Thank you dear subscribers, we are overwhelmed with your response.
Your Turn is a unique section from ThePrint featuring points of view from its subscribers. If you are a subscriber, have a point of view, please send it to us. If not, do subscribe here: https://theprint.in/
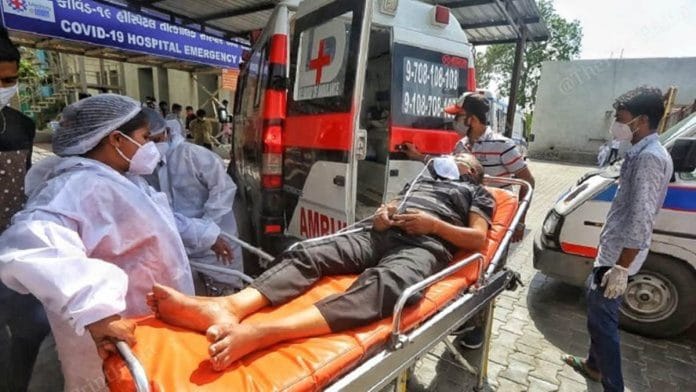
India witnessed a massive second surge of Covid-19 cases since March, 2021 after a period of decline from September 2020. With 30,585,229 cases reported and 402728 deaths, it is time to assess where India went wrong and what is needed to avoid another surge or virus outbreak.
ICMR, which spearheads the Covid-19 pandemic in India, is neither a statutory body nor a regulatory body in India. NCDC, unlike CDC of USA, has taken a back seat in the fierce battle fighting Covid-19. NCDC needs real teeth to fight impossible fights. Hence, it should be transformed as an autonomous statutory body to monitor, intervene, and stabilize (overriding state governments) any health crisis stemming from anywhere in India. NCDC should have a sizable purse, a separate dedicated ground force like CBI, with district-wise offices, and constitutional authority to inspect, quarantine victims and ensure the production and distribution of vital drugs and vaccines across India. After Tsunami, then-PM Dr. Manmohan Singh had created NDRF, and this pandemic warrants a National Health Crisis Response Force consisted of doctors and other health professionals under the umbrella of NCDC.
When the Covid-19 pandemic started, India had just one BSL-4 level laboratory at the National Institute of Virology (NIV) in Pune for a nation of 1 billion people. India had largely depended on isolating and identifying the SARS-CoV-2 virus from US and EU labs. As it took just 65 crore rupees (approximately $11.9 million USD) to build a BSL-4 lab, India should establish such labs in every state. Covaxin vaccine could only be produced at BSL-3 laboratories, but India has only a few such labs. To remedy this, at least 6% of our GDP should be invested in the next 10 years, for creating and developing health infrastructure instead of the present allocation of a mere 1.5%. India is among the countries with the lowest public healthcare budget in the world. Except for few states like Kerala and Tamil Nadu, many states lag behind the creation and spread of physical facilities such as hospitals and laboratories. Tamil Nadu’s ‘Amma Clinics’ and Delhi’s Mohalla clinics are the ways to go. As of now establishing small and medium level hospitals in every ward of the country should be the priority rather than building big, splashy AIIMS.
All states must have a separate and dedicated facility for the mass production of PPE kits and vaccines. HLL, a government subsidiary vaccine complex in Chengalpet, has not been operational for the past nine years even after the completion of the construction. Even private sectors can’t help the government during a crisis; hence, India needs real self-sufficiency in this matter. The global ban on some materials that are essential for vaccine production has derailed India’s massive vaccine-producing goals. The Union and state governments must invest in producing such basic materials, raw materials, and miscellaneous tools in India itself either by the private sector or by a government body.
Logistics plays a crucial role in handling any health crisis, let alone a pandemic. The horrific second wave of Covid-19 in India witnessed the accelerating need for liquid oxygen and the herculean task of providing them from one corner of the country to another. There is a need for a separate and dedicated logistics agency to aid NCDC to trace, track, and supply resources across India. India needs a centralized control room at both Union level and State level, GPS tracking of ambulances and medical supplies, a transparent information portal such as a dashboard in websites with impeccable software. When Delhi and the heartlands of India struggled to create such a dashboard, southern states like Kerala, Tamil Nadu and Karnataka had them from day one.
While governments across the globe are graduating their final year MBBS and Nursing students early so that they can replenish their health professional forces, India is setting up tougher entrance exams, which scares off the talents. Therefore, entrance examinations are clearly not the way to eliminate unqualified doctors. Strict enforcement of end-semester examinations in MBBS or nursing exams will do that. Both 100% external invigilation and 100% external evaluation in theory and lab exams will ensure the undeserving students leaving the field without degrees. In simpler terms, instead of stopping the inflow of talents, India should focus on standardizing the outflow of the talents. Students pursuing medical degrees from foreign countries should be allowed to practice medicine in India without any additional examinations as well. Now is the time for pragmatic changes, not frivolous gimmicks.
These pieces are being published as they have been received – they have not been edited/fact-checked by ThePrint.


COMMENTS