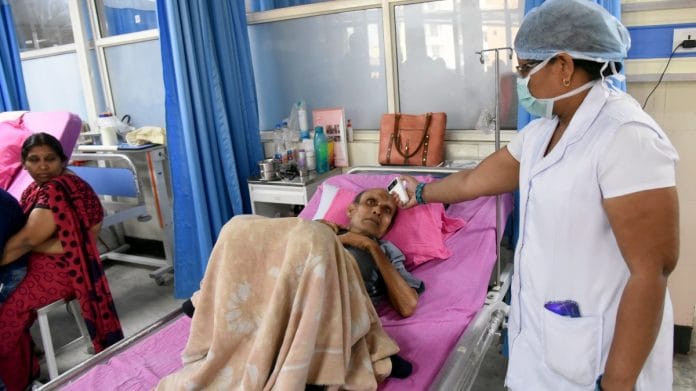
Patna: As Covid-19 cases continue to surge in Bihar, the state government Tuesday announced a complete lockdown until 31 July.
The lockdown is, however, only for urban areas of Bihar, and the villages have been exempted from it.
All schools, colleges, malls, religious places and public transport will remain shut. Shops selling essential items like food and medicines can remain open. Government offices will also remain open with 50 per cent staff capacity.
Deputy Chief Minister Sushil Kumar Modi said that a meeting would be held late Tuesday evening to introduce other measures to curb the spread of Covid-19.
Talking to ThePrint, Modi said the detailed guidelines of the lockdown would be announced later.
Doctors, however, said half-hearted lockdowns without people wearing masks or maintaining social distancing won’t yield any results.
“I find more than half the people without masks and moving in groups, while the police look the other way instead of penalising them. It’s becoming scary,” said Dr Kumar Vikram, who runs a private clinic in Patna.
But the Additional Director General of Police, law and order, Jitendra Kumar Monday issued a statement, saying between 5-13 July, police have fined over 28,000 people for not wearing masks.
As of Tuesday evening, Bihar has 18,853 total cases and 143 deaths, according to state government data. In the last 24 hours, 1,432 fresh cases were reported.
Also read: Ventilator-equipped hospital to be set up at Bihar CM Nitish Kumar’s residence
Crisis in state-run health hubs
In the wake of the rising Covid cases, the state government Sunday took a desperate step and announced free treatment for coronavirus patients in all state and private institutions.
But the trouble is not many appear to have faith in the government’s health facilities. When the director of one of Bihar’s premier health hubs, Indira Gandhi Institute of Medical Sciences (IGIMS), Dr N.R. Biswas tested Covid-positive, he didn’t get himself admitted in his own institute. He was admitted in the central-government run AIIMS in Patna. The IGIMS is run by the state dispensation.
“There appears to be a failure on the part of the government in planning. A Covid hospital needs three things — a dedicated ICU unit, ventilators and oxygen. The government dedicated NMCH (Nalanda Medical College and Hospital) as a Covid hub and has over 800 beds. But it is not only beds that matter. How many patients can they adjust in the ICU? The government’s order is fine for patients with mild symptoms. But serious patients need much more than beds,” said Dr Prabhat Kumar, a former scientist of ICMR.
On 7 July, the state health department declared just 385 fresh cases. On 8 July, it was 749. On 13 July, the numbers shot up to 1,266. Doctors say these rising numbers could suggest a community spread of the disease.
“I believe community spread has started. In a place like Bihta, located on the outskirts of Patna, there have been 126 cases in one go (June-end),” said Dr Ranjan Kumar, a private practitioner in Patna’s Kankarbagh locality.
The doctor was referring to a wedding, which emerged as super-spreader of Covid-19.
‘Overburdened AIIMS’
Two days ago, a video went viral on social media, showing an official of the state home department suffering from Covid-like symptoms and lying at the gates of AIIMS as the guards refused him entry. The official later tested positive and was admitted to AIIMS.
On this, AIIMS authorities expressed anger at the IGIMS, which referred the patient to the former. “He was referred to us by IGIMS. The least they could have done is to treat him during the night and send him in the morning,” said an AIIMS official, claiming that the hospital was being overburdened because institutes like IGIMS and Patna Medical College and Hospital have stopped taking Covid patients.
Director of AIIMS, Patna, Dr P.K. Singh told ThePrint: “A week ago, we had around 200 Covid patients. Today, we have more than 500. They keep pouring in. We have a separate place for Covid patients where we keep less serious patients and the serious (ones) at another place. We strictly follow the standards.”
Also read: Across Bihar, migrants returning from Delhi top list of new Covid positive cases
Impact of returning migrant labourers
Dr Alok Ranjan, a public health expert of AIIMS with a PhD on community diseases from California University, said the impact of migrant labourers returning to Bihar from red zones like Delhi, Mumbai and Gujarat has been huge.
“Most of the patients admitted in AIIMS are migrant labourers or their kin. Most of them have travel history,” he told ThePrint, stressing that there is an urgent need to step up testing to get a real picture of Covid-19 in Bihar.
Asked if Bihar is seeing community transmission, he said: “I do not have sufficient data to indicate that there is community spread. But the situation is alarming.”
The government, however, has been silent on the number of beds available in ICUs and ventilators in state-run health facilities.
But Monday, health department secretary Lokesh Kumar Singh said in a statement that orders have been placed for oxygen cylinders and efforts are being made to increase manpower in all hospitals.
State Health Minister Mangal Pandey said that 40,000 units of rapid testing kits have been sent to districts.
“But the government response has been too late and too little,” said a doctor, working at a government hospital, on condition of anonymity.
The government’s decision to include private health facilities in the Covid-19 fight is also facing reluctance.
“In government hospitals, disciplinary action can be taken for not treating Covid patients. In private hospitals, we cannot force staff to do so. They will quit. Also, how can I admit a Covid patient if I do not have extra ventilators or oxygen cylinders,” asked heart surgeon Dr Ajit Pradhan, who runs a private hospital in Patna.
Also read: 25 Bihar BJP leaders test Covid-positive, party says it has nothing to do with e-rallies