New Delhi: Despite a burgeoning mental health crisis, India has seen significant underspending of funds meant for central and state mental health programmes over the past five years, with government data showing states and Union territories spent around 50 percent of allocated funds.
According to data presented in Lok Sabha on Friday by Minister of State for Health and Family Welfare Pratap Rao Jadhav, in five years between 2020-21 and 2024-25, states and Union territories spent Rs 328.27 crore out of Rs 691.24 crore approved under the District Mental Health Programmes (DMHPs), about 47.5 percent of the total allocation.
DMHP activities are run by states and UTs. It involves running outpatient psychiatric services, community outreach, awareness campaigns, and training of healthcare workers in districts.
According to the data presented by the minister, allocation and spending have gone up under the DMHPs, but utilisation as a percentage of allocation has remained around 50 percent every year since 2020-21.
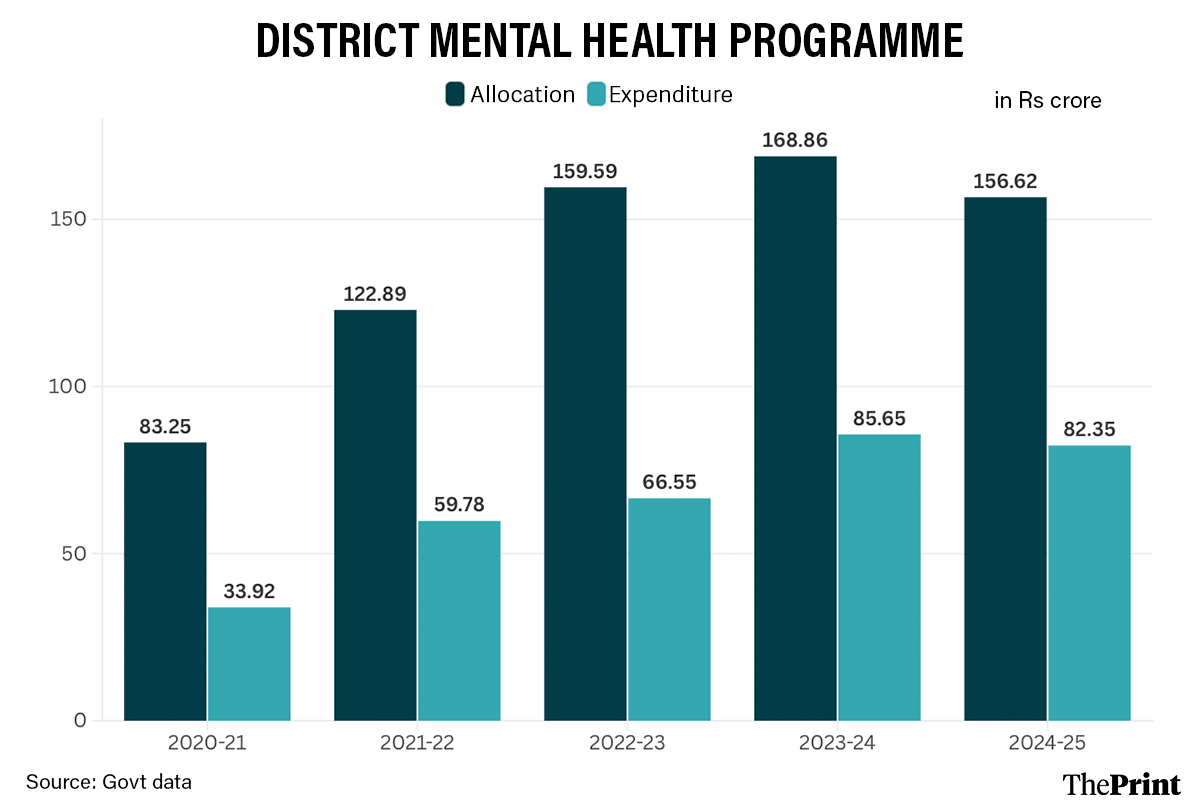
In 2020-21, a cumulative Rs 83.26 crore was approved for the programme for all states and UTs, but only Rs 33.92 crore was spent. In 2021-22, approvals jumped to Rs 122.90 crore, but spending was only Rs 59.78 crore, roughly 49 percent of the sanctioned funds.
In 2022-23, Rs 159.59 crore was approved and Rs 66.55 crore spent.
The next year 2023-24, approvals rose again to Rs 168.86 crore, while expenditure stood at Rs 85.65 crore, about 51 percent utilisation, the highest in the five-year period but still only about half of the available funds.
In 2024-25, states and UTs spent Rs 82.35 crore out of Rs 156.62 crore approved.
Dr. C Naveen Kumar, Professor of Psychiatry at National Institute of Mental Health and Neurosciences (NIMHANS) Bangalore, told ThePrint, “Since health is a state subject, if states utilise funds quickly and submit utilisation reports on time, the Centre can release additional funds as required under the programme framework.”
Bhopal-based public health researcher Anant Bhan said the state’s inability to spend even what is allocated is hurting the fight against mental health problems at the grassroots level.
“A major proportion of the union mental health budget is spent on tertiary apex care institutions like NIMHANS. The funds available through the DMHP allow for a focus on a key area in mental health: primary and secondary care,” he told ThPrint.
“These (DMHP) funds are meant to cover the cost of running the programme: screening, diagnosis and linkage to care for those with mental illness, community-based outreach services, and mental health awareness activities (which contribute to destigmatisation),” he said.
Bhan said the underspending combined with the “shortage” of mental health specialists is a cause for concern, “Better fund utilisation to enhance quality mental health services and decentralised care models through approaches such as task-sharing need to be looked into,” he said.
Also Read: Budget and Economic Survey signal clearer mental health crisis recognition
Tracking NMHP expenditure
The data presented in Parliament shows significant fluctuations in spending under the National Mental Health Programme (NMHP). The last financial year’s expenditure was only 16 percent of the budget estimate of nearly Rs 31 crore.
The numbers were even starker in 2018-19 and 2019-20 when the respective expenditures were just about 1 percent and 4 percent of the budget estimates, hitting mental healthcare initiatives across the country.
Launched in 1982, the NMHP is the Union government’s main scheme to expand mental health services across the country. It focuses on training specialists, strengthening psychiatric departments in medical colleges, and running district-level services through the DMHP so that treatment becomes available closer to people’s homes.
Dr. Kumar of NIMHANS Bangalore explained that under NMHP, there is scheme A, which covers Centres of Excellence, and Scheme B, which is for upgrading psychiatry departments across the country.
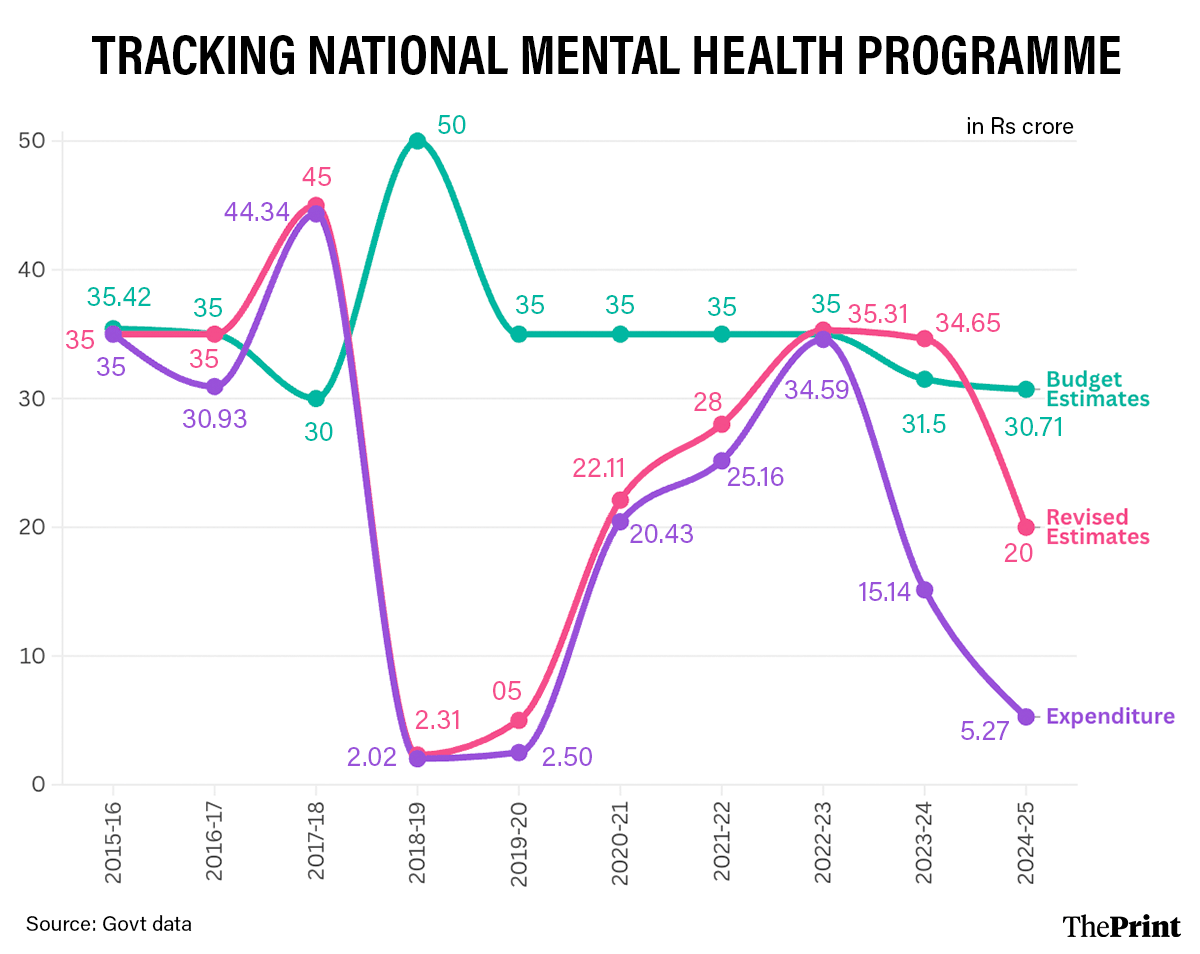
Over the past decade, the programme’s Budget Estimate stayed close to Rs 35 crore for several years, with Rs 35.42 crore in 2015-16. Spending had also been relatively high in the initial years of the decade—Rs 35 crore in 2015-16, Rs 30.93 crore in 2016-17, and Rs 44.34 crore in 2017-18.
However, expenditure dropped sharply after that. In 2018-19, the revised estimate was cut to Rs 2.31 crore from the budget estimate of Rs 50 crore, and only Rs 2.02 crore could be spent. In 2019-20, spending remained very low at Rs 2.50 crore, despite a Budget Estimate of Rs 35 crore.
Expenditure improved again in later years, reaching Rs 20.43 crore in 2020-21, Rs 25.16 crore in 2021-22, and Rs 34.59 crore in 2022-23.
But the trend again weakened, with Rs 15.14 crore spent in 2023-24 (when the Budget Estimate was Rs 31.5 crore), and merely Rs 5.27 crore in 2024-25 against the Budget Estimate of Rs 30.71 crore, according to the parliamentary reply.
Explaining the drastic drop in expenditure in the previous financial year, Dr Kumar said this reflects lower utilisation by institutions receiving funds under Scheme A and B. “If institutes ask for funds, they will be given. The revised estimate depends on utilisation reported by the Centres of Excellence.”
Rising need
The spending gaps come at a time when mental health problems are becoming more common in India and across the world.
The COVID-19 pandemic led to a sharp rise in mental health problems globally. According to the World Health Organization, the global prevalence of anxiety and depression increased by about 25 percent in the first year of the pandemic. The rise was linked to factors such as social isolation, fear of infection, financial stress, and disruption of daily life.
Stigma remains one of the biggest barriers to mental health care in India, particularly among the middle and upper-middle classes, said Dr Rajesh Goyal, senior consultant psychiatrist at Sir Ganga Ram Hospital in New Delhi.
He also said that environmental and social changes are contributing to rising mental health concerns. Air and noise pollution in large cities affect mental well-being, he said.
He added that the decline of joint family systems and increasing social isolation have reduced avenues for emotional support.
“Earlier, people had family members and neighbours to talk to. Today, many young people feel isolated and do not have anyone to share their problems with,” he said.
Goyal further noted that increased exposure to violent or distressing content on digital platforms may also be affecting mental health, particularly among younger populations.
The National Mental Health Survey (2015–16) conducted by the National Institute of Mental Health and Neurosciences found that 10.6 percent of adults in India were living with a mental disorder at the time of the survey. The study also estimated the lifetime prevalence of mental disorders at 13.7 percent, meaning roughly one in seven Indians may experience a mental health condition at some point in their lives.
India also faces a shortage of specialists. The government told the parliament in its response that the availability of psychiatrists in the NMHS states varied from 0.05 per lakh population (Madhya Pradesh) to 1.2 per lakh population (Kerala).
As per the WHO, Mental Health Atlas 2020, the global average of availability per 1,00,000 population is 1.7 psychiatrists.
The government said it has tried to address the shortage by increasing the number of medical colleges and postgraduate seats, and by setting up Centres of Excellence in mental health to train more specialists.
(Edited by Ajeet Tiwari)
Also Read: Why banning social media for kids risks misdiagnosing the problem