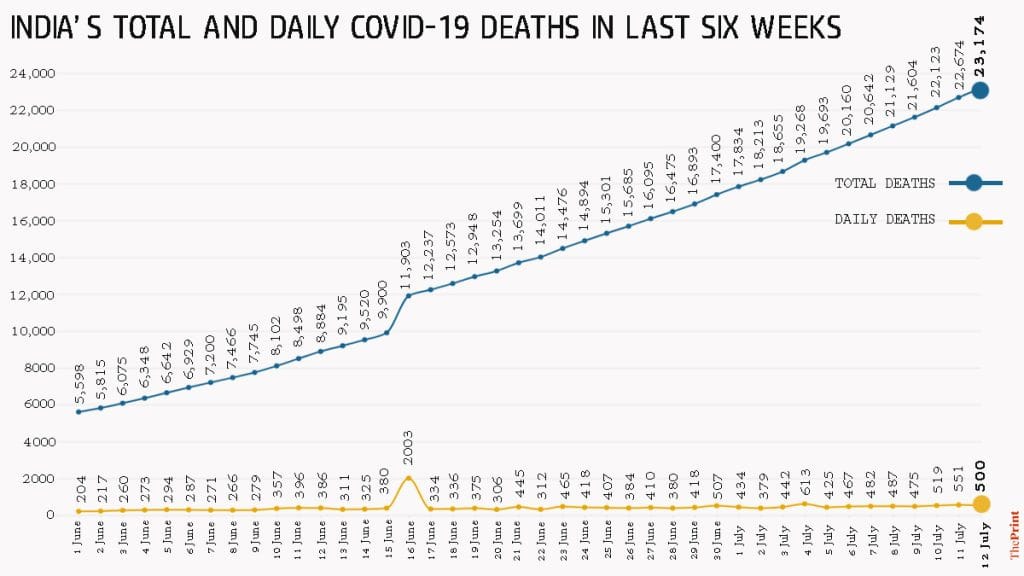
New Delhi: The Modi government has repeatedly said how well India has fared against the Covid-19 disease by citing figures such as cases/deaths per lakh population, but in the last six weeks, the number of daily deaths has more than doubled — to 500 on 12 July from 204 on 1 June.
Besides, the positivity rate — the number of cases reported among the total samples tested — has also risen steadily during the same period. In the 2-7 June week, it was 7.14 per cent, while in the 6-12 July week, the positivity rate was 9.8 per cent, according to government data.
The rise in daily death numbers has come with a more than tripling of daily cases, which kept India’s case fatality ratio among the lowest in the world, but experts say the age-wise break-up of deaths is the real cause for worry.
The fact that 47 per cent of all deaths in India are happening among people aged less than 60 years could be a very strong indicator that India is missing deaths in the elderly population.
The cumulative case fatality ratio in the country is currently 2.6 per cent, while globally it stands at 4.3 per cent.
Also read: Recovery rate crosses 60%, over 2.41 lakh tests, 379 deaths: India’s latest Covid numbers
Rising daily deaths
On 1 June, 204 patients had died of Covid-19. Since then, the number has been on the rise steadily, albeit by a small margin every day. An exception was seen on 16 June, when 2,003 deaths were reported after states like Delhi, Maharashtra and West Bengal — following a long political tussle — added deaths that had occurred earlier but were not attributed to coronavirus, in the total tally.
Preventing deaths has been a key goal of Covid-19 control measures as both government and health officials say that minimising delay for a patient, who needs medical care, is often the deciding factor between death and survival.
However, epidemiologist Dr J.P. Muliyil said it is not so much the number of deaths as the profile of the dead that is a cause for worry.
“A certain percentage of people infected with the virus will die. However, the experience of other countries is that 90 per cent of all deaths are among the elderly. Here that figure is just about 52 per cent, which gives me a strong reason to suspect that we are under-reporting deaths, especially in the elderly in urban slums,” he said.
“You think a poor, old person with pneumonia and breathlessness in an urban slum will seek medical help? You have made it so difficult for the person with quarantining and sealing of the house and all that. That seems to be the population we are missing. Even the argument about high malnutrition does not explain these deaths numbers because we do not have that kind of malnutrition any more.
“Morbid obesity is a comorbidity, but we do not have that as much as the US or many other western countries. Why then are young people here dying so much more? Because we are missing deaths in the elderly,” said Dr Muliyil, who is also a former principal of CMC Vellore.
The age-wise breakup of deaths in the analysis done by the Integrated Disease Surveillance Programme (IDSP) shows that 0.54 per cent deaths were among children aged less than 14 years, 2.64 per cent deaths were among 15-29 year olds, 10.82 per cent deaths were among people aged between 30-44 years, 32.79 per cent deaths happened among those aged between 45-59 years, 39.02 per cent deaths among those aged between 60-74 years and 12.88 per cent happened among people aged more than 75 years.
Also read: Fatigue and shortness of breath persist in recovered Covid patients, study finds
Disparities between states
Until 12 July, almost half of the total Covid deaths in the country — 23,174 — had happened in Maharashtra, according to data compiled by the Ministry of Health.
The state, which has been grappling with the disease from the very start, has so far seen the highest number of deaths — 10,289 — followed by Delhi (3,371) and Tamil Nadu (1,066). West Bengal and Uttar Pradesh follow with 934 and 932 deaths, respectively.
While Dr Mulyil is suspicious of the age profile of the dead, at the National Centre for Disease Control — the central agency for tracking infectious diseases — there are misgivings about the high percentage of deaths that are happening in people with no comorbidities. The IDSP analysis puts this figure at 43 per cent.
Health officials suspect it is because a lot of deaths among Covid-positive patients are being put down to comorbidities such as diabetes and heart disease. This too is resulting in under-reporting of deaths, they suspect.
“The data show that a high percentage of deaths are happening in people without comorbidities. However, this could also be because when there are comorbidities, many states are incorrectly putting the comorbidity as a cause of death rather than Covid, presumably to keep the numbers down. That would then also mean that we are missing out a lot of deaths in the national estimates. This is why we are pushing for states to report all deaths to us,” said a senior health ministry official.
Positivity on the rise
India’s daily sample positivity rate was 6-7 per cent in the first week of June. However with time, even though the number of tests has significantly gone up — 1,00,180 tests on 1 June versus 2,19,103 on 12 July (despite a usual weekend dip in tests) — the positivity rate also kept increasing.
In the 2-7 June week, the average positivity rate was 7.1 per cent, between 8-14 June, it was 7.6 per cent. Between 15-21 June, it was 8.68 per cent, between 22-28 June, it was 8.5 per cent. Between 29 June and 5 July, it was 9.5 per cent and between 6-12 July, it was 9.8 per cent.
Every Monday, the positivity rate shoots sharply because of low testing on Sundays. For example, Monday (13 July), the figure was 13 per cent, on 5 July, it was 13.4 per cent, on 28 June, it was 11.4 per cent.
There are wide discrepancies between states in terms of positivity rate. However, there is a general, informal consensus among various government agencies that a positivity of more than 10 per cent is an indicator that tests have not kept pace with the spread of the disease. India is dangerously close to that mark now.
Dr Giridhara R. Babu, head, life-course epidemiology, at the Indian Institute of Public Health, Bengaluru, said the ideal positivity rate advised both by WHO and the Government of India is 5 per cent.
“Both advise that positivity should not cross 5 per cent, but that is really ideal. Positivity rate is a function of the prevalence of the disease and the number of tests done. If any one of them goes up or down, it shows in the positivity numbers. For example in Telangana, the positivity figures shot up because they were doing too few tests and the prevalence of the disease was high. Delhi too had a similar situation,” he said.
Also read: India’s positivity rate jumps, 10 out of every 100 people tested is infected with Covid-19





