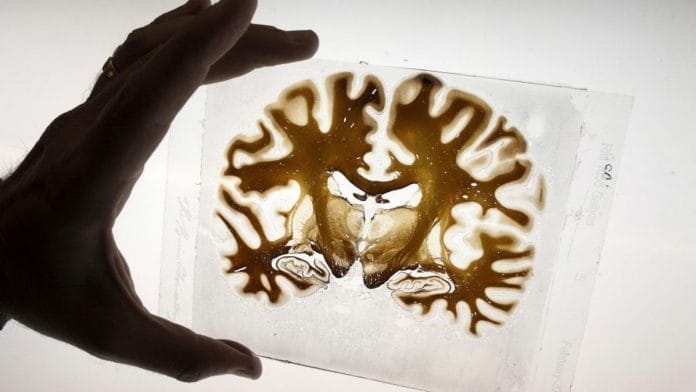
Recent research from the U.K. on the health effects of Covid-19 found that even mild cases could cause significant changes to the brain. Sam Fazeli, a Bloomberg Opinion contributor who covers the pharmaceutical industry for Bloomberg Intelligence, answers questions about this development and the implications of the findings. The conversation has been edited and condensed.
These findings on Covid-19’s impact on the brain sound troubling. What are the details?
The U.K. has been running an incredible project called UK Biobank involving half a million adults ranging in age from 40 to 69. They provide regular blood and other samples, as well as detailed health information plus thousands of scans, including brain images using MRI. This has allowed researchers to conduct one of the most rigorous analyses of the effects of Covid on the brain. What makes the data especially powerful is that they compare brain images before and after a Covid infection in the same people. So what did it show? Even mild cases of Covid led to loss of volume in certain areas of the brain, specifically those involved in processing smell and taste. But they also found statistically significant brain volume loss in the gray matter — the thin layer on the surface of the brain that contains most of the neurons — in other areas involved with memory formation. The authors speculate that this raises the possibility that even mild cases of SARS-Cov-2 infection can have deleterious effects that may last long past the period of infection.
What makes this research stand out from other Covid research?
As noted above, the particularly important thing about this data is that it was generated using subjects as their own “control” because there were images available from before they contracted Covid to use as a comparison. Further, this kind of “longitudinal” analysis allowed them to discover something else they might not have otherwise: people who were diagnosed with Covid had a smaller thalamus to begin with than those who did not. Without having access to brain images of people before they got Covid, one would have concluded that Covid infections lead to the loss of thalamic neurons. But in fact they found that all those who got Covid already had smaller thalamic regions before the infection, so this has nothing to do with the infection itself. Of course, it does raise the question as to whether people with a smaller thalamus are more susceptible to Covid or it just an odd association without any relevant causal relationship.
Is this finding unique to Covid, or has it been found in other viral diseases?
There are other viruses that infect the nervous system, such as measles, HIV, herpes and polio, and as we know these can have dire consequences. But the only other common respiratory virus that I know of that can infect the brain, aside from coronoviruses, is the respiratory syncytial virus. But these mostly manifest as seizures and brain inflammation. It’s important to note that volume changes are only one of the potential brain conditions caused by Covid infection. There is also the increased risk of seizures, strokes and Guillain-Barre syndrome. But the issue with brain volume loss, if shown to last much longer beyond the period of infection, is a significantly bigger problem given it happens in even mild cases of Covid.
How does this change your view about managing Covid?
I had been wondering when we will get over our obsession with case counts and focus more on hospitalizations and deaths, given that vaccines are very effective in reducing the latter as compared with mild infections, especially with the rise in variants. But if even mild cases cause issues that store up real morbidity for the future, then we should continue to be obsessed with crushing even mild cases of Covid.
Could this brain condition be linked to some of the reported “long Covid” symptoms? Which ones come to mind?
Some of the issues reported with long Covid are directly related to the pathology of Covid-19 disease. These include shortness of breath as a result of lung damage, chest tightness, joint pain, etc. But the “brain fog” that is one of the key issues reported by those suffering long-term consequences after a case of Covid could be related to exactly what this new research has found.
Is it more a problem because of the possible long-term impact or more because of how little we know about its impact and the sheer number of potentially affected people? Can it be treated?
Last question first: probably not given that I don’t think there is anywhere near a clear understanding of what the mechanism behind the brain volume loss is. And you’re right, the problem is that we don’t know how many of the 180 million people worldwide are suffering from this or have increased risk of dementia or longer-term issues.
Were the effects magnified in any particular type of person?
There was no obvious link to age, but the majority of people in the study were in the older part of the age range of participants in the Biobank.
Anything else?
We need a lot more research to understand the longer-term issues resulting from Covid. Until we do, we should try our best not to have to “live with the virus” as some politicians have said. We should aim to get as close to zero cases as possible. And for that we need to be one step ahead of the virus, which includes much higher levels of genomic surveillance. We have a very long road ahead of us. -Bloomberg
Also read: Covid can cause loss of brain grey matter in recovered patients, Oxford researchers find