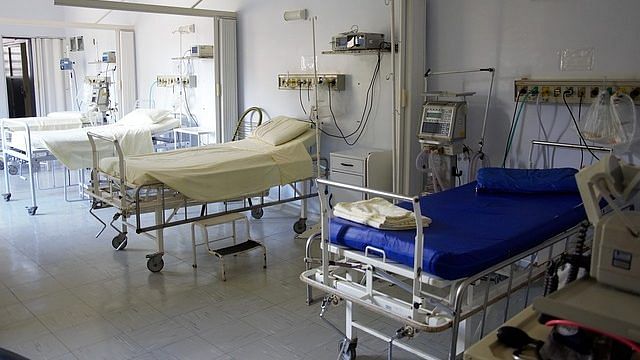
The concern with the health protection scheme is whether the insurance companies would make it worthwhile for hospitals to extend services easily.
Unfolding the budget, the finance minister devoted at least six paragraphs to support specific health initiatives.
Why is this important? Because until now, the Union Budget has been dominated by a vision founded on taxation, finance, industry, defence and the core sectors. Health has never received so much attention in terms of specificity. It indicates a new and welcome thrust on what matters hugely to people’s lives, and changes the age-old excuse that under the Constitution, health is a state subject.
But, there are ‘buts’. Because there are no details of how the schemes would pan out, one is left wondering whether and to what extent there would be a gap between intention and action. Providing insurance coverage through a national health protection scheme for poor families, and providing up to Rs 5 lakh per family per year for hospitalisation sounds fantastic. But the concern is whether the insurance companies would make it worthwhile for hospitals to extend services easily, efficiently, and with compassion. In case it is a cashless facility, the costing would be between the hospital managements and the insurance setup.
Judging from the implementation of the much smaller Central Government Health Scheme, the payouts by the government have been chronically slow and cumbersome, and many hospitals have opted out. It is precisely because of the track record of delayed payments that one is concerned. The management of the programme would have to devolve on the states, which do not function at the same level of professionalism.
Things will work if there is a specific law, which sets out duties, responsibilities and accountability overseen by a regulator who knows the workings of medical establishments. Setting up such a regulator and an ombudsman for overseeing the tug-of-war over payments has not been mentioned.
People do not just go to hospitals. Long before that happens, they need medication for day-to-day acute illnesses. They need laboratory services and diagnostic services within reach. The question of being hospitalised only comes up when someone has been diagnosed with the need for hospitalisation. At the back end, the poor go to thousands of unqualified medical practitioners (referred to as RMPs, which is a misnomer because they are not registered and have no medical qualification). These people give medication and also provide linkages with private-sector doctors running small clinics when things get worse. The question of going to a large hospital – covered by an insurance system – will arise when multi-speciality or super-speciality treatment is needed. But the bulk of health care is provided by non-doctors who have arrangements with private qualified doctors to take over cases which do not respond to their treatment.
Hospitals only account for eight per cent of the 10.4 lakh medical establishments in the country. Eighty per cent of medical services are provided by private sector single practitioners – qualified or unqualified. The intention here is not to take away from the thunder of a commendable announcement and the effort to universalise health care, but the back end process, which is the bane of health care in rural areas, and has not been confronted.
The 1.5 lakh wellness centres are expected to provide the diagnostic services and medication. If they are to replace or subsume the existing primary health centres and community health centres run by the state governments, it would not be practical. That is because the 25,000 primary health centres in the country and about 2,000 community health centres are not visited by the poor because of reasons which are important.
First, the opportunity cost of travelling 5-10 or more kilometres is too high, as it means the loss of wages and second, there is uncertainty about meeting a doctor or getting the medication – something the quacks give at an affordable cost within walking distance from the village. It is possible that the wellness centres would only cater to urban areas and, in that case, existing diagnostic centres and laboratories in the private sector could be accredited to provide services. But if the players are from the private sector, the question of monitoring, accountability and utilisation of public funds will come up and will need to be confronted.
The budget does not seem to have made specific financial provisions for accrediting privately-run clinics. Unless the assigned functions are clear and payment is regular, private centres would not find it making much business sense.
Providing nutrition at the rate of Rs 500 per month to tuberculosis patients is a welcome development. Tuberculosis treatment is long drawn-out and the poor are unlikely to spend on buying fruit, eggs and milk, which are costly. But if, as promised, there is cash support for the patient’s nutrition, the message would go that tuberculosis is not to be taken lightly. This would result in higher rates of people seeking diagnosis and course completion, which are fundamental to the success of the programme. Incentives have worked for maternal health, and will work for TB too. But money supply has to be sustained and given on time. That is the challenge.
The announcement that the government will set up 24 new medical colleges and hospitals by upgrading existing district hospitals in the country is excellent news. With one medical college in every three parliamentary constituencies, the health and medical sector will receive an infusion of a much needed health workforce. The presence of residents will automatically bring greater efficiency and improved output. But medical colleges are costly. If the state governments are expected to contribute, the scheme can get delayed. If it is a purely central scheme, then it has to be sustained including its recurring costs.
Given the laxity of many states and the dismal state of district hospitals, such a scheme may well take years to fructify. The question of assured funding has to be addressed and provided for. The size of the health budget does not give evidence of that. A clear understanding of the responsibilities of the Centre and the states is also needed. Without clear ownership for outcomes, the scheme may flounder.
I would not join those who say the health announcements are a jumla. But much thinking is needed on accountability, funding and sustainability. Unless there are detailed schemes to back the good intentions, the benefits may not reach the public as quickly as needed.
Shailaja Chandra is a retired civil servant and former secretary in the Health Ministry