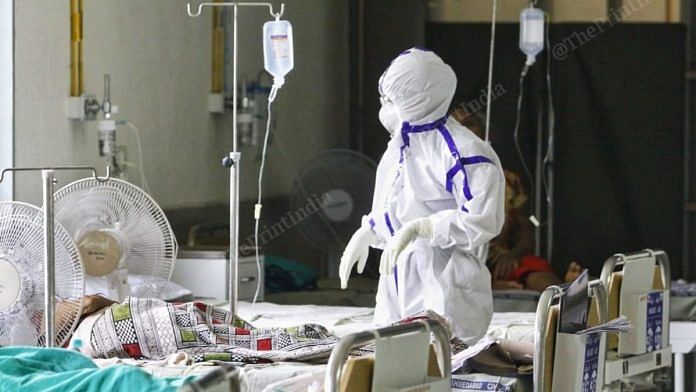
New Delhi: The Covid-19 pandemic has left India grappling with a major problem — dealing with tonnes of waste that also constitutes a transmission hazard if not segregated and disposed of properly.
As of Monday, India had registered over 60 lakh cases of coronavirus. Given the highly infectious nature of Covid-19, the pandemic has led to a surge in the use of personal protective equipment (PPE), and its individual components such as face masks and gloves, by healthcare and testing lab staff as well as patients.
Once disposed of, these items are treated as biomedical waste, and tonnes of it are being thrown out every day by hospitals, labs, quarantine centres and households with Covid patients.
Before Covid-19 times, India produced an average of 609 metric tonnes of biomedical waste (BMW) per day. This number jumped to 710 metric tonnes per day in June, and stood at 778 metric tonnes as of August, according to the ‘Covid-19 BMW’ app launched by the Central Pollution Control Board (CPCB) that tracks the movement of biomedical waste from its generation to disposal.
CPCB estimates suggest India has the capacity to incinerate 840 metric tonnes of biomedical waste per day. Incineration is one of two ways biomedical waste is tackled, the other being autoclaving or sterilising the waste at high temperatures and recycling it.
Going by CPCB figures, India has the capacity to handle the biomedical waste being churned out amid the Covid-19 pandemic. However, the authorities find their efforts hampered by a lack of awareness about waste segregation for effective disposal.
In August, the Supreme Court made it mandatory for all urban local bodies to download and use the Covid-19 BMW app so biomedical waste can be properly accounted for and disposed of.
Over 5,000 waste generators across the country, such as hospitals, quarantine centres, testing labs are registered with the app. But the amount of Covid-related waste that is being mixed with general solid waste is unknown.
“A major issue is collection from households. Most houses don’t follow segregation at source. PPE and masks should never go into municipal waste, and should be kept separate for at least 72 hours before disposal,” said Swati Singh Sambyal, a Delhi-based waste management expert. “The key is to be more disciplined with segregation.”
Also Read: Delhi to Vijayawada, India has started dumping Covid-19 infected waste in public places
How biomedical waste is collected
According to the Biomedical Waste Rules of India, ‘BMW’ is defined as “any waste which is generated during the diagnosis, treatment or immunisation of human beings or animals or in research activities pertaining thereto or in the production or testing of biologicals”.
Biomedical waste is collected from hospitals and other generators by municipalities or private agencies hired by the government. The waste is then taken to a common biomedical waste treatment facility (CBWTF) where the waste is either treated or incinerated.
“In the months of March and April, there was actually a fall in biomedical waste since lots of clinics were closed (during the lockdown) and few patients were coming to hospitals. It began to pick up in June,” said Satish Sinha, associate director of Toxics Links, an environmental justice organisation based in Delhi.
Data from the CPCB shows India produced 3,025 metric tonnes of Covid-related biomedical waste in June, 4,253 metric tonnes in July, and 5,238 metric tonnes in August. When Covid waste started to mount, there were no clear protocols for how it should be managed, and so all of it was incinerated, say CPCB officials.
“In April and May, the incineration facilities in big cities were running nearly at full capacity because they were burning all waste touched by a Covid-19 patient, including food waste and cutlery,” said an official from the CPCB’s biomedical waste department.
Since March, the CPCB has revised its Covid waste-handling guidelines four times to account for various provisions. “We were making the guidelines as the pandemic spread,” the official added.
It wasn’t until June that specific guidelines on how to segregate Covid waste from general solid waste were made clear. The fourth iteration of the guidelines, released in July, specify how caregivers and municipalities should treat waste from Covid wards, quarantine centres, testing labs, and homes.
With rising cases — particularly asymptomatic carriers — there are concerns about whether disposable waste generated in houses could be a potential source of infection.
The CPCB does not consider disposable masks from households without a Covid patient as biomedical waste. However, guidelines for their disposal do exist, even if they are not widely known.
“Most people don’t know about the guidelines in place for the masks they throw away. Because they could be a potential source of infection, they have to be kept aside for 72 hours, cut up, and only then disposed with dry solid waste, which can be taken by the municipality,” the official said.
Unsegregated waste, the official added, are a particularly major concern from quarantine centres and households.
If protocols aren’t followed, it’s sanitation workers who are most at risk of contracting the virus by handling waste that hasn’t been properly segregated or disposed of. The Supreme Court’s decision to make the CPCB’s app mandatory was driven, in part, by this.
“The biggest leakage is from unsegregated waste that goes in with the regular municipal waste that is collected from the door. The only way out is to spread awareness on the importance of segregation,” said Sambyal.
Dr B. Venkatesh, who manages biomedical waste for the East Delhi Municipal Corporation, said they are trying to do their best to properly segregate waste.
“The general public is using masks and gloves, and it has been advised that they follow the guidelines, but it isn’t always the case that they do,” he added.
“We have issued a circular to all our officers telling them they need to follow these guidelines, but we haven’t for the public yet. We’re trying our best with it,” he said.
Also Read: Let’s talk about garbage in Covid battle and clap for India’s sanitation workers
‘No capacity issue’
Once collected, Covid waste is either burned at 1,200 degrees, or autoclaved, which means it’s put into a large microwave and sterilised at a high temperature, before being shredded or recycled. Colour-coded bags determine the fate of the waste inside.
Non-plastic PPE kits worn inside Covid wards, masks worn by patients, and other materials containing bodily fluids are examples of waste put in yellow bags and sent to burn. Plastic face shields, coveralls, and gloves go into red bags that can be autoclaved.
“Before the guidelines made it clear, we got a lot of mixed waste which made processing the waste very difficult,” said the CPCB official quoted above.
There are 198 CBWTs across India, with a capacity to incinerate 840 metric tonnes per day. India is already producing 778 metric tonnes, but treatment capacity isn’t an issue.
“Big cities have more than enough capacity to deal with the waste. There isn’t a problem there,” said Sinha, adding, “The problem in big cities is that the groundwork is not being done properly, such as distribution of colour-coded bags door to door or awareness for waste segregation.”
The official at the CPCB agreed, saying, “Not all the waste has to be incinerated, so we’re still using a little over 50 per cent of the capacity. The problem lies in places that don’t have waste treatment facilities — we must turn our attention to those places.”
The states of Tripura, Mizoram, and Goa, the official said, don’t have waste processing facilities, and must either bury their waste deep into the ground or send it to the nearest processing facility.
Also Read: Today’s PPE kits could be tomorrow’s roads, fuel — CSIR’s plan to tackle Covid plastic surge