New Delhi: Each time Girja Sharma stumbles upon someone not wearing a mask, she gets irritated and frustrated.
“It feels very irritating. People are being so careless because of which, others have to suffer,” she explained her annoyance.
Sharma is the chief nursing officer in Fortis Hospital, Shalimar Bagh, New Delhi, and has spent every waking moment battling the coronavirus pandemic this year.
Nursing staff has been at the forefront, quite literally, of combating the lethal virus. The year, however, has been punctuated with confusing protocols on Covid treatment initially, lapses in healthcare infrastructure, and no work-life balance, not to mention the unbearable PPE suits.
Nursing staff across the country shared their experiences of with the outbreak and how it has been different from other epidemics. The pandemic, they said, was accompanied by an intense pressure when it came to nursing Covid patients, the psychological toll of isolation and the annoyance of seeing people being careless despite the magnitude and seriousness of the pandemic.
The initial mess of early Covid days
In the first few months of the pandemic, nurses and other healthcare workers were caught unawares as there wasn’t much information available about the novel coronavirus.
“Through my career, I have seen many other contagious diseases and we were aware of how they spread. But, no one was aware of how Covid spread. There was a lot of confusion, even the guidelines for treatment used to change daily,” Sharma explained. She said it was a “total mess” in the initial days of the pandemic.
Loveleen Sunil, chief of nursing services at Columbia Asia Hospital in Palam Vihar, Gurugram, recalled that she had witnessed the treatment of swine flu, but the confusion brought that came with the Covid pandemic was unseen before.
“I had to manage a team of nurses wherein everyone was fearful, angry and refusing to work. Some nurses also threatened to resign from the job, but all that had to be handled,” Sunil said.
With each day, protocols kept changing, making it difficult for nurses to rely on one course of treatment. Sunil recalled how she stood by the bedside table of a Covid patient even though she was “terrified”. She was determined to show her team that she was fulfilling her duty.
“If I had shown that I am terrified, the team would have fallen apart,” she said.
Also read: Doctors, nurses have final responsibility to protect themselves from Covid: Govt to SC
A hazmat & mask-covered personal touch
Dhanya, a nurse from a Covid-19 ward in Bengaluru’s Columbia Asia Hospital, located in Whitefield, remembered the emotional toll she felt when dealing with a 65-year-old patient who had been in the hospital for 2-3 days.
“One day, I went in to check her vitals and found that she was crying,” Dhanya said. She was feeling really lonely and was unable to interact with her family due to visitor restrictions.
“When I went into her ward, she held my hand and told me that I was her daughter. It became very difficult for me to handle the situation,” Dhanya recalled.
Typically, each patient is provided an attendant for their needs. But, in the case of Covid-19, it isn’t possible to assign one attendant to each patient, which increased the workload on nurses as they had to perform the duties of attendants too.
“Nurses always carry the fear of getting infected… but we don’t have a choice. It is our duty to provide to the sick,” said Katherine Jacobs, chief nursing officer, Paras Hospital, Gurugram.
Jacobs revealed that the frequency of call bells also increased from Covid-19 patients.
“Lack of information creates many problems. Nurses have to constantly reassure the patient and address their queries. The frequency of call bells increases since patients admitted are alone in their rooms,” she said.
Nursing staff also struggled with not being able to comfort patients in the same way as other patients. Jacobs said that a distance had to be maintained from the patient.
Nurses are hailed for providing the personal touch in the healthcare system. But, when it came to Covid-19, a hazmat suit that ensured only the eyes were visible came between nurses and their patients. To tackle this, many started marking their names on PPE kits.
Others recalled facing trouble communicating with patients since the mask would muffle voices.
The lack of communication resulted in patients becoming restless, which inevitably added to the challenges nurses were facing.
“Patients have become very demanding recently. They demand things like everything is normal and there isn’t a pandemic going on,” Sharma said. This often led to nurses undergoing severe stress, she added.
Further, since patients couldn’t meet their families, they tended to take their “frustration out on nurses” and yell at them, said Sharma.
A staff crunch only compounded all these issues.
Sharma told ThePrint that earlier, the ratio of nurses to patients was 1:5 in normal wards and 1:2 in critical care units. However, after the pandemic, the ratio has been stretched to 1:12 in normal wards and 1:5 in critical care.
Psychological toll
Asked to describe the most cumbersome aspects of battling the pandemic, surviving in the PPE kit and quarantining are at the top of the list for these nurses.
Those of them in Covid wards haven’t met their families since the beginning of the pandemic. For instance, in Fortis hospital in Delhi’s Shalimar Bagh, nurses haven’t been able to go back home since April. The hospital has instead put them up at a hostel.
In most hospitals, nurses operate on shifts that include seven days of duty, followed by seven days of isolation.
Ammu Paulose, a ward nurse at Columbia Asia Referral hospital in Bengaluru, said: “Quarantining myself has been the most terrible thing I have had to do.”
Dhanya, too, shared this sentiment. “Isolation is truly the worst thing to experience because we can’t go out or mingle with people.” She said she hung out in the hostel allotted by her hospital, where the nurses chat with each other and share their daily experiences of treating Covid.
Paulose also described that since patients can’t meet their loved ones, it has put immense pressure on nurses to cater to their emotional well-being. Even those who have been able to meet their family, fear for their safety.
Sunil at the Palam Vihar hospital said, “My kids are around 15 years old. I am constantly scared that I am carrying the virus and will pass it on to them.” She expressed concern over how she couldn’t even hug her children and had to keep them at a safe distance.
The seven days of duty are accompanied by wearing the PPE kit for at least six hours daily.
For Dhanya, wearing the PPE kit has been the most “horrible thing” to do. “Wearing PPE is cumbersome, we can’t empty our bladders. It also becomes difficult when women are on their monthly cycle or periods,” said Sharma.
Also read: ‘Fighting in the frontline without fear’ — Nurses discuss Covid situation with Rahul Gandhi
Death looms daily
With the virus having claimed 1,44,789 lives so far, death has become a daily occurrence for the nursing staff.
Neetu Maitra, chief of nursing at the Indian Spinal Injuries Centre, New Delhi, said: “Sometimes even after the best treatment, it isn’t possible to save our patients.”
“Patients are in such conditions where they are battling for their life … it is horrifying when someone is battling for a single breath,” she added. Often the job becomes difficult since nurses have to answer queries of family members knowing that the patient isn’t going to survive.
While dealing with death is indeed part of the job, Jacobs pointed that dealing with a Covid death is different. “Dealing with a Covid death is a new thing because formalities are different,” explained the chief nursing officer at Paras Hospital in Gurugram.
In most cases, healthcare staff and relatives can’t even see the face of the deceased. She also recalled the “hopelessness” in most patients’ eyes when they realise the consequence of the disease. It is hard to get over such kind of “emotional trauma”, she said.
‘People being careless must visit Covid wards’
One things all nurses were in staunch agreement was how people’s carelessness in following Covid precautions was adding to the problem.
Maitra said that each time she saw someone not wearing a mask, she wanted to take them to a Covid ICU ward to show them the harshness of the disease.
“We do everything to save them (patients), but sometimes, it’s just not possible. I want common people to see that,” she said.
Jacobs has different approach. “If I see anybody violating Covid guidelines, I always stop by and ask them to take precautions and also tell them they have a casual attitude towards Covid.”
Sunil, meanwhile, reminded us that the virus hasn’t left the country yet. Each day the hospital receives a positive report. It is as much a threat right now as it was in March, she said.
Also read: This Delhi doctor doesn’t wear full PPE when treating Covid-19 patients. Here’s why



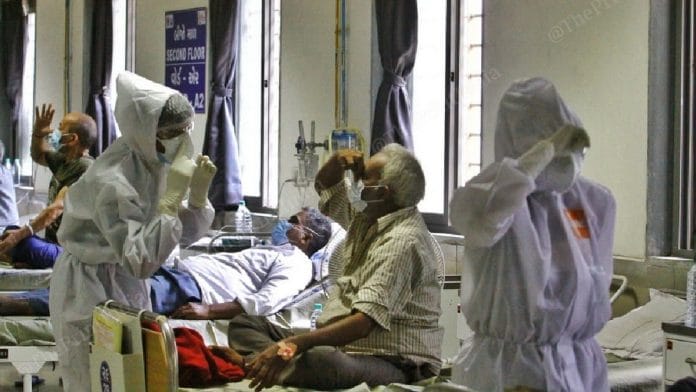


The one who shares the major burden doesn’t get enough appreciation and support. Feeling so sorry for these nurses. May they overcome !
First hand out free good quality masks in every ward, every house should get 4 masks free everyday, if people still casually behave like animals then they need to be treated as such, with a solid beating and a fine. There is already fatalism in India, add to that, reckless casual behaviour plus “it’s not my problem” culture, it becomes a toxic mix.