Manjula Rao died 14 months after she was bitten by a venomous snake. Over the course of that period, she was treated by multiple hospitals and local healers until the day she passed away. By then, her family was drowning in a debt of over Rs 16 lakh. “This is just one story of an individual whose family was driven into poverty and debt due to a snakebite, but the true scale of the population affected, the mental, financial and socio-economic impact that snakebite has on lakhs of families in India is potentially monumental and unaccounted for,” says Sumanth Bindumadhav, acting country director at the Humane Society International/India who has been actively working on management of human-snake conflict in India for over a decade.
Mostly a rural problem, snakebite envenoming is an acute life-threatening and neglected tropical disease (NTD). Data from a 2020 national mortality study shows that 94 per cent of snakebites occur in rural areas and 77 per cent of the deaths occur outside the hospital.
Families of daily wage workers and farmers in India face the greatest threat of being driven into poverty when a member of the household succumbs to a bite. The cruel reality is that it might be worse if the snakebite victim survives and is left to deal with the morbid aftermath: Physical disabilities, a lifetime of dependency and care, and compounding medical bills.
Also Read: ‘To live is to kill’ — a Malabar pit viper and gliding frog affirm nature’s basic law
Snakebite envenoming effects
Envenoming, a body getting poisoned by snake venom, can cause acute local and systemic effects depending on the toxicity of the venom and the location of the bite. Some who receive timely medical care may get away with minor tissue injuries, swelling, pain and blistering. However, in most cases, it is the lack of initial response to snakebite that causes severe problems.
Those who don’t take snakebites seriously enough go to local healers or indulge in superstitious practices. Success stories of local healers are rampant, and experts in the field offer an insight as to why that is the case. “If a local healer claims that they have an 80 per cent success rate, it can be attributed to the fact that eight out of 10 bites are possibly dry bites (a bite without venom being injected) or bites where a very small amount of venom entered the body,” says Romulus Whitaker, India’s most acclaimed herpetologist and founder of the Madras Crocodile Bank Trust.
Bindumadhav adds that in more severe cases when treatment has been delayed or inadequate, partial or complete limb amputations are an unfortunate and common outcome. “In the long term, survivors of snakebite are known to suffer a gamut of issues ranging from musculoskeletal disabilities, chronic wounds, kidney damage, loss of body parts, blindness and mental health-related issues rendering the victim unproductive or with a greatly compromised ability to contribute to the gross household income.”
Also Read: Indian Mouse Deer’s status as ‘Lowest Risk’ is worrying. Look at full picture first
The scale of the problem
The actual number of snakebite-related fatalities is debatable but any individual actively working in this field will tell you that it is a figure that is generally underreported. “First, because most people are worried about going to hospitals and the cost associated with it. Second, these cases are not recorded or reported, as snakebite is not a notifiable disease in India,” says Gerry Martin, founder of The Liana Trust based in Karnataka.
Based on the Million Death Study, an initiative by the Registrar General of India and the Centre for Global Health Research at St. Michael’s Hospital and the University of Toronto, India reports approximately 58,000 deaths per year. Nearly 50 per cent of the victims fell between the ages of 30 and 69. “While the study estimates how many people have died from snakebite, the number of snakebite survivors that are currently leading physically compromised lives and their families who are heavily burdened with financial debt is probably far higher,” adds Martin.
While a few states in India do offer compensation to families of snakebite victims, the amount offered and lengthy process of accessing these funds is a major deterrent.
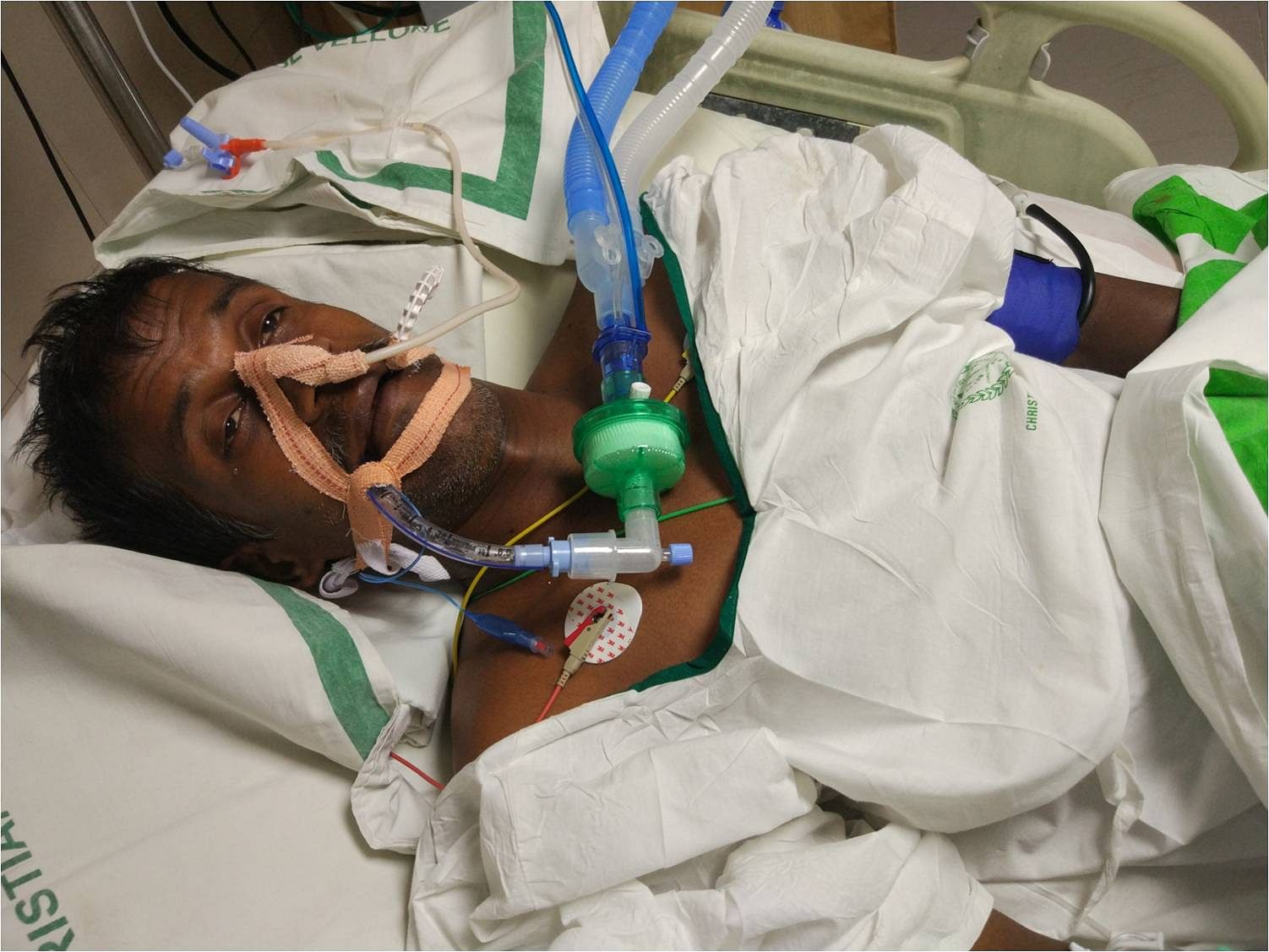
Ensuring a snakebite victim quickly accesses a medical facility to receive treatment is merely one hurdle. “Several hospitals, especially in rural areas, do not have a reliable supply of anti-venom available nor a proper storage facility for it. Even if they do, most doctors lack the training in administering the anti-venom dose correctly or managing the life-threatening anaphylactic reaction that may result from administering anti-venom. Most doctors are not updated about the latest snakebite treatment protocol published and circulated by the Government of India based on the guidelines provided by the World Health Organisation,” says Bindumadhav.
Other factors like intra-species variation of venom in different geographies of India also complicate the treatment of snakebites. Currently, there are seven pharmaceutical laboratories in India that produce antivenom to combat the venom of four medically important snake species: Spectacled cobra, common krait, Russell’s viper, and saw-scaled viper. Almost all the venom required for the production of the anti-venom in the country is sourced from Chennai.
Considering there are four species of cobra (Naja), eight species of kraits (Bungarus) and two distinct sub-species of saw-scaled viper (Echis Carinatus) found in different geographical locations in the country, the anti-venom solely sourced from South India may not be effective in treating all snakebites.
Martin says that “at least six different collection locations across the country are potentially required to ensure that the anti-venom produced and administered by medical professionals in hospitals is effective to prevent morbidity and mortality of snakebite victims.”
The government and NGOs are attempting to address this. In 2020, the Indian Council of Medical Research constituted a National Task Force to research snakebites in India and initiated a program to build capacity for the healthcare system. The NGO, Indian Snakes, lists directories of hospitals where snakebite treatment can be availed across the country.
Also Read: Orphaned and exposed, why these Indian leopard cubs can’t return to the wild
The way forward
The long-term chronic effects of snakebite and the economic burden associated with it are critical components of the poverty cycle that mandate attention from policymakers and executives. Our healthcare systems need to be more responsive and accommodate the needs and circumstances of the survivors of snakebites and their families.
While our healthcare systems need to develop a holistic approach to managing snakebites, Whitaker says that prevention is the first step. “The world is very focused around the idea of a next-generation ‘cure-all’ anti-venom. Undoubtedly, a good quality anti-venom that is effective pan-India is very important and I am certain the ongoing research is going to make this a reality soon.”
He stressed the importance of educating people on how to prevent snakebites and correctly respond. “I strongly believe that a lot more support from the government needs to be channelled into funding community-driven outreach and education initiatives where the mass of our people needs to hear it from those whose lives are affected by snakebites. When a message goes out ‘from the people’ who were really affected ‘to the people’ who can relate to them, it may truly make a difference.”
Neha Panchamia is Founder and President, RESQ Charitable Trust. She tweets @NehaPanchamia. Views are personal.
(Edited by Srinjoy Dey)