- November is Lung Cancer Awareness Month.
- As people live longer the risk of cancer increases, with over 70% of cancer cases occurring in people over 50.
- By 2050, nearly two-thirds of the world’s population over 60 will live in lower- and middle-income countries.
- The option of healthy, cancer-free ageing should not be sequestered to high-income countries: it should be made available to everyone around the world.
Successful public health initiatives have contributed to a steady rise in lifespan around the world, but this positive trend is not without consequences. As people live longer, combined with environment and lifestyle changes, the risk of cancer increases, with over 70% of cancer cases occurring in people over 50.
The most common cause of cancer death worldwide is lung cancer, a burden that is most heavily felt in lower- and middle-income countries (LMICs) where early detection and treatment is limited. By understanding the gaps and barriers in identifying and treating lung cancer in LMICs, healthcare systems can invest in the necessary infrastructure to curb cancer trends as populations continue to age.
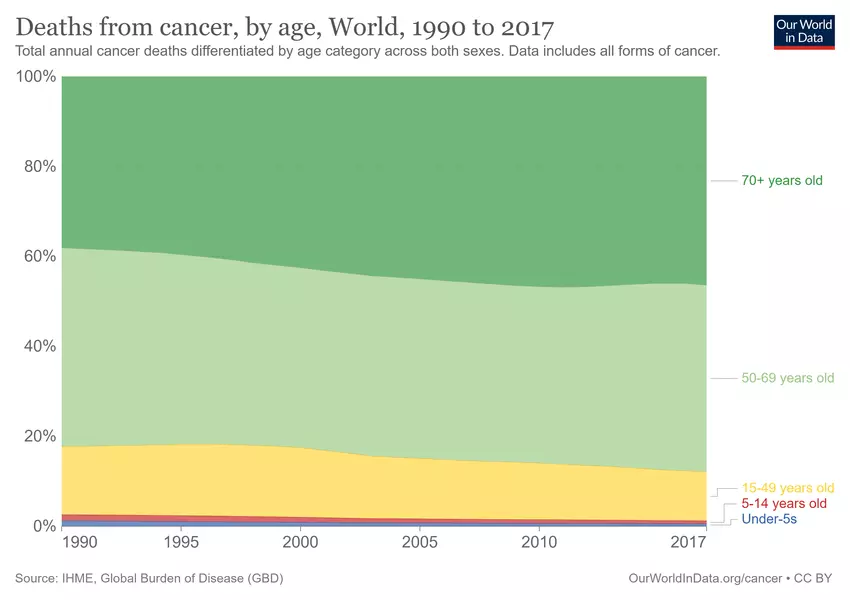
Lung cancer is an unequal burden
Worldwide, approximately 70% of cancer deaths occur in LMICs, a large fraction of which is attributed to lung cancer. Smoking is the leading risk factor for lung cancer and over 80% of smokers worldwide live in LMICs.
Environmental factors like poor air conditions created by traffic and residential heating also contribute to this disease. Smoking habits, industrialized cities, and growing populations, raise the need for widespread cancer screening across LMICs for early detection and treatment.
Early detection of cancer is one of the most effective ways to improve survival outcomes. Detection begins with screening to identify individuals with cancerous or pre-cancerous abnormalities. Next, diagnosis helps determine the most effective treatment regimen, which can save time and resources.
Infrastructure challenges like a lack of transportation, long travel distances, and poor road conditions can limit access to cancer screening in LMICs. The equipment and personnel necessary also means that available screening centres may be limited. Lung cancer symptoms that are similar to other diseases like tuberculosis, which infects the lungs, can lead to misdiagnoses and further delay treatment.
Even once a diagnosis is made, individuals in LMICs are not guaranteed adequate treatment. According to the World Health Organization, in low-income countries, fewer than 30% of patients diagnosed with cancer have access to treatment, versus 90% in high-income countries. This disparity is partly due to poor access to medications and inability to see the necessary surgical and cancer specialists.
The COVID-19 pandemic has further exacerbated the lung cancer burden in LMICs. Healthcare resources have shifted towards fighting the pandemic, while the implementation of pandemic mitigation steps like physical distancing has impaired hospital services by postponing cancer screening, in-person consultation, and limiting treatments.
As countries reimagine their healthcare systems post-pandemic, specific attention must be given to cancer as populations age and as lifestyle changes lead to higher incidences of noncommunicable diseases.
Also read: Detection is key for breast cancer patients. AI can make it more accessible and affordable
Improving lung cancer survival in LMICs
The first step towards reducing lung cancer mortality in LMICs starts with better screening and education. Unlike other types of cancer, screening for lung cancer is not economical or justifiable on a population level. Instead, targeted screening of high-risk individuals is a practical way to promote early detection. Mobile CT scanners can help reach remote communities or individuals unable to travel. These screening efforts should also be paired with initiatives to help people quit smoking.
Transitioning from diagnosis to treatment, lung cancer survival in LMICs can improve via better healthcare coordination. Throughout the patient’s journey, treatment continuity is vital to improved outcomes and can be achieved by assembling multidisciplinary teams consisting of surgeons, radiologists, pulmonologists, and other specialists.
In 2015, there was an estimated worldwide shortage of over 1 million specialist surgical, anesthetic, and obstetric providers in 136 LMICs. Improved and expanded medical training will be necessary to equip local doctors who can treat patients, especially those in advanced stages of cancer.
In addition to physical infrastructure and personnel, updated electronic health record systems, cancer registries, and data sharing protocols will improve cancer care on a national and regional level. Sharing genetic and health data allows public health officials to monitor trends and tailor prevention and awareness strategies. This information also helps doctors choose the most effective treatment regimen for a particular cancer patient based off aggregated health data across providers. Regulatory bodies must play a role in establishing these registries in order to ensure appropriate levels of privacy, protection, and consent when sharing personal health data.
Access to affordable cancer drugs is a significant barrier for many patients in LMICs. BIO Ventures for Global Health (BVGH) oversees the African Access Initiative, which is a public-private partnership that aims to expand access to cancer medicine and technology. Through negotiations with international pharmaceutical companies, BVGH and other similar groups are able to help African countries acquire life-saving drugs at affordable prices.
Addressing lung cancer in the pursuit of healthy ageing
By 2050, nearly two-thirds of the world’s population over 60 years will live in LMICs. As we look to the future, we must prepare the necessary healthcare infrastructure to more accurately detect, effectively treat, and holistically care for cancer patients in LMICs.
Reaching this goal will require coordination between governments, industry, healthcare providers, and NGOs working within and across countries. The option of healthy ageing should not be sequestered to high-income countries, but be made available to everyone around the world.
Kevin Doxzen, Hoffmann Fellow, Precision Medicine and Emerging Biotechnologies, World Economic Forum
This article first appeared in World Economic Forum.
Also read: Third of India’s cancer cases linked to tobacco use, nearly half in people over 60: ICMR report