New Delhi: “I want another life,” Deepak Roshan, 29, says. “Maybe a dog’s.” The object of his envy, Lucy, wags her tail slightly as she stands on the bed where he lies immobile. His mother oils his legs. It won’t cure him, just as years of surgery and physiotherapy haven’t, but it’s a kind of comfort, like the painkillers and protein packets he gets from the palliative care team that visits his home.
When there is no hope of a cure and living in pain is unavoidable, trying to prolong life can feel like cruelty, but there is something to be said about making whatever’s left of it easier, or at least more bearable.
Many people are in a long and slow process of dying in India — from cancers, complications from serious injuries, neurological diseases like Alzheimer’s or Parkinson’s. Like in any growing economy, people are living longer but this doesn’t necessarily mean they are living better.
With access to healthcare and technology, there is an increasing emphasis on clinical interventions and treatments, but in many cases, all they do is stave off death, often at the cost of quality of life.
But a growing voice from within the medical community is pushing for a move away from hospital-based invasive treatments in the last days of life, or in cases where a cure is impossible.
The alternatives, say doctors and civil society organisations working in this sector, are palliative and hospice care, both of which focus on the cessation of pain and discomfort.
Palliative care places emphasis not on ‘cure’ but on relief from physical, psychological, and emotional suffering, not only for the patient but also for their family. It can be extended alongside medical treatments.
Hospice care, on the other hand, implies ceasing treatment, except for palliative care, soon before death is expected to occur.
While palliative care is often associated with cancer where treatments may not work after a point, its need for patients suffering from other illnesses and disabilities is slowly being recognised.
But with limited reach and awareness about palliative and hospice care, many patients find themselves caught in an unnecessary and futile ‘battle’ with their medical conditions, which makes death less peaceful than it could be for them and their loved ones.
Also Read: Only 8 Ayushman Bharat packages cover care for terminally ill patients, govt analysis finds
A better quality of death
In the chaotic outpatient department of AIIMS cancer hospital, Deepa Chuphal is patiently waiting in queue to get a dose of morphine for her five-year-old niece, Prisha Adhikari. When Prisha was two years old, she was diagnosed with a tumour in the brain and within six months, the cancer spread to her body.
“Earlier, doctors gave us hope, but now we are just counting down the days,” Chuphal says, her eyes moist.
Not long after her diagnosis, little Prisha was referred to the pain management department of the cancer hospital where the focus of the doctors has been to relieve her of pain until she breathes her last.
“When patients are in chronic conditions and cure is not possible, then we see that there is an information crisis among patients and relatives. They don’t know anything about the disease and the treatment options. They feel that we are only doing symptomatic treatment,” says Dr Sushma Bhatnagar, head of onco-anaesthesia and palliative medicine at the All India Institute of Medical Sciences (AIIMS) in Delhi.
She says doctors need to inform families about holistic care to help them come to terms with the situation and begin their emotional healing.
“We not only treat the patients’ symptoms but also take care of the family members. Palliative care is the only branch of medicine that offers care to caregivers,” she adds.
According to Roop Gursahani, a neurologist and an advocate of advance care planning, patients should also be empowered to make decisions about their care when they are in a mental state to do so.
“An ICU is a terrible place to die,” Dr Gursahani says in a webinar on advance life planning. “People should die in their own beds, surrounded by their families.”
In January, the Lancet Commission released a series, Value of Death, bringing attention to how Covid-19 led to people suffering the “ultimate medicalised deaths, often alone but for masked staff in hospitals and intensive care units, unable to communicate with family except electronically”.
The series of papers draw attention to the over-emphasis on aggressive treatments to prolong life, high costs of end-of-life treatments, and global inequities in access to palliative care. A rethink is needed, then, to reshape our relationship with death and how we care about the dying, the papers say.

Also read: The Covid pallbearers — How Indians across religion and caste worked to give the dead dignity
Preparing to say goodbye
Conversations about death are never easy, but not having them causes even more difficulties, according to palliative/hospice care experts.
“We have to bring them face to face with the reality that the patient is not going to get better. But at the same time, we give them the assurance that we will be with them until the end for their every need,” says Pallika (who doesn’t use a last name), a counsellor with CanSupport, which provides free home-based palliative care, mostly to people with cancer.
The first conversation is always the hardest, she says. Families break down and their emotional anguish can be hard to witness — but most people usually accept the outcome, allowing themselves to deal better with the situation.
Many doctors in India are not adequately trained in breaking the bad news in a way that spells out the facts without further traumatising the patient or their family members. While some hospitals do hold workshops on communication skills for doctors, such initiatives are rare.
According to Dr Gursahani, in addition to breaking the news, it is important also to help patients make “living wills”. These help to vest decision-making with patients or the family members they appoint to carry out their last wishes about the kind of treatment they want.
“It’s a simple form where they can list out things that they don’t want. It is clearly stated that if you choose to refuse a treatment then nobody can force it on you,” explains Dr Gursahani.
The form lists several procedures that people can opt out of when they are at hospital, including artificial respiration, tube feeding, dialysis, and chemotherapy.
“It’s a painful process, but all of us must do it,” he says.
The lack of communication and planning about such options puts many patients and families in a difficult situation when it comes to deciding how long the treatment should continue.
Palliative care in India
Although the need for palliative care is widely recognised, less than 2 per cent of people in need have access to it in India. With the exception of Kerala, where palliative care is community-driven, decentralised and supported by the state government, the services provided in the rest of the country are patchy at best.
While a few NGOs work in collaboration with hospitals to help provide home-based care, they are still generally seen as dispensing a charitable service.
At AIIMS, palliative care has been given to patients for a long time, but a dedicated department started only in 2016, which is when a specialised MD degree in palliative care was also introduced. In India, there are less than 100 trained physicians who specialise in this field and it is still focused on pain management in cancer patients.
“Worldwide, palliative care and cancer are hooked to each other. The main issue is pain [management]. But if you put a number to the suffering of a patient with Parkinson’s disease in the last two-three years of their lives, it’s the same as a cancer patient’s,” Dr Gursahani says.
Then there are cases like Deepak Roshan’s — debilitating, incurable, but not necessarily terminal. In such instances, too, palliative care can be an alternative to cure-oriented treatments.
The NGO CanSupport caters to such patients too, free of cost, in their daily roster of home visits. The team also offers support to caregivers who struggle managing the needs of the patient when the rest of the medical establishment has given up.
Also Read: Global life expectancy has risen by 43 years, but it’s more time living in poor health
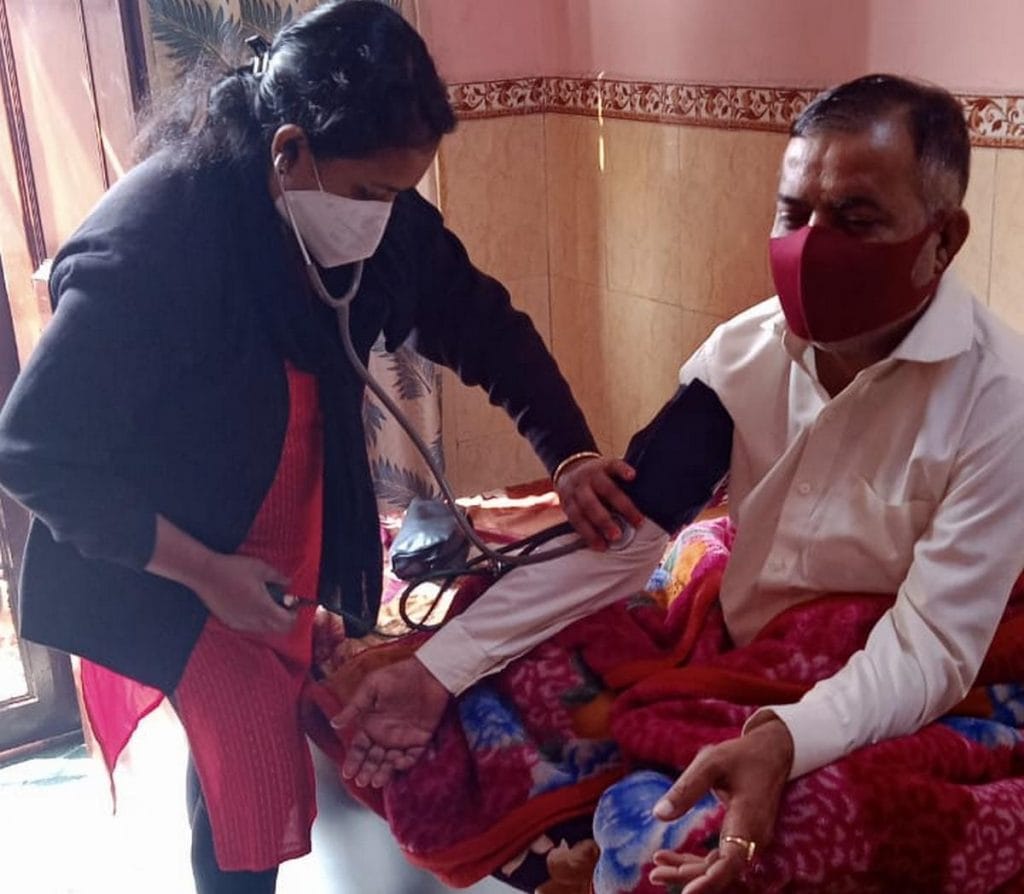
Home-based palliative care for long-term conditions
Eleven years ago, when he was 18 and high on life, Deepak Roshan decided to take a dive in a river in his father’s village in Bulandshahr, Uttar Pradesh. “I felt a spark in my whole body as my head hit the riverbed. I wanted to swim, but I kept drifting away in the water. I haven’t felt anything since then,” he says.
That was the moment when the C5 bone in his neck snapped. He would never drive his tempo again or enjoy his favourite activity of watching movies in a cinema hall. For almost a year after the accident, Deepak was confined to the hospital, until one day the doctors said there was nothing more they could do. He could go home. He was young, maybe his body would spontaneously regain movement.
But, home — a single-room house in Ghaziabad — meant even more discomfort. With her limited income, his mother and primary caregiver Poonam could not afford the right kind of mattress or an air conditioner, and Deepak soon developed bed sores.
While scrambling to get him help, Poonam came in contact with CanSupport. With a team of a doctor, nurse, and counsellor visiting them regularly to help manage his condition, Poonam and Deepak have come to accept he may never be mobile again.
Life is still difficult, of course.
“I want to get rid of this body,” he says at one point, looking down at his wasted muscles and skin mottled with the scars left by bed sores.
Deepak gets restless in the afternoon heat. Every ten minutes, Poonam has to turn to his side, straighten his curved legs, and grip them hard to stop the convulsions.
When the palliative care team visits, both mother and son feel a sense of relief. The team hands out basic medicine, cleans Deepak’s catheter, and talks to both of them about how they are doing.
Deepak, who admits he is lonely despite his constant companions — his dogs Lucy and Tuffy — shares things with the team that he feels reluctant to with his mother.
Yet, Deepak and Poonam both still hope that one day he will get better and be able to walk again. They are waiting for a miracle, but until then, at least they have some respite from suffering.
(Edited by Asavari Singh)






