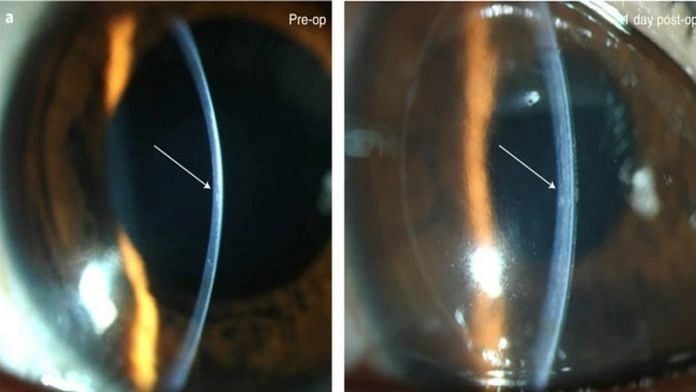
Bengaluru: A cornea implant made from pig skin collagen has enabled 20 volunteers suffering from corneal blindness to see again in a pilot trial. The trial was designed and conducted by researchers from Sweden’s Linköping University, and took place at AIIMS, Delhi, and Farabi Eye Hospital, Iran.
The volunteers were implanted with a biosynthetic cornea that uses medical-grade collagen — a protein found in tissues, skin, and bone which provides structural support and performs tissue repair — extracted from pig skin, facilitating an easy and sustainable solution to corneal blindness. Every year, more than a million people worldwide lose their vision because of damaged or diseased corneas, but there is an acute shortage of cornea donors.
Details of the latest Phase 1 trial — conducted between November 2016 and June 2022 (including follow-ups) — and its outcome were published on 11 August in the peer-reviewed scientific journal Nature Biotechnology. Phase 2 of the trial is ongoing, with up to 40 volunteers being recruited.
More than a decade ago, researchers from Linköping University had shown through their work how biosynthetic corneas can restore vision in humans and address organ shortage. The latest procedure is also minimally invasive — instead of removing the existing cornea and replacing it with the new one, surgeons simply make a small incision and insert the biosynthetic pig collagen cornea.
The bioengineered corneas do not utilise human tissue and can potentially be mass produced in the future with improved storage capabilities. The trial volunteers reported no adverse events after the procedure during follow-ups over a period of 24 months.
Also Read: Dedicated teams, cost, facilities — why pvt hospitals do over 75% of organ transplants in India
Disproportionate corneal blindness in low, middle income nations
Loss of corneal function is one of the leading causes of blindness in the world, and is treatable by transplantation. However, a severe shortage of cornea donors means that only 1 in 70 people who need one have access to it, as of 2016.
Additionally, the donor shortage has a larger consequence in low- and middle-income countries (LMICs), where there are disproportionate cases of untreated corneal blindness due to lack of access to extremely invasive and expensive transplant procedures.
The main indicator of a patient requiring a transplant is keratoconus — the thinning, scarring, and weakening of cells in the cornea. Keratoconus is widely prevalent around the world, with 30 million people in India affected by it at present. It is genetically also likely to be more prevalent among Asian populations than white Caucasians.
Furthermore, there are threats to existing corneal tissue available for transplant as well. For example, there is also an increased risk of regular pandemics in today’s world as well as the spread of antimicrobial-resistant superbugs, which has spurred research into bioengineering tissue for cornea transplants or regeneration.
Cell-free implantable medical device in place of corneal tissue
In the latest trials, the researchers bioengineered a cell-free implantable medical device as a substitute for corneal tissue. The material is made up of natural type I collagen, the main protein in the human cornea, sourced from porcine skin.
This collagen is already medical-grade and approved by the US Food and Drug Administration (FDA), and is a purified byproduct from the food industry. The researchers used a new method to physically structure the material into a hydrogel, improving its strength and stability.
The outcome of the procedure was eventual corneal thickening, restoring corneal shape, and rapid healing of wounds and scars, the researchers found. The Phase 1 trial involved a small number of volunteers and continuous testing and monitoring for safety.
Why pigs?
Pigs are proving to be a popular choice for xenotransplantation — the process of transplanting animal organs into humans. Their organs and physiology are very similar to humans, and humans also have centuries of knowledge about pigs.
They also grow quickly in labs and their organs can mature to transplantable sizes within a few months. They are also easy candidates for genetic modifications to make their organs more suitable for human bodies.
The FDA-approved medical grade collagen from pig skin is already regularly used in glaucoma surgeries, as well as for grafting skin after burns. Pig heart valves have also been used in humans for over two decades.
In the past year, there have been numerous breakthrough advances in using pig organs and tissues, including transplanting pig kidneys and hearts into humans.
Pigs are thought to be the most promising candidate for generating biomedical solutions that can address the acute organ shortage that plagues global healthcare today.
(Edited by Gitanjali Das)
Also Read: 175 dogs guard Assam’s pig heart doctor who bangs desk to speak. Patients still lining up