Bengaluru: Since the onset of the pandemic, researchers have been developing newer and more efficient methods to curb Covid infection. Today, the vaccines and boosters in circulation help prevent severe disease, saving millions from hospitalisation, and death.
However, Covid vaccines do not prevent infection or the disease itself. Now, researchers are looking at ways to prevent the SARS-CoV-2 virus from entering and infecting the body.
The main contender for such an effective defence against the virus is a nasal vaccine or spray, one that would elicit mucosal immunity. Such vaccines and sprays have been the subject of discussion since the early days of the pandemic, with research finally making headway into actually testing nasal sprays for mucosal immunity.
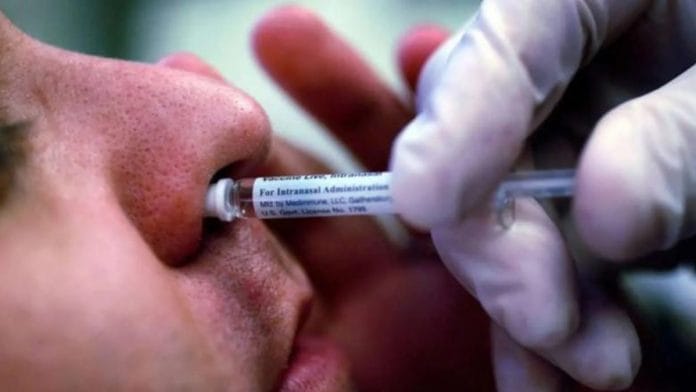
Mucosal vaccines are nasal or intranasal, and are not injection-based. They are often administered as sprays or drops.
Also read: Study on mice shows Covid virus leads to brain neuron death, higher anxiety, reduced cognition
Mucosal immunity
As the name suggests, the term ‘mucosal immunity’ is derived from mucosa — or the layer of protective mucus that lines our internal organs, as well as air passageways and the nose.
This mucus is made up of wet tissue, and is often the first line of defence against external particles and the outside environment, triggering an immediate and strong immune response. This occurs naturally, a typical example being allergic reactions including asthma.
As mucosal cells are so important to the body’s defences, they contain the majority of immune cells.
The mucosal immune system is the largest component of human immune systems. The body’s defensive cells — T cells and B cells (which produce antibodies) — reside in the mucosal lining in the respiratory, gastrointestinal, and urogenital tracts.
Our immune system produces multiple kinds of antibodies, of which IgA is produced as an immediate and generic defensive response, while IgG antibodies are produced after a few days from the first infection, with a more tailored and precise response that can destroy the pathogen in the body.
Traditional muscle-injected vaccines fine-tune the IgG response, but mucosal sprays and vaccines can improve the IgA antibodies so that the virus can be stopped and neutralised at its point of entry.
IgA antibodies are produced in a higher quantity than other antibody types combined, and could thus be utilised for better protection at a very early stage.
In the human immune response, IgA antibodies dominate the nasopharyngeal pathways where the SARS-CoV-2 virus enters the body, all the way up to the tip of the lungs, after which the IgG antibodies start to dominate.
Also read: Oxford study on long Covid says even mild infection spurs ‘brain shrinkage’
Current trials
Nasal vaccine development has been spurred on by the success of the oral polio vaccine (OPV), which induces mucosal immunity in the gut that helps eliminate the polio virus, spread through contaminated food and water.
In trials on mice and human cells, intranasal — or nasal — vaccines and boosters have shown tremendous promise. Researchers have discovered molecules that are capable of blocking infection in nasal cells, which are being tested on mice both therapeutically, after exposure to the virus, and prophylactically, before exposure.
There are many nasal vaccines that are currently in trial in many countries.
In India, Bharat Biotech is conducting trials of its intranasal vaccine at AIIMS Delhi.
There are also oral pills — being tested as an alternative to nasal vaccines — that act in a similar manner to trigger mucosal immunity. Mucosal vaccines use other vector viruses to carry the spike protein, similar to how the Covishield/Oxford-AstraZeneca vaccine works. Oxford, too, is currently testing the intranasal version of the same ChAdOx1 vaccine.
(Edited by Manoj Ramachandran)
Also read: Covid patients from 1st & 2nd waves can still feel buzzing in ears, doctors say it’s a concern