A volleyball between the Narendra Modi-led government at the Centre and the states, between political incentives and health concerns, is leading to the loss of countless Indian lives in the intense second wave of the Covid-19 pandemic. Who is accountable for what and when is getting increasingly muddy. Public health is a state subject in India. Yet, there are elements of public health that have been led and managed by the central government. With a lack of policy clarity, transparency, and accountability between the Centre and states, India’s pandemic response has suffered. Where does the administrative and moral responsibility of this crisis rest?
As the vaccine supplier to the world, India hoped to provide Covid vaccines to several other countries. It is instead struggling to vaccinate its own population; currently facing an enormous supply gap. While the Centre has been controlling procurement and supply for the last several months, procurement has recently been liberalised, with states and private entities now allowed to buy vaccines directly. Some have lauded the move, because some states were previously not getting enough supply. But it’s worth examining where the solutions to the constrained supply really lie, what we are solving with decentralised procurement, and what new challenges might emerge.
Breakdown of Centre-state relations
The central government rightly controlled procurement of vaccines because public health responses (such as vaccination, especially in this context of positive externalities) are amenable to market failures. No other country in the world has allowed market forces to control this. Especially in a federal context, this may likely lead to increased inequities across and within states.
Not only has the price of the vaccine been increased for states — from Rs 150 per dose to Rs 400 in the case of Covishield — but the states are now required to fund this themselves. It is also unclear why the Centre and states are paying differential prices.
With variable fiscal contexts and vulnerabilities across states, is there not a real concern of this policy leading to inter-state inequities in access to the vaccine; if some states do not have the resources to purchase, or if inter-state competition for procurement results in some procuring more than their requirements (not unlike the situation at the global level across high-income and low-income countries)?
If states charge citizens for the current vaccines, or purchase higher priced vaccines like Pfizer and Moderna, intra-state inequities could be a distinct possibility. With strong positive externalities for the vaccines, can India afford such inequities, both from an individual and societal perspective?
There was a reason why procurement was centrally controlled. Historically, vaccines have been provided by the central government to states in a reasonably smooth manner, without concerns of competitive federalism. This was usually accompanied with a clear and transparent criterion for distribution across states. Similarly, the Covid-19 vaccination was planned as a centrally controlled task to ensure access to the country’s entire population; much like previous vaccinations and like other countries have done.
Unlike previous vaccinations, however, the lack of a transparent mechanism through which vaccines were being distributed across states, and the slow run rate in vaccination, led to some states expressing strong concern about the lack of adequate supply, and asking for greater autonomy in procurement; some of this a result of an erosion of trust between the Centre and the state. The challenge, however, was less about state autonomy, but more about the gaps in assessment and planning in the first place, resulting in inadequate supplies. The gaps in initial procurement commitments, advance purchase agreements, in the absence of which manufacturing capacity was perhaps not expanded to the required levels, contributed to current supply gaps.
At this critical juncture, however, does ensuring vaccination for India’s population no longer remain the responsibility of the central government, with the states having inherited a precarious situation, the outcome of which they may be accountable for?
Also read: The oxygen story exposes how India breathed too easy between the two Covid waves
Oxygen crisis
The scarcity of oxygen has taken many lives, but no one seems to be in charge, pushing a private hospital to file a case in the Delhi High Court over the lack of oxygen supply. It may be argued that this is the responsibility of states and private hospitals, which indeed it is. But isn’t the role of the Centre, especially during a national emergency, to prioritise national needs, take over planning, and enable inter-state coordination over life-saving resources?
As the steward for health in the entire country, the central government is well positioned to play a coordinating role across states, just as global mechanisms attempt to do the same across countries, specially for public health. A role that ensures that vaccines and oxygen — critical public health — reach all those who need it. The Centre is well positioned to undertake periodic planning and intervene, in collaboration with the states, to develop transparent mechanisms for distribution of vaccines to each state, rather than leave it to the market to determine who gets what. It would be more than unfortunate if state-level fiscal and capacity challenges, along with politics, are allowed to impact the safety and survival of our population.
The author is a Fellow, Lancet Commission for Reimagining India’s Health system. Views are personal.



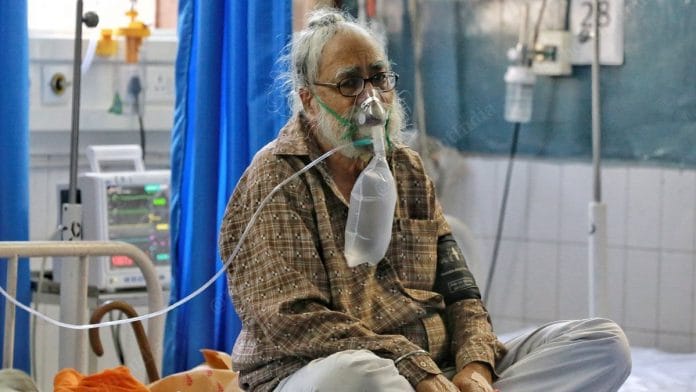


It’s sad to see the Centre-State fight when thousands getting died on a daily basis.
Fine column by Shri A K Bhattacharya for BS. From May 1, the states will become responsible for inoculating 600 million citizens aged between 18 and 44. Above 45 remains GoI’s domain. The vaccine itself will cost 400 / 600 per dose, adding upto about 60,000 crores, at a time when they are all fiscally stressed. The renewed lockdowns are throwing into doubt projections made for a swift economic rebound. The Union Budget was presented on February 1, at a benign phase of the pandemic. Even so, its 35,000 crore provision for vaccination, at 150 per dose, could have covered a billion Indians. 2. Seven states, including important ones like Maharashtra and Kerala, have announced free vaccines. The BJP has promised them for Bihar and Bengal. Difficult to see how any state government – Mr Ajay Bisht faces his voters less than a year from now – would find it politically feasible to charge for them. There is time for the Centre to sit with states and rework the strategy. Some things should be beyond politics. 3. Consider what has happened to India abroad. We proudly declined $ 100 million from the rulers of UAE after the floods in Kerala. Now even a bottle of oxygen is being gratefully accepted. There is some unhealthy speculation about why the Biden administration took so long to either talk or walk. Whichever way one sees it, the trajectory of New India is looking less promising than the old one.
Here is the best chance for all to eradicate the Covid-19 in this month of Ramazan, chosen to be the best month by One Almighty God with full of Blessings and Mercies. In Ramazan, Gates of paradise are opened, Gates of Hell are closed and the devils are chained up. What better time than any to draw closer to One God in the most blessed month of Ramazan and at at a time of greatest need to get rid of the Covid-19. As fasting in Ramazan is obligatory to all Muslims every year, it is not only a ritual to refrain from eating and drinking but it is an act of worship to get closer to God with dedication to feel the hunger of the hungry and help the poor with alms and charity who cannot afford their daily meals and necessities.
Since the fasting is also practiced and preached in other religions besides Islam, therefore the people of all religions must join together to fast in Ramazan with two billion Muslims to make it an unprecedented and unique opportunity to show the unity and solidarity to our One Almighty God by people of all religions by fasting and praying for common cause to get the virus eradicated from this earth. All the non-Muslims and Muslims got an golden opportunity to come together as never before to turn a new leaf to get success in this world and Hereafter on the basis of commonalities of major religions which clearly say in the religious scriptures of Hindus and Christians, Jews and Muslims that they there is Only One God, worship Him, Ekam Evadvitiyam, He is One only without a Second.There is only One God, worship Him, Ekam Evadvitiyam, He is One only without a Second.There is only one God, not the second, not at all, not at all, not in the least bit. There is no deity but God. The Lord our God is One.
In this most blessed month of Ramazan all good deeds are multiplied. The arrival of Ramazan at a time of calamity of Covid-19 gives a very good chance to the entire world to take full advantage of the Blessings and Mercies of Ramazan to call One Almighty God because the same One God belongs to all. So it is time for everyone to call upon One Almighty God without joining any partners, demigods, idols or Trinity to One God as this is an unforgivable sin.
Now, just imagine when if the billions pray, prostrate and grovel to One God by praying in this very month, certainly have an immense effect to be answered by One Almighty as we supplicate with one voice with tearfull eyes and hearts then we hope One Almighty God will do the rest to eradicate the deadly virus with His will as there is no might nor any power except with One Almighty God.
Random thoughts in the wake of such media reports which serve no real purpose…
It is a pandemic, not an epidemic or common flu. Things that will move the needle the most—are things that past events give us little to no guide about, especially a viral pandemic mutating fast and tomorrow it may mutate faster than the speed of light (figuratively) and be able to travel in the air. Hopefully it will not come to that and humanity will survive this pandemic. There will be unprecedented events. Their unprecedented nature means we won’t be prepared for them, which is part of what makes them so impactful. It is in each one’s hands to look after the self.
Nassim Nicholas Taleb writes in his book Fooled By Randomness:
“In Pharaonic Egypt … scribes tracked the high-water mark of the Nile and used it as an estimate for a future worst-case scenario. The same can be seen in the Fukushima nuclear reactor, which experienced a catastrophic failure in 2011 when a tsunami struck. It had been built to withstand the worst past historical earthquake, with the builders not imagining much worse—and not thinking that the worst past event had to be a surprise, as it had no precedent.”
Good decisions are not necessarily about making good decisions, they are about repeatedly not screwing up. The most impactful part of a plan, especially in conditions like a pandemic, is planning on the plan not going according to plan. It is hard to maintain a mindset that can be paranoid and optimistic at the same time Seeing things unfold takes less effort than accepting nuance. But you need short-term paranoia to keep you alive long enough to exploit long term optimism.
Dependence or reliance on past data as a signal to future conditions in a pandemic is a direct trap. We need to be proactive to events unfolding. That which can be technically true can be contextually nonsense. For instance, it may be, technically, a good decision to vaccinate all above 18 at the earliest. But contextually chaos will unfold at vaccination centers from May1, with unprecedented rush – registration notwithstanding.
In your fight against the pandemic, start with the self, family, community you live in, people who depend on you and on who you depend and so on. Have close WhatsApp groups. In your groups, carry honest stories on the pandemic that is happening in your area of influence, how people act and react as prevention, what they do for their work, etc… There are more relevant lessons to take away from this kind of close observation than there are in studying the extreme characters that tend to dominate the news.
Tail piece: Nothing is as good or as bad as it seems