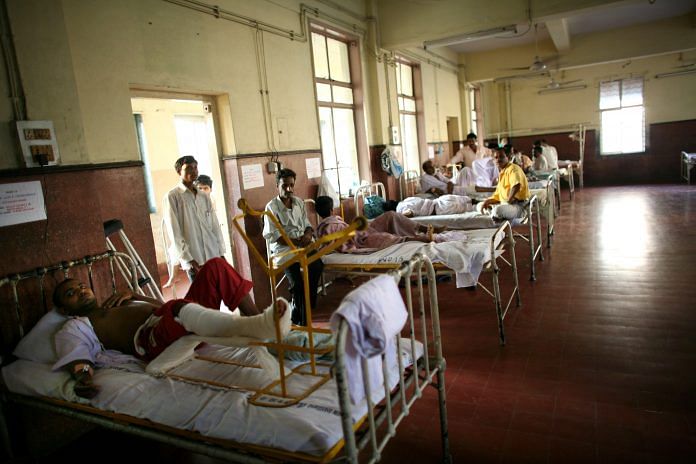
Government to fine insurance companies for delayed payments to hospitals but will not budge on demand for higher rates for procedures.
New Delhi: With just weeks left for the launch of the ambitious insurance-based healthcare scheme Ayushman Bharat, the Modi government is racing against time to ensure the success of a welfare programme with a high potential for political gain.
It has decided to fine insurance companies that delay payments and take away their power to reject claims, hoping to win back big private hospitals that had decided not to participate citing the hassles they said they face in dealing with insurance firms.
But it has also run into a wall, with some top private hospitals and the largest body of practicing doctors in the country rejecting the rates for various procedures announced under the scheme. They want higher payments before agreeing to enlist.
The government said that it won’t budge on the rates, at least not before the scheme is launched by Prime Minister Narendra Modi, most likely on 15 August, Independence Day.
The scheme, popularly referred to as ‘Modicare’, is expected to figure high on the Modi government’s 2019 re-election campaign. Touted as the world’s largest national health insurance scheme, it promises to ease the healthcare burden of India’s poor who struggle with high costs.
The scheme assures a health insurance cover of up to Rs 5 lakh per family every year to 50 crore poor and vulnerable persons, to start with.
But as ThePrint reported exclusively last month, at least 2,000 super-speciality hospitals had decided against being part of Ayushman Bharat.
The hospitals had cited poor reimbursement rates and pending dues under the existing insurance-based government healthcare scheme — the Central Government Health Scheme (CGHS).
One per cent fine
Hoping to address this concern, the Centre has directed insurance companies to settle claims of hospitals within two weeks, failing which they will face a fine of 1 per cent of the original amount, for every week of delay.
The government has also decided that state governments will have the final say on accepting or rejecting claims from hospitals, effectively taking away the authority from insurance firms.
“In an attempt to create a hassle-free model unlike CGHS, the insurance companies under the new scheme will be slapped with a fine of 1 per cent every week if they fail to clear the claims of the hospitals within two weeks,” Indu Bhushan, CEO of Ayushman Bharat, told ThePrint.
“In turn, insurance companies will receive money from the government seamlessly. Under the initiative state governments will be barred from using the scheme’s money for any other purpose. The money will be saved in escrow accounts,” Bhushan said.
On the government taking away the authority of rejecting claims from insurance companies, Bhushan said, “Insurance firms benefit if they reject a claim. Under the scheme, state governments are the final authority in deciding whether the claim should be rejected or not.”
Insurance Regulatory and Development Authority, an autonomous and statutory body tasked with regulating and promoting the insurance industry in India, has accepted the clauses, Bhushan added.
‘Cash-flows choked’
According to the Association of Healthcare Providers, India (AHPI), which represents 2,500 speciality and 8,000 smaller hospitals, hospitals are still owed over Rs 400 crore under the CGHS scheme, which provides free healthcare to central government employees.
Hospitals blame the scheme for choking their cash-flows and are hence hesitant to participate in Ayushman Bharat, which is a similar insurance-based scheme.
While the government has moved to address the problems hospitals face with insurance firms, the hospitals are still simmering with discontent. They point out that the government hasn’t addressed the rate for medical procedures, one of the reasons they are still reluctant to join the scheme.
Under the scheme, the treatment for various procedures including coronary bypass, knee replacements and stents would be provided at rates which are 15-20 per cent than CGHS.
“CGHS lacks professionalism. We appreciate the attempt to not repeat the mistakes under CGHS. However, we are still not convinced with the proposed rates of treatments under the scheme,” said Girdhar J. Gyani, director general, AHPI.
Naresh Trehan, chairman and managing director, Medanta, said: “The rates, which the government has offered, are not realistic. They haven’t calculated our overhead expenditures. We are ready to support that initiative but the scheme rates are just not doable.”
Trehan is not alone. More than 2,000 hospitals, including Sir Ganga Ram Hospital, Fortis Healthcare, Apollo Hospitals and BLK Super Speciality Hospital have refused to participate under the scheme.
AHPI got a shot in the arm last weekend when the Indian Medical Association (IMA), the largest body of practicing doctors in the country, backed it and rejected the rates announced under Ayushman Bharat.
“The rates are so low that hospitals will suffer losses. These hospitals are willing to partner with the government provided the package rates are revised to a reasonable level,” said Dr R.N. Tandon, general secretary, IMA.
Govt firm on rates
However, the government has decided to not pay heed to the demands of the IMA and the super-speciality hospitals.
According to the estimates of NITI Aayog, these hospitals comprise just 3 per cent of total hospitals in the country. Over 85 per cent of health service delivery centres are single doctor clinics in India. The other 12 per cent are hospitals with 10 to 50 beds.
“We have taken the cost of procedures from over 100 hospitals of all categories and finalised the median rates scientifically. We cannot increase the reimbursement prices due to the cost of fancy environment,” said Alok Kumar, health advisor at NITI Aayog.
However, under certain circumstances hospitals can earn a bit more.
For instance: If a hospital is accredited with the National Accreditation Board for Hospitals (NABH), it can add 10 per cent more to the base rate; hospitals providing PG courses can add another 10 per cent to the base rate; hospitals in the 115 backward districts can add yet another 10 per cent.
“The rates are now final,” said Bhushan. “The states have the authority to tweak the charges within a specified limit but price setting at the national level will now be done in the later stages.”
“We won’t revise the prices at least until the launch of the scheme. We have addressed the key issues including timely payments to hospitals, strict clauses on insurance firms, and ease of setting up of IT infrastructure,” Bhushan said. “The prices of procedures are derived scientifically and we are confident they do not compromise on patient’s safety.”