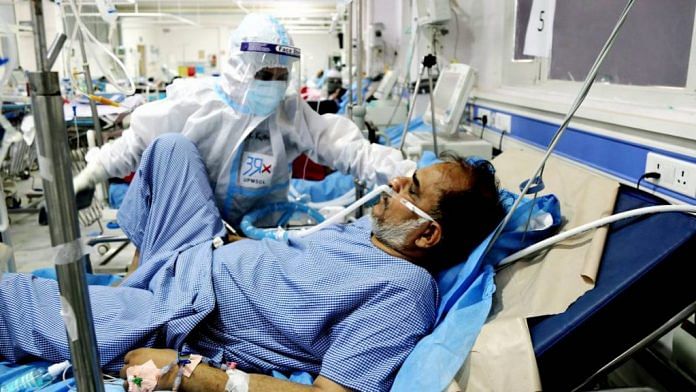
New Delhi: Excruciating pain, multiple surgeries, medical bills exceeding Rs 30 lakh and still a long way from recovery — for 33-year-old Gujarat-based interior designer Siddhartha Gohil, recovering from Covid-19 was not the end of sufferings. Owing to the use of steroids in treatment, weak body immunity resulted in mucormycosis, a life-threatening disease, known to spread “like a wildfire” in the body.
His doctor, Dr Tanu Singhal, consultant, infectious disease at Kokilaben Hospital, Mumbai, believes that Gohil is lucky to have survived the infection, as it didn’t infect his brain.
In latest proof of post-Covid complications, doctors have raised concerns over increasing cases of life-threatening fungal infections in patients, caused by prolonged use or high-dose intake of steroids that are being used to treat the infected. These include mucormycosis, a rare fungal infection that originates in the nasal sinus and spreads rapidly around the facial area, including the brain, and Aspergillosis, an infection in the lungs, less lethal than mucormycosis. There have also been cases of vision loss from glaucoma — permanent loss of eyesight owing to damage of the optic nerve.
All three problems are more common in those with diabetes.
While steroids — such as dexamethasone and methylprednisolone — are known to play a critical role in reducing deaths from Covid, its prolonged use, or high-dose intake, may lead to complications, warned experts.
Meanwhile, the central government, in a press briefing on Covid Friday, said that the occurrence of such fundal infections is natural and the correlation between mucormycosis and Covid-19 is not exclusive.
“It is a fungus that breeds on wet surfaces. It is very uncommon among patients who do not have diabetes. There are reports of this fungal infection among Covid-19 patients. But I want to reassure you that there is no major outbreak and we are monitoring the cases at our level,” Niti Aayog (health) member V. K. Paul, said.
Doctors insist, however, that the occurrence of the infections has gone up exponentially in recent months.
“In my decade-long stint at AIIMS, between 2002-2014, I would get just two-three cases of mucormycosis in a year. Today, I have been diagnosing two-three such cases every month,” said Dr Digvijay Singh, head, eye department, Narayana Hospital, Gurugram.
Singh added that “while steroids are essential medicines known to reduce deaths from Covid, we want to red-flag the trend of increasing cases of mucormycosis, glaucoma and cataract in patients who were administered steroids during their Covid treatment. The majority of these patients had a history of diabetes”.
Other medical experts too share similar concern.
Dr Shailesh Kothalkar, head and neck cancer surgeon, and director at Mumbai’s Seven Star Hospital, told ThePrint that “in the past two decades, I have operated on only 12 patients for mucormycosis. In the past two months, however, I have been doing three to four surgeries daily for mucormycosis. The surge is phenomenal.”
Experts highlight that those who have recovered from Covid-19 should keep a watch on symptoms of mucormycosis, such as stuffy nose, headache, black lesions on the upper inside of the mouth, facial pain, and loss of vision. For aspergillosis, common symptoms include breathlessness, cough, and fatigue. A feeling of pressure on the eyeballs and constant headache are primary symptoms of glaucoma.
Also read: Struggling to find an open Covid vaccination slot on CoWin? Get help from these websites, apps
Mucormycosis and its prevention
Talking about the life-threatening nature of mucormycosis, Singhal said, “generally, this infection spreads to the brain within a few days, and then it is impossible to save the patient.”
The Mumbai doctor said is now treating at least 15 patients every month with such fungal infections. “All the patients have a history of Covid and were given steroids during treatment. It’s a very strong trend. Symptoms of mucormycosis appear approximately two to four weeks after Covid treatment. And the death rate is very high, about 50 per cent,” she said.
Doctors advise quick tapering of high doses of steroids and prescribing steroids in accordance with treatment protocol, only when the patient is suffering from severe Covid.
“We have been seeing patients who start consuming steroids in early stages of infection on the prescription of local doctors, or they were given high doses of steroids over a long period. All this is leading to increased cases of steroid-induced side-effects,” said Dr Praveen Gupta, director and head, neurology at Gurugram-based Fortis Memorial Research Institute.
Also read: Your govt’s Covid failures have made another lockdown inevitable, Rahul Gandhi tells Modi
Aspergillosis and other complications
Doctors are also reporting a higher incidence of another fungal infection, aspergillosis. “There are more than 1,000 patients with aspergillosis currently across Gujarat and Maharashtra. Aspergillosis is not life-threatening as it doesn’t spread as rapidly as mucormycosis,” said Neha Gupta, consultant, internal medicine at Gurugram-based Medanta.
There are other complications induced by the increased use of steroids.
“If not fungal infections, use of steroids would lead to weight gain, calcium loss, reduced immunity, and acidity. It also leads to increased complications and mortality in people with diabetes,” Gupta said.
Singh, of Narayana Health, said that in the past one month he has come across two cases of glaucoma in patients who were being treated for Covid. “Patients generally feel high pressure in their eyes, specifically on the eyeballs. Steroid-induced glaucoma leads to damage to the optic nerve and causes irreversible blindness,” he explained.
(Edited by Poulomi Banerjee)
Also read: Delhi hospital study finds just 16% vaccinated individuals got Covid, experts say nothing serious