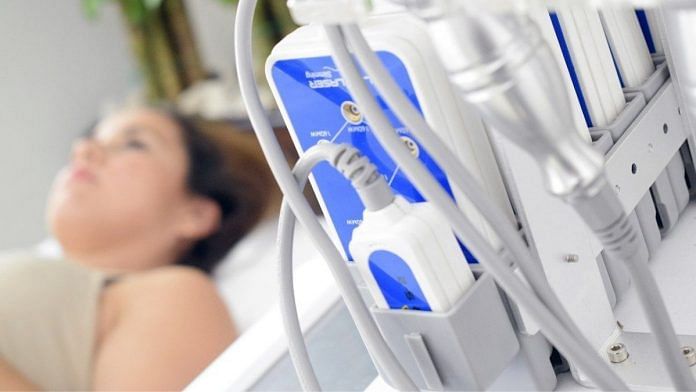
- High mortality rates for breast cancer patients are often due to late detection, particularly in rural areas where accessing reliable, affordable screening can be challenging.
- In resource-constrained settings, innovative technology-assisted solutions for detecting cancer could be the way forward.
- Analysing thermal images using AI-based algorithms, for example, provides a no-touch, no-radiation, low-cost way to accurately screen for breast cancer in such areas.
Breast cancer is the second most common cancer globally, and is the most commonly diagnosed cancer in Indian women. Of the 685,000 women who die around the world every year because of breast cancer, over 90,000 are in India, where cancer of the breast is the most common cause of cancer-related deaths in India. One of the major reasons for the high mortality rate in India is that most Indian patients present in the later stages of the disease.
Population-scale screening with early detection methods, and efforts to increase awareness of breast cancer, could help tackle the disease, improve survival rates and reduce treatment costs. Screening mammography is a widely used method, but its usage in low- and middle-income countries (LMICs) is limited due to equipment cost and the expert skill required for interpretation of mammograms.
Also, mammography has sensitivity of around 62% to 68% in women with dense breast tissue. Breast ultrasonography (USG) has demonstrated a greater sensitivity than mammography in younger women with dense breast tissue. However, USG is largely dependent on the skill and experience of the clinician. Additionally, due to India’s Pre-Conception and Pre-Natal Diagnostics Technique Act, which aims to prevent female feticide, a USG machine cannot be transported to be used as a community-based breast cancer screening tool.
As a result, the more affordable clinical breast examination (CBE) is the most common method for screening women in India because it does not require any equipment. It is more dependent on the healthcare worker performing the test, however. A shortage of more than 25,000 health workers means staff are already overloaded with maternal and child health, family planning and immunisation-related activities. In the absence of devoted, well-trained health workers and quality control, CBE can produce inconsistent results.
In a resource-constraint setting such as India, where the understaffed grass-root level health workers are overburdened and the radiologist to population ratio is as low as 1:100,000, innovative technology-assisted solutions could be the way forward.
Finding affordable, reliable solutions to detect breast cancer
Integrating technology such as medical imaging with artificial intelligence (AI) has shown promising results in various healthcare domains, including oncology. From improving the accuracy and speed of cancer diagnosis to optimisation of cancer treatment, the clinical applications of AI in oncology are many.
Several AI-based computer-aided detection (CAD) algorithms for screening mammography have reduced variability among radiologists and improved breast cancer detection rates. Google’s AI system interprets computed tomography (CT) scans to predict the likelihood of having lung cancer.
In resource-constrained settings, however, solutions that require expensive equipment such as mammography, CT scans, or magnetic resonance imaging (MRI) are not readily available. For example, in India, there are just 55 mammography machines at Government district hospitals to cater to 763 districts. Hence, there is a need for portable AI-based screening technologies that do not depend on extensive and expensive infrastructure. This would not only make preventive screening accessible and feasible, but also affordable.
Using AI-based technology to detect breast cancer
AI-based low-cost oncology technology innovations for LMICs already exist. MobileODT’s Eva System uses a patented AI algorithm to assess an image for the presence of cervical cancer. The image is taken with a mobile digital colposcope made from a smartphone equipped with a light source.
Niramai’s Thermalytix solution is based on the principle that highly active cancer cells create an area of higher temperature due to the enlargement of existing blood vessels and the formation of new blood vessel lesions. With today’s infrared cameras – which are portable and can be procured for a tenth of the cost of a 2D-mammography equipment – it is possible to measure these temperature variations with high precision and identify and characterise heat patterns generated due to breast abnormalities.
This non-radiation test creates a heatmap image, which the Thermalytix AI algorithm then analyses for temperature variations. This kind of automated quantitative test provides consistent interpretation and real-time reporting. It can be performed by a non-clinical trained technician who has basic knowledge of how to operate a laptop and a smartphone. This reduces the burden on the radiologist, who can now focus only on patients that require additional investigations.
Further, the Thermalytix test involves maintaining a distance between the technician and patient, making the experience private. This inherent distance is an added advantage during the current COVID-19 pandemic or any future situations involving communicable diseases.
Re-exploring thermal imaging
Though thermography as a screening tool was introduced way back in 1956, it has not been widely accepted to date. This is mostly due to the low sensitivity and specificity shown in past studies. However, with the latest advances in infrared cameras, the quality of thermal images has improved in the past 50 years. It is now worthwhile to re-explore thermal imaging, combined with AI, to provide a no-touch, no-pain, non-invasive test for an efficient, quick and comfortable screening experience.
A portable and affordable AI-based test such as this may be the solution to accessing reliable breast cancer screening in rural areas, which often have a medical centre but lack imaging equipment and/or radiologists. Such AI-based screening tests could positively impact the scalability of screening programs in LMICs and help reduce existing health inequalities.
Anita Borges, Vice Chairperson, Indian Cancer Society
Lakshmi Krishnan, Clinical Research Scientist, Niramai Health Analytix Pvt Ltd
This article was originally published on the World Economic Forum (WEF). You can read it here.
Also read: Early-stage breast cancer treatment to cost 10 yrs of average annual wages in India: WHO