney disease
The recommendation made in the white paper is not for everyone. The main concern is hyperkalaemia—a condition where potassium levels in the blood become dangerously high—in people whose kidneys cannot remove excess potassium efficiently.
The risk of high potassium mainly affects people with severe kidney disease or those taking medicines that increase potassium levels.
Experts recommend a case-by-case approach. Most people—including those with mild kidney issues, diabetes, or on common blood pressure medicines—can safely use low-sodium salt, as long as they’re monitored properly.
Professor Vivekanand Jha, Executive Director of the George Institute for Global Health, India, noted that the benefits of LSSS come from both eating less sodium and getting more potassium, with potassium providing the larger share of benefit. “Recent kidney disease guidelines themselves acknowledge that evidence for strict long-term potassium restriction in early kidney disease is weak, and that higher potassium intake may actually protect kidney function in the early stages of CKD (Chronic Kidney Disease),” he said.
Professor Sandeep Mahajan, nephrologist at AIIMS New Delhi, argued that the risk is being overstated and that a simple list of warning conditions would open the door for the vast majority of people. “That would free approximately 90 percent of the population, which can use it,” he said. “We are just looking at a small proportion—not even 10 percent.”
Mahajan drew a comparison with tobacco warning labels to argue for targeted cautions rather than a sweeping restriction.
The barriers that remain
Low-sodium salt substitutes currently make up just 0.4 percent of India’s edible salt market. They cost two to four times more than ordinary iodised salt.
The paper pointed out that the higher cost is largely because of potassium chloride, the key ingredient, which is imported from Canada, Russia and Belarus, and accounts for 60 to 75 percent of production costs.
Availability is heavily skewed toward large cities like Delhi, Mumbai, Bengaluru and Pune, which together account for roughly 70 percent of all LSSS sold in India, with almost no presence in smaller towns or rural areas, the paper noted.
Experts said that awareness among doctors is low, with most general practitioners continuing to advise patients to eat less salt rather than switch to a different kind.
Chennai-based dietician Dr Meenakshi Sachdeva, who was also a part of the panel, noted that at current prices, switching costs roughly 25 paise more per day than regular salt, a gap she said is manageable.
Tamil Nadu had previously (in 2014) ran a government-subsidised low-sodium salt programme, she recalled, showing that scale and affordability are achievable with political will.
The white paper lays out a path forward. It recommends reducing the Goods and Services Tax (GST) on LSSS, providing production subsidies, incorporating the substitute into national dietary guidelines with clearly defined warning conditions, training healthcare professionals, and running public awareness campaigns with simple messaging.
It also recommends including LSSS in government food procurement for school mid-day meals, the Integrated Child Development Services (ICDS), the public distribution system, and hospital kitchens, to bring costs down and normalise its use among the people most affected by high blood pressure.
(Edited by Ajeet Tiwari)
Also Read: Hypertension care guidelines miss out on endorsing low-sodium & potassium-enriched salt, says study





