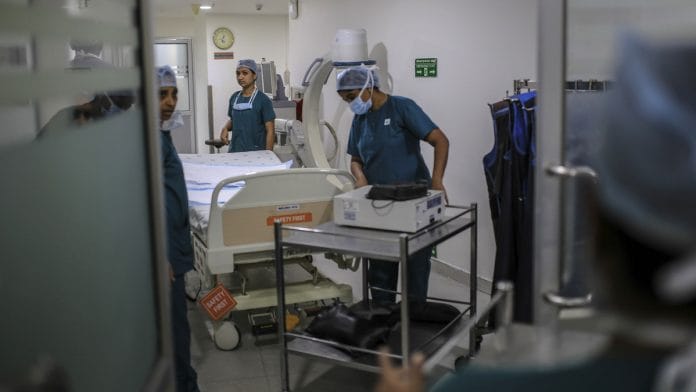
With a second wave of COVID-19 hitting Beijing, it is abundantly clear that the era of lockdowns is not over.
Beijing is once again shutting hospital doors, preventing expectant mothers, cancer patients and people living with a rare disease or requiring routine surgeries from seeking care. There is also debate on how to record the number of deaths caused by COVID-19: not just the people who die from the virus itself, but all of the peripheral or missed victims.
By prioritizing the prevention of the spread of COVID-19, we have globally – and unintentionally – left behind those who already live on the brink of life and death every day: people with chronic health conditions. For people living with cancer or a rare disease, hospitals shutting their doors to anything but COVID-19 is a problem – and it cannot happen again in a second lockdown.
Right now, we must address a growing third wave: the expedited loss of people struggling with non-COVID disease. We must take immediate action to prevent continued scenarios in which the potential health risk of closing off care for a non-COVID disease is greater than the risk associated with potentially contracting COVID-19.
Doctors are being forced to sit on the sidelines.
Doctors who don’t work in the emergency room, intensive care unit or parts of a hospital responsible for infectious disease are hindered, if not entirely unable to continue with their work, with the current standard for shutdown. The Royal College of General Practicioners in the UK found that in Northern Ireland, 4 out of 10 general practice doctors have been unable to practice since the shutdowns began.
According to the American College of Emergency Physicians, 70% of people are very or somewhat concerned about going to a health facility for fear of contracting COVID-19. This perceived risk, however, means we are also seeing far lower numbers of routine disease management and preventive screenings. Emergency rooms have seen a 50% decline in visits, meaning a significant number of people are waiting too long to seek treatment, which can lead to long-term damage and premature death.
Acute, deadly conditions like heart attacks, strokes and appendicitis are also at all-time low levels of hospitalizations, even though the occurrence of these conditions in the general population is not likely to be decreasing. Cigna, a major US healthcare payer, found hospitalization decreased 35% for atrial fibrillation, 31% for transient ischemic attack, 28% for epilepsy and seizures and 24% for gastrointestinal bleeds compared to normal levels before the initial COVID-19 lockdown in the US.
While telemedicine is bringing some relief, many common deadly conditions cannot be adequately managed by a video chat or phone call with a clinician.
Also read: Lockdown saw fall in cancer care, child delivery claims under Ayushman Bharat: Govt report
New cancer cases aren’t being detected.
Each year, 18 million people are diagnosed with new cases of cancer. Globally, cancer is the second-leading cause of death, responsible for an estimated 9.6 million deaths – one in six – in 2018.
And early detection is critical. With cervical cancer, for example, the five-year survival rate is 93% when diagnosed before the cancer spreads, but 15% when the cancer is at an advanced stage. Early detection also reduces the cost of cancer treatment, with costs for people who are diagnosed early costing two to four times less money to treat in our hospital systems than those diagnosed at a later stage.
During the pandemic, there have been significant decreases in cancer screenings. During the first 15 weeks of 2020 compared to the first 15 weeks of 2019, cervical cancer tests decreased by 68.2%, ovarian cancer tests by 33.8% and breast cancer monitoring by 17.4%.
It comes as no surprise, then, that a data analytics firm noticed a 31% decrease in the number of newly diagnosed cancer patients in March in the US. Specifically, the number of newly diagnosed breast cancer patients dropped by 8.4%, the number of newly diagnosed ovarian cancer patients by 8.6% and the number of newly diagnosed colorectal cancer patients by 14%.
People living with rare diseases are being ignored.
Perhaps the group hit hardest by the near-total shutdown of hospital systems is the 475 million people globally living with a rare disease, who wait an average of 5-7 years to be diagnosed and then only have a 5% chance of an US FDA-approved treatment being available. In normal times, many people living with a rare disease see their care team in a clinical setting weekly, if not more frequently.
In Europe, 9 in 10 people living with a rare disease experienced interruption in care for their disease, with 6 in 10 categorizing this interruption as “detrimental” to their health. Furthermore, 3 in 10 perceived the interruption as “definitely” or “probably” life-threatening. More than half who needed immediate surgery or transplants had such interventions either indefinitely cancelled or postponed. Lastly, 7 in 10 people with a rare disease continue to have appointments with primary care doctors or specialists cancelled – affecting around 25 million of the estimated 35 million people in Europe living with a rare disease.
Similarly, of the estimated 25 million people impacted by a rare disease in the US, 95% reported that COVID-19 affected their immediate and long-term health and well-being. In addition, 74% had medical appointments cancelled, while 69% worried about medication and medical supply shortages.
Meanwhile, the small number of people living with a rare disease who were able to have their care designated as “essential” to receive in a clinical setting were treated as if they were infected with COVID-19 by default. In order to attend clinical appointments, many people with rare disease are being unnecessarily put at risk for contracting COVID-19. The vast majority of hospitals in the US require everyone, with or without COVID-19, to enter through the emergency room and be screened for the virus before proceeding to appointments in other wings. Why can’t people with a rare disease have their own entrance, away from potential exposure to COVID-19? Why are we putting our must vulnerable populations at an increased risk for contracting COVID-19 amid the pre-existing circumstance of a risky delay in clinical care?
While some jurisdictions specifically planned for providing care to people living with rare diseases during COVID’s first wave, in the majority of regions around the world, there has been a void in policy, resources and action around rare diseases. Driven by need, the rare disease community has stepped up to attempt to fill that void. Yet, with an estimated 475 million people globally living with a rare disease, the lack of a dedicated, coordinated, visible and accessible approach is akin to neglecting the care of the world’s third-most populous country during a time of crisis.
Healthcare is essential—all of it, for everyone.
While many hospitals have tried to make case-by-case decisions on what procedures should be allowed, a perspective focused only on minimizing foot traffic is missing a crucial consideration: all healthcare is essential.
It is time to face the growing “third COVID wave”: preventable losses from non-COVID diseases caused by the lockdowns. Policymakers and administrators are in an untenable position, trying to determine if suffering long-term painful, adverse consequences of living with a rare disease or dying of cancer is less “essential” than suffering from COVID-19 or dying from complications of it.
There is an enormous opportunity to translate the successes, and learn from the failures, in managing the first wave of the COVID-19 pandemic. To start, healthcare administrators must consider separating COVID-19 services from the equally necessary services like screening for cancer or rare-disease complications. We could have special hours for non-COVID-19 patients, similar to grocery stores accommodating seniors, or offer drive-through appointments to allow face-to-face evaluation or routine vaccine delivery.
The dynamics of both living with any disease and a pandemic are characterized by isolation, uncertainty and shared needs – needs like connection; innovation; accelerated drug repurposing, clinical trials and novel vaccines; dedicated and agile regulatory frameworks; coordinated multi-stakeholder interaction; acute and ongoing intervention; clear and consistent communication and use of language; and a global public health response.
We cannot deem only the COVID-19 response as “essential” and treatment for people living with other diseases as “non-essential”. Creative solutions are desperately needed to ensure the global population can access basic healthcare, crisis or not.
Lynsey Chediak is Lead, Precision Medicine, Shaping the Future of Health and Healthcare, World Economic Forum
Gareth Baynam is Founder, Project Y, Program Director, Undiagnosed Diseases Program Western Australia, and Head, Western Australia Register of Developmental Anomalies
This article was originally published in The World Economic Forum
Also read: How Covid is making it tougher to tackle TB, AIDS, malaria and child health