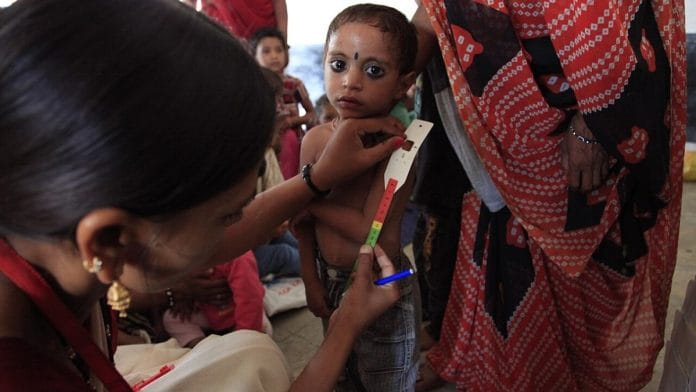
New Delhi: A four-year Indian Council of Medical Research (ICMR)-led trial has been launched in six states to tackle child malnutrition in the first three years of life. The initiative will test whether redesigning Anganwadi take-home rations (THR), paired with structured counselling for mothers, can reduce the number of underweight children aged 6 to 36 months as well as stunting and wasting among them.
The study, whose protocol was published in the Frontiers in Nutrition journal in March 2026, is currently in the first phase.
The study, NECCTAR/Nutritional Status Enhancement of Children through Behaviour Change Communication and Take-Home Ration, is part of the ICMR’s National Health Research Priority Projects. The initiative funds large, multi-state research across 11 focus areas with grants of up to Rs 25 crore per project, aimed at directly informing policy. These areas include antimicrobial resistance, tuberculosis, cancer, mental health, and nutrition.
The trial will run in Karnataka, Madhya Pradesh, Maharashtra, Meghalaya, Odisha, and Rajasthan—one district per state. The six sites were chosen to represent different dietary practices and existing THR models, which state governments currently supply.
Take-home rations are dry, pre-packaged food supplements—typically given to children, pregnant women, and lactating mothers once or twice a month through Anganwadi centres under the Integrated Child Development Services (ICDS) scheme, which was launched in 1975.
The rations, usually comprising a cereal-pulse blend or energy-dense mix, are to be prepared at home as a porridge or similar preparation and fed to young children as a complement to breastfeeding. Each state designs its own formulation.
The trial is based on decades of evidence that improving complementary feeding for young children is necessary to improve the situation around stunting and wasting. According to the latest National Family Health Survey, 35.5 percent of Indian children, under five, are stunted, and 19.3 percent are wasted—both above the World Health Organization thresholds for a public health emergency.
Stunting, or low height for age, reflects chronic, long-term undernutrition and is largely irreversible after age two. Wasting or low weight for height reflects acute undernutrition and sharply raises the risk of death from common infections. On the other hand, the term underweight captures children who weigh too little for their age and is often a composite of the above two health conditions.
“There is a very rapid increase in childhood undernutrition after exclusive breastfeeding ends,” said Dr Bharati Kulkarni, Director of ICMR–National Institute of Nutrition (NIN), Hyderabad, and co-author of the study. “This is the period when children require complementary foods with enough energy, protein, and micronutrients to support their rapid growth and development—and that is the area which has been a big concern.”
The problem, she said, is not just what is in the ration packet but what happens to it after it reaches the home. Rations are state-specific, vary in composition, and are handed over to mothers to prepare and feed children correctly and consistently over weeks.
“We feel there is a big gap—children are not getting the optimal quantity and quality of take-home foods essential for preventing growth faltering,” Dr Kulkarni told ThePrint. “To strengthen this programme, the trial has been undertaken.”
Trial in three phases
According to the study protocol, NECCTAR is structured into three phases over 48 months.
Researcher teams in each of the six districts will spend six to seven months in the field, tracing the journey of take-home rations from procurement to households. They are mapping the supply chain, documenting what children are actually being fed, and speaking with everyone in the system—mothers, Anganwadi workers, vendors, and local health officials—to get context-specific insights on the composition and quality of rations reaching the child. Researchers will also chemically analyse existing ration batches in accredited laboratories to assess their actual nutritional and microbiological profile.
The formative phase will also identify what is already working: researchers will specifically seek out mothers of well-nourished children in the same communities to document what they are doing differently, and use those practices as the basis for their counselling strategy.
In the second phase, the findings will be used to design two to three improved ration formulations, built around locally available, nutrient-dense ingredients, and developed in the presence of mothers and community members so that families will actually use them.
The formulations will meet the revised nutritional norms notified under the National Food Security Act in January 2023—standards that go beyond basic energy and protein to include the quality of fat, carbohydrates, and seven key micronutrients. A behaviour change communication strategy will be developed in parallel.
Before deciding on the final recipes, five one-week cycles of real-world household testing—giving families the improved rations to prepare and feed, with inputs obtained on taste, texture, ease of preparation, and actual consumption. This iterative process, known as ‘trials of improved practices’, is designed to weed out formulations that look good on paper but fail in the kitchen.
The third phase is the trial itself. Anganwadi centres will serve as implementation units, with clusters defined at the level of health sub-centres to minimise contamination. The study will assess impact at both individual and population levels—tracking a cohort of children aged 6–18 months over 18 months, while conducting repeated cross-sectional surveys of all children aged 6–36 months at regular intervals. The intervention will be delivered through the ICDS platform by frontline workers, supported by health staff, while control areas will continue standard services.
Also Read: In a small town in Gujarat, researchers are training AI to detect anaemia, without drawing blood
What counts as success
The study will track results for two groups of children: one from before the intervention started and another from the start. The latter group will be checked every six months, at 6, 12, 18, and 24 months.
The children, who will be followed from before the intervention, will be examined for changes up to 18 months, with an additional check at 24 months for any longer-term impacts. For the others, results will be compared from the start to the end of the study, while trends will be checked at regular six-month intervals.
The trial will also use a standard WHO measure called ‘weight-for-age z-score’, or WAZ, to judge whether the intervention worked. The score captures how a child’s weight compares to a global reference for healthy children of the same age and sex. A score of zero means the child weighs exactly what a healthy child of their age should. A score of minus two or below—two standard deviations below the norm—is the threshold at which a child is classified as underweight.
The trial has been designed to detect a difference of 0.3 in this score between the two groups of Anganwadi centres after 18 months. Now, that may sound modest, but it is the shift that similar nutrition trials in comparable settings have consistently achieved—and it is what the researchers have modelled the study to reliably pick up on.
Beyond child growth, the trial will also calculate cost-effectiveness—what it actually costs the government per child to achieve that improvement. That figure will provide policymakers a concrete basis for deciding whether to scale the model through the existing ICDS network.
“We have to generate evidence that the optimised formulation of the take-home ration, along with behaviour change communication, results in improvement in child growth. That is the primary purpose,” Dr Kulkarni added.
Behavioural change at the centre
The counselling component of NECCTAR is designed around a simple but important insight from research literature. The same ration packet performs very differently depending on who receives it, how it is prepared, and what the family believes about it.
Along with packet distribution, the Anganwadi workers in these intervention clusters will counsel caregivers during home visits, using pictorial guides on feeding frequency, portion size, and hygiene, running cooking demonstrations with the improved recipes. The strategy will also engage fathers, grandmothers, and community leaders, recognising that feeding decisions in most households are rarely made by the mother alone. Community mobilisation campaigns, locally produced videos, and radio content have also been planned.
The intervention will be delivered entirely through the existing ICDS platform: Anganwadi workers and helpers actively engaged with state governments.
If the trial shows positive results, Dr Kulkarni said, the next step would be to work with state governments on implementation research before the actual implementation using the same network.
The government has already laid some groundwork. In 2021, the Ministry of Women and Child Development subsumed the old ICDS scheme into a larger umbrella programme called Mission Saksham Anganwadi and Poshan 2.0—one of the world’s largest nutrition and early childhood care initiatives. In 2025-26, the mission consolidated the supplementary nutrition programme, the Poshan Abhiyaan behaviour change drive, and the Scheme for Adolescent Girls under a single framework, with a budget allocation of Rs 21,960 crore.
It introduced the Poshan Tracker, a digital platform for monitoring THR delivery in real-time through Aadhaar verification and QR codes, and mandated upgrading of Anganwadi centres into modernised Saksham Anganwadis. The mission specifically focuses on maternal nutrition, infant and young child feeding norms, and treatment protocols for severely and moderately malnourished children.
“First, we have to know that it is effective so that policymakers get evidence on what works and what does not. After that, the evidence is there, and then the next step is to scale up in the real world through the existing programmes,” Dr Kulkarni said.
(Edited by Madhurita Goswami)
Also Read: A 5-spice mix to fight long-term diabetes & obesity complications? ICMR set to back human trials