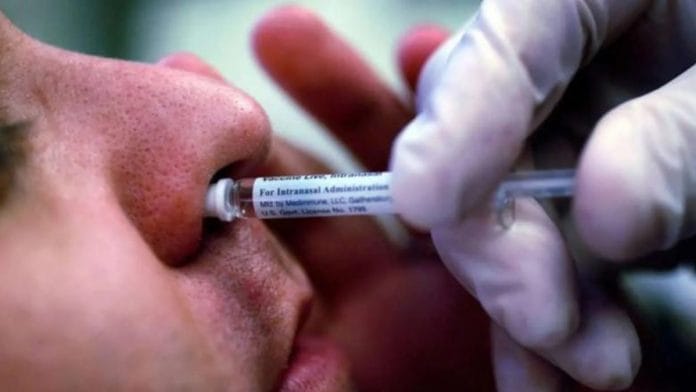
Bengaluru: Hyderabad-based Bharat Biotech is set to launch Phase 3 clinical trials of its nasal Covid vaccine after receiving regulatory approval from the Drugs Controller General of India (DCGI). The vaccine, intended to induce mucosal immunity, will be administered as a booster dose.
Because the mucous membranes are the first line of defence against pathogens, an immune response can be produced at the site of entry for the virus, should the trials succeed, preventing it from infecting the body further.
The development of mucosal vaccines for Covid has been spurred on by the success of the oral polio vaccine (OPV), which induces mucosal immunity in the gut that helps eliminate the polio virus, which spreads through contaminated food and water.
What is mucosal immunity?
Mucosa are the wet tissues that line the nose, airways, mouth, and digestive tract, triggering the first immune response from this region.
The immune response cells here, leukocytes or white blood cells called granulocytes, regulate the inflammatory response by the immune system. This is the system that kicks into action during allergic reactions, including asthma. Mucosal cells are constantly exposed to pathogens because they are exposed to the outside, and are the point of interaction between the physical body and the outside environment.
Because mucosal cells are so important to the body’s defences, they contain the majority of immune cells. The mucosal immune system is the largest component of our bodies’ immune systems. The body’s defensive cells, T cells and B cells (which produce antibodies) reside in the mucosal lining in the respiratory, gastrointestinal, and urogenital tracts.
The human immune response is of two types, innate and adaptive. The former is generic to pathogen and kicks into action at any point an antigen or foreign particle is detected. Data from this immune response is used to tailor a more specific one, which gets induced a few days later when a pathogen is new — the adaptive response. The innate immune response produces IgA antibodies, while the adaptive produces IgG antibodies.
Because IgG are more specialised and targeted, they are able to neutralise any pathogen quickly and more effectively, without much damage to the body. Traditional vaccines aim to enhance the efficiency of these antibodies. As booster shots, mucosal vaccines elicit a systematic immune response faster.
But mucosal vaccines additionally also attempt to make the IgA antibodies more efficient so that the virus can be stopped and neutralised at its point of entry itself. IgA antibodies are produced in a higher quantity than other antibody types combined, and could thus be utilised for better defence.
These IgA antibodies dominate the nasopharyngeal pathways where the SARS-CoV-2 virus enters the body, all the way up to the tip of the lungs where the oxygen enters the bloodstream — the alveoli — after which the IgG antibodies start to dominate.
Unlike response from a traditional vaccine, which prevents severe disease but not infection or transmission, mucosal vaccines can be effective at potentially preventing both infection and lowering transmission.
Also read: What causes long Covid? US study finds 4 factors, including viral load & Type-2 diabetes
Advantages of mucosal vaccines
Mucosal vaccines are nasal or intranasal, and are not injection-based. They are provided through the nose.
Muscle-based injection vaccines enter the bloodstream directly, while mucosal vaccines are able to immediately elicit a response in the mucous membrane, at the first point of contact. When the body comes in contact with the virus, this helps in reducing the time available to the virus to multiply in the body.
Since the SARS-CoV-2 virus enters the body through the upper respiratory tract first, the immune system first interacts with the virus at the respiratory mucosal surfaces.
The IgG antibodies produce an inflammatory response, which can be avoided through an IgA-dominant response.
Traditional vaccines focus on antibody-producing B cells and also the T-cell response, which produce cytotoxic T cells that kill infected cells and prevent further multiplication.
Intramuscular vaccines do not focus on improving neutralising mucosal response, which could prevent the virus from latching on to cells.
It is thought that without a robust mucosal response, injected vaccines are less likely to produce sterilising immunity, where, upon coming in contact with the virus, the body eliminates it entirely before it can infect cells.
Mucosal vaccines are also easier to produce and store.
(Edited by Neha Mahajan)
Also read: Covid will return ‘like the flu’ after Omicron, but won’t be a pandemic: US researcher in Lancet